Pyloric stenosis
•Download as PPTX, PDF•
30 likes•14,900 views
Pyloric stenosis is a condition where the pylorus, the opening from the stomach to the small intestine, becomes narrowed due to muscle thickening. This causes projectile vomiting after feeding as food cannot pass easily into the intestines. It typically affects young infants under 3 months of age. Treatment involves a pyloromyotomy surgery to cut the thickened muscle and allow food to pass through.
Report
Share
Report
Share
Recommended
PYLORIC STENOSIS.pptx

PYLORIC STENOSIS
Pyloric stenosis is a medical condition in which the pylorus, the muscular valve between the stomach and the small intestine, becomes abnormally narrowed or obstructed, leading to the obstruction of the gastric outlet. This narrowing of the pylorus prevents the proper passage of food from the stomach to the small intestine.
The exact cause of pyloric stenosis is still unknown, but it is believed to have a multifactorial etiology.
Genetic factors are thought to play a role, as there is a higher incidence of pyloric stenosis among siblings and family members.
Environmental factors may also contribute to the development of the condition, but specific triggers remain unidentified.
The hallmark symptom of pyloric stenosis is projectile vomiting, which occurs shortly after feeding.
Vomitus is often non-bilious and may resemble curdled milk.
Forceful vomiting that may project several feet away from the infant.
Signs of hunger and irritability despite frequent feeding attempts.
Weight loss or poor weight gain.
Dehydration and electrolyte imbalances due to excessive vomiting.
Palpable “olive-shaped” mass in the epigastric region.
Infants appear hungry, irritable, and unsatisfied after feeds.
Physical Examination:
Palpation of the abdomen may reveal a palpable “olive-shaped” mass in the epigastric region, which represents the hypertrophied pylorus.
The “olive” can often be felt when the infant is in a relaxed state and the stomach is empty.
Abdominal Ultrasound:
Abdominal ultrasound is the primary diagnostic tool for confirming pyloric stenosis.
Fluid and Electrolyte Management:
Prior to surgery, infants with pyloric stenosis often require fluid resuscitation and correction of electrolyte imbalances caused by excessive vomiting.
Intravenous hydration and electrolyte replacement may be necessary to restore the infant’s fluid and electrolyte balance.
Atropine Therapy:
In some cases, medical management with intravenous atropine may be attempted as a temporary measure to relieve pyloric spasm and improve the passage of food.
Surgical management of pyloric stenosis involves performing a pyloromyotomy.
This procedure is typically done under general anaesthesia and can be performed as an open surgery or laparoscopically.
Postoperative Nursing Care:
Monitor vital signs, surgical site, and signs of infection, such as fever, redness, swelling, or discharge.
Administer prescribed pain medications and antibiotics.
Observe for complications, such as bleeding or infection, and report any abnormalities to the healthcare team.
Encourage early feeding and monitor for successful feeding tolerance, ensuring the infant is retaining and digesting food properly.
Educate parents about postoperative care, including incision care, feeding techniques, and signs of potential complications, emphasizing the importance of follow-up visits and ongoing care.
Pyloric stenosis

PYLORIC STENOSIS:
Review the anatomy and physiology of digestive system
Review the incidence of pyloric stenosis
Define pyloric stenosis
Explain the causes and risk factors of pyloric stenosis
Describe the pathophysiology of pyloric stenosis
Enumerate clinical features of pyloric stenosis
Enlist the diagnostic evaluation for pyloric stenosis
Explain the management of pyloric stenosis
Enumerate the complications of pyloric stenosis
Exstrophy of bladder 

Bladder exstrophy is a congenital (present at birth) abnormality of the bladder. It happens when the skin over the lower abdominal wall (bottom part of the tummy) does not form properly, so the bladder is open and exposed on the outside of the abdomen. In epispadias, the urethra does not form properly.
Intestinal obstruction in children ppt

Intestinal obstruction in children pptProf.Dr.Shali.B.S.Mamata College of Nursing,Khammam,Telangana.
Intestinal obstruction pptRecommended
PYLORIC STENOSIS.pptx

PYLORIC STENOSIS
Pyloric stenosis is a medical condition in which the pylorus, the muscular valve between the stomach and the small intestine, becomes abnormally narrowed or obstructed, leading to the obstruction of the gastric outlet. This narrowing of the pylorus prevents the proper passage of food from the stomach to the small intestine.
The exact cause of pyloric stenosis is still unknown, but it is believed to have a multifactorial etiology.
Genetic factors are thought to play a role, as there is a higher incidence of pyloric stenosis among siblings and family members.
Environmental factors may also contribute to the development of the condition, but specific triggers remain unidentified.
The hallmark symptom of pyloric stenosis is projectile vomiting, which occurs shortly after feeding.
Vomitus is often non-bilious and may resemble curdled milk.
Forceful vomiting that may project several feet away from the infant.
Signs of hunger and irritability despite frequent feeding attempts.
Weight loss or poor weight gain.
Dehydration and electrolyte imbalances due to excessive vomiting.
Palpable “olive-shaped” mass in the epigastric region.
Infants appear hungry, irritable, and unsatisfied after feeds.
Physical Examination:
Palpation of the abdomen may reveal a palpable “olive-shaped” mass in the epigastric region, which represents the hypertrophied pylorus.
The “olive” can often be felt when the infant is in a relaxed state and the stomach is empty.
Abdominal Ultrasound:
Abdominal ultrasound is the primary diagnostic tool for confirming pyloric stenosis.
Fluid and Electrolyte Management:
Prior to surgery, infants with pyloric stenosis often require fluid resuscitation and correction of electrolyte imbalances caused by excessive vomiting.
Intravenous hydration and electrolyte replacement may be necessary to restore the infant’s fluid and electrolyte balance.
Atropine Therapy:
In some cases, medical management with intravenous atropine may be attempted as a temporary measure to relieve pyloric spasm and improve the passage of food.
Surgical management of pyloric stenosis involves performing a pyloromyotomy.
This procedure is typically done under general anaesthesia and can be performed as an open surgery or laparoscopically.
Postoperative Nursing Care:
Monitor vital signs, surgical site, and signs of infection, such as fever, redness, swelling, or discharge.
Administer prescribed pain medications and antibiotics.
Observe for complications, such as bleeding or infection, and report any abnormalities to the healthcare team.
Encourage early feeding and monitor for successful feeding tolerance, ensuring the infant is retaining and digesting food properly.
Educate parents about postoperative care, including incision care, feeding techniques, and signs of potential complications, emphasizing the importance of follow-up visits and ongoing care.
Pyloric stenosis

PYLORIC STENOSIS:
Review the anatomy and physiology of digestive system
Review the incidence of pyloric stenosis
Define pyloric stenosis
Explain the causes and risk factors of pyloric stenosis
Describe the pathophysiology of pyloric stenosis
Enumerate clinical features of pyloric stenosis
Enlist the diagnostic evaluation for pyloric stenosis
Explain the management of pyloric stenosis
Enumerate the complications of pyloric stenosis
Exstrophy of bladder 

Bladder exstrophy is a congenital (present at birth) abnormality of the bladder. It happens when the skin over the lower abdominal wall (bottom part of the tummy) does not form properly, so the bladder is open and exposed on the outside of the abdomen. In epispadias, the urethra does not form properly.
Intestinal obstruction in children ppt

Intestinal obstruction in children pptProf.Dr.Shali.B.S.Mamata College of Nursing,Khammam,Telangana.
Intestinal obstruction pptHirschsprung disease

Its a pediatric disease which is very severe, this content will be useful for the students who pursuing nursing course
Tracheoesophageal fistula

A Tracheoesophageal fistula (TEF) is an abnormal connection (fistula) between the Oesophagus and the trachea. TEF is a common congenital abnormality.
Oesophageal atresia is failure of oesophagus to form a continuous passage from the pharynx to the stomach
TEF is an abnormal connection between the trachea and the oesophagus
Tef ppt new

A Tracheoesophageal fistula is a congenital disease. It is a acquired communication between the trachea and esophagus. Most of the patient with TEF are diagnosed immediately following after birth.TEF are often associated with life threatening complications.
Hyperemesis Gravidarum 

Hyperemesis Gravidarum:
Introduction
Aetiology & Proposed theories
Clinical course
Investigations and management
Ppt tracheo esophageal atresia

introduction, deinition, types, pathophysiology,clinical manifestation, management
More Related Content
What's hot
Hirschsprung disease

Its a pediatric disease which is very severe, this content will be useful for the students who pursuing nursing course
Tracheoesophageal fistula

A Tracheoesophageal fistula (TEF) is an abnormal connection (fistula) between the Oesophagus and the trachea. TEF is a common congenital abnormality.
Oesophageal atresia is failure of oesophagus to form a continuous passage from the pharynx to the stomach
TEF is an abnormal connection between the trachea and the oesophagus
Tef ppt new

A Tracheoesophageal fistula is a congenital disease. It is a acquired communication between the trachea and esophagus. Most of the patient with TEF are diagnosed immediately following after birth.TEF are often associated with life threatening complications.
Hyperemesis Gravidarum 

Hyperemesis Gravidarum:
Introduction
Aetiology & Proposed theories
Clinical course
Investigations and management
What's hot (20)
Similar to Pyloric stenosis
Ppt tracheo esophageal atresia

introduction, deinition, types, pathophysiology,clinical manifestation, management
Esophageal Atresia (EA) and Tracheo Esophageal Fistula (TEF)

Esophageal atresia (EA) is the
congenital malformation that
represent the failure of the esophagus
to develop a continuous passage upto
the stomach
Tracheo esophageal fistula (TEF) is
the congenital malformation where the
trachea and esophagus fails to separate
into distinct structures and a passage is
created between the two.
Pyloric stenosis.pptx

Introduction
• Pyloric stenosis is also known as pylorostenosis or infantile hypertrophic pyloric stenosis. It is the most common cause of intestinal obstruction in infants. It is a form of obstruction in the gastric outlet which means a blockage from stomach to intestine.
• It was First described by Hirschsprung in 1888
• Ramstedt described an operative procedure to alleviate the condition in 1907 – the procedure used to this day to treat pyloric stenosis.
Definition
• Hypertrophic pyloric stenosis is a marked and progressive outgrowth or enlargement of circular muscle fibers of pylorus causing partial or total obstruction of the stomach outlet due to narrowing of lumen.
Anatomy
The stomach sits in the upper abdomen on left side of the body. The top of the stomach connects to a valve called the esophageal sphincter (a muscle at the end of esophagus). The bottom of stomach connects to small intestine.
The stomach is divided into 5 regions:
• The cardia is the top part of the stomach. It contains the cardiac sphincter, which prevents food from traveling back up the esophagus.
• The fundus is a rounded section next to the cardia. It's below the diaphragm (the dome-shaped muscle that helps to breathe).
• The body (corpus) is the largest section of the stomach. In the body, stomach contracts and begins to mix food.
• The antrum lies below the body. It holds food until the stomach is ready to send it to your small intestine.
• The pylorus is the bottom part of the stomach. It includes the pyloric sphincter. This ring of tissue controls when and how stomach contents move to the small intestine.
Incidence
• It is more commonly seen in child with 2-5wks of age.
• 2-9 per 1000 livebirths can be born with this condition.
• Predominant sex: Male > Female (6:1). Males are more prone to get
• Genetic predisposition can be an underlying factor for disease causation.
• Full term babies especially first borne are most commonly affected.
• Death from infantile hypertrophic pyloric stenosis is rare and unexpected; the reported mortality rate is very low and usually results from delays in diagnosis with eventual dehydration and shock.
Etiology
• Idiopathic
• Other factors : *maternal stress especially in third trimester *elevated prostaglandin levels *deficiency of nitric acid *immature pyloric ganglion cells with abnormal muscle innervation.
• In adults, it can occur due to history of peptic ulcer in pylorus region and hypertrophic changes in muscle layer of pylorus.
Risk factors
• Sex. Pyloric stenosis is seen more often in boys — especially firstborn children — than in girls.
• Race. Pyloric stenosis is more common in whites of northern European ancestry, less common in Black people and rare in Asian
anesthesia for obstructed inguinal hernia

anesthetic implication for obstructed inguinal hernia in pediatric patients...
Pyloric Stenosis.pptx

It occurs when the area distal to the pyloric sphincter becomes scarred and stenosed from spasm or edema or from scar tissue that forms when an ulcer alternately heals and breaks down. The patient has nausea and vomiting, constipation, epigastric fullness, anorexia, and, later, weight loss.
tracheo oesophagal fistula gihs

tracheo oesophagal fistula
Definition of TEF
Development
Epidemiology
Anatomical variation
Pathophysiology
Clinical manifestations
Diagnostic evaluation
General management
Surgical management
Nursing management
Tube feeding ( Gavage feeding )

This is pdf file for basic knowledge for nursing care for Gavage feeding in neonatal care in intensive care unit ( ICU ) .
Similar to Pyloric stenosis (20)
Esophageal Atresia (EA) and Tracheo Esophageal Fistula (TEF)

Esophageal Atresia (EA) and Tracheo Esophageal Fistula (TEF)
More from Mahesh Chand
Infection control in intensive care unit

Infection Control In icu,disinfection, sterilization, standard safety measures and prophylaxis
Organization and functions of nursing srvices and education

staffing pattern and levels of staff and services
Chronic Obstructive pulmonary diasese

Definition, causes, S/S tests and Management with emphysema and bronchitis
More from Mahesh Chand (20)
Organization and functions of nursing srvices and education

Organization and functions of nursing srvices and education
Recently uploaded
The Roman Empire A Historical Colossus.pdf

The Roman Empire, a vast and enduring power, stands as one of history's most remarkable civilizations, leaving an indelible imprint on the world. It emerged from the Roman Republic, transitioning into an imperial powerhouse under the leadership of Augustus Caesar in 27 BCE. This transformation marked the beginning of an era defined by unprecedented territorial expansion, architectural marvels, and profound cultural influence.
The empire's roots lie in the city of Rome, founded, according to legend, by Romulus in 753 BCE. Over centuries, Rome evolved from a small settlement to a formidable republic, characterized by a complex political system with elected officials and checks on power. However, internal strife, class conflicts, and military ambitions paved the way for the end of the Republic. Julius Caesar’s dictatorship and subsequent assassination in 44 BCE created a power vacuum, leading to a civil war. Octavian, later Augustus, emerged victorious, heralding the Roman Empire’s birth.
Under Augustus, the empire experienced the Pax Romana, a 200-year period of relative peace and stability. Augustus reformed the military, established efficient administrative systems, and initiated grand construction projects. The empire's borders expanded, encompassing territories from Britain to Egypt and from Spain to the Euphrates. Roman legions, renowned for their discipline and engineering prowess, secured and maintained these vast territories, building roads, fortifications, and cities that facilitated control and integration.
The Roman Empire’s society was hierarchical, with a rigid class system. At the top were the patricians, wealthy elites who held significant political power. Below them were the plebeians, free citizens with limited political influence, and the vast numbers of slaves who formed the backbone of the economy. The family unit was central, governed by the paterfamilias, the male head who held absolute authority.
Culturally, the Romans were eclectic, absorbing and adapting elements from the civilizations they encountered, particularly the Greeks. Roman art, literature, and philosophy reflected this synthesis, creating a rich cultural tapestry. Latin, the Roman language, became the lingua franca of the Western world, influencing numerous modern languages.
Roman architecture and engineering achievements were monumental. They perfected the arch, vault, and dome, constructing enduring structures like the Colosseum, Pantheon, and aqueducts. These engineering marvels not only showcased Roman ingenuity but also served practical purposes, from public entertainment to water supply.
BÀI TẬP BỔ TRỢ TIẾNG ANH GLOBAL SUCCESS LỚP 3 - CẢ NĂM (CÓ FILE NGHE VÀ ĐÁP Á...

BÀI TẬP BỔ TRỢ TIẾNG ANH GLOBAL SUCCESS LỚP 3 - CẢ NĂM (CÓ FILE NGHE VÀ ĐÁP Á...Nguyen Thanh Tu Collection
https://app.box.com/s/hqnndn05v4q5a4k4jd597rkdbda0fniiCACJapan - GROUP Presentation 1- Wk 4.pdf

Macroeconomics- Movie Location
This will be used as part of your Personal Professional Portfolio once graded.
Objective:
Prepare a presentation or a paper using research, basic comparative analysis, data organization and application of economic information. You will make an informed assessment of an economic climate outside of the United States to accomplish an entertainment industry objective.
The Challenger.pdf DNHS Official Publication

Read| The latest issue of The Challenger is here! We are thrilled to announce that our school paper has qualified for the NATIONAL SCHOOLS PRESS CONFERENCE (NSPC) 2024. Thank you for your unwavering support and trust. Dive into the stories that made us stand out!
"Protectable subject matters, Protection in biotechnology, Protection of othe...

Protectable subject matters, Protection in biotechnology, Protection of other biological materials, Ownership and period of protection
Mule 4.6 & Java 17 Upgrade | MuleSoft Mysore Meetup #46

Mule 4.6 & Java 17 Upgrade | MuleSoft Mysore Meetup #46
Event Link:-
https://meetups.mulesoft.com/events/details/mulesoft-mysore-presents-exploring-gemini-ai-and-integration-with-mulesoft/
Agenda
● Java 17 Upgrade Overview
● Why and by when do customers need to upgrade to Java 17?
● Is there any immediate impact to upgrading to Mule Runtime 4.6 and beyond?
● Which MuleSoft products are in scope?
For Upcoming Meetups Join Mysore Meetup Group - https://meetups.mulesoft.com/mysore/
YouTube:- youtube.com/@mulesoftmysore
Mysore WhatsApp group:- https://chat.whatsapp.com/EhqtHtCC75vCAX7gaO842N
Speaker:-
Shubham Chaurasia - https://www.linkedin.com/in/shubhamchaurasia1/
Priya Shaw - https://www.linkedin.com/in/priya-shaw
Organizers:-
Shubham Chaurasia - https://www.linkedin.com/in/shubhamchaurasia1/
Giridhar Meka - https://www.linkedin.com/in/giridharmeka
Priya Shaw - https://www.linkedin.com/in/priya-shaw
Shyam Raj Prasad-
https://www.linkedin.com/in/shyam-raj-prasad/
How to Make a Field invisible in Odoo 17

It is possible to hide or invisible some fields in odoo. Commonly using “invisible” attribute in the field definition to invisible the fields. This slide will show how to make a field invisible in odoo 17.
Chapter 3 - Islamic Banking Products and Services.pptx

Chapter 3 - Islamic Banking Products and Services.pptxMohd Adib Abd Muin, Senior Lecturer at Universiti Utara Malaysia
This slide is prepared for master's students (MIFB & MIBS) UUM. May it be useful to all.Unit 2- Research Aptitude (UGC NET Paper I).pdf

This slide describes the research aptitude of unit 2 in the UGC NET paper I.
Supporting (UKRI) OA monographs at Salford.pptx

How libraries can support authors with open access requirements for UKRI funded books
Wednesday 22 May 2024, 14:00-15:00.
Palestine last event orientationfvgnh .pptx

An EFL lesson about the current events in Palestine. It is intended to be for intermediate students who wish to increase their listening skills through a short lesson in power point.
Digital Tools and AI for Teaching Learning and Research

This Presentation in details discusses on Digital Tools and AI for Teaching Learning and Research
special B.ed 2nd year old paper_20240531.pdf

Instagram:-
https://instagram.com/special_education_needs_01?igshid=YmMyMTA2M2Y=
WhatsApp:-
https://chat.whatsapp.com/JVakNIYlSV94x7bwunO3Dc
YouTube:-
https://youtube.com/@special_education_needs
Teligram :- https://t.me/special_education_needs
Slide Shere :-
https://www.slideshare.net/shabnambano20?utm_campaign=profiletracking&utm_medium=sssite&utm_source=ssslideview
678020731-Sumas-y-Restas-Para-Colorear.pdf

KKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKKK
Recently uploaded (20)
BÀI TẬP BỔ TRỢ TIẾNG ANH GLOBAL SUCCESS LỚP 3 - CẢ NĂM (CÓ FILE NGHE VÀ ĐÁP Á...

BÀI TẬP BỔ TRỢ TIẾNG ANH GLOBAL SUCCESS LỚP 3 - CẢ NĂM (CÓ FILE NGHE VÀ ĐÁP Á...
"Protectable subject matters, Protection in biotechnology, Protection of othe...

"Protectable subject matters, Protection in biotechnology, Protection of othe...
Mule 4.6 & Java 17 Upgrade | MuleSoft Mysore Meetup #46

Mule 4.6 & Java 17 Upgrade | MuleSoft Mysore Meetup #46
Chapter 3 - Islamic Banking Products and Services.pptx

Chapter 3 - Islamic Banking Products and Services.pptx
Digital Tools and AI for Teaching Learning and Research

Digital Tools and AI for Teaching Learning and Research
Pyloric stenosis
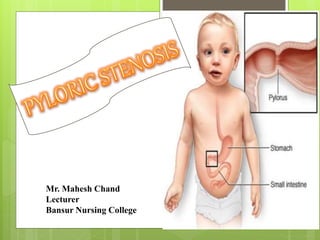
- 1. Mr. Mahesh Chand Lecturer Bansur Nursing College
- 3. Pyloric stenosis or pyloro stenosis is narrowing (stenosis) of the opening from the stomach to the first part of the small intestine known as the duodenum. The pylorus, meaning "gate".
- 5. Due to enlargement (hypertrophy) of the muscle surrounding this opening which spasms when the stomach empties. This condition causes severe projectile non-bilious vomiting. It most often occurs in the first few months of life. It more specifically labelled as infantile hypertrophic pyloric stenosis.
- 6. The thickened pylorus is felt classically as an olive-shaped mass in the middle upper part or right upper quadrant of the infant's abdomen. Pyloric stenosis also occurs in adults, where the cause is usually a narrowed pylorus due to scarring from chronic peptic ulceration.
- 8. Pyloric stenosis is defined as “narrowing (stenosis) of the outlet of the stomach so that food cannot pass easily from it into the duodenum, pyloric stenosis results in feeding problems and projectile vomiting.”
- 10. 3/1000 live birth Male: Female = 4:1 Commonly in the first born male child Most common cause for laparotomy before 1 year. Age 3weeks to 3 months. Child of those parents who affected with pyloric stenosis. It affect more commonly child than the adult.
- 27. Persistent hunger. Babies who have pyloric stenosis often want to eat soon after vomiting. Stomach contractions. Notice wavelike contractions (peristalsis) that ripple across baby's upper abdomen soon after feeding, but before vomiting. This is caused by stomach muscles trying to force food through the narrowed pylorus.
- 28. Dehydration. Baby might cry without tears or become lethargic. You might find yourself changing fewer wet diapers or diapers that aren't as wet as you expect. Changes in bowel movements. Since pyloric stenosis prevents food from reaching the intestines, babies with this condition might be constipated.
- 31. History collection Physical examination Blood tests USG X-ray of Upper GASTRO INTESTINAL Tract
- 35. Intravenous and oral atropine may be used to treat pyloric stenosis. It has a success rate of 85-89% compared to nearly 100% for pyloromyotomy, however it requires prolonged hospitalization, skilled nursing and careful follow up during treatment. It might be an alternative to surgery in children who have contraindications for anaesthesia or surgery, or in children whose parents do not want surgery.
- 37. Laparoscopic pyloromyotomy In Pyloromyotomy, the surgeon cuts only through the outside layer of the thickened pylorus muscle, allowing the inner lining to bulge out. This opens a channel for food to pass through to the small intestine.
- 40. Consider thermoregulation at all times, Before transport to theatre, transfer infant to incubator set at neutral thermal environment (NTE) temperature. Ensure incubator will be plugged in and pre-warmed for the infant to be transferred into in recovery. After return to the ward, ensure temperature is stable prior to transferring to open cot.
- 41. Monitor temperature hourly until stable. Routine post anaesthetic observations. Monitor wound and report abnormalities to surgeon. Observe for bleeding, redness, swelling, ooze from incision site. Maintain adequate fluid balance chart. Monitor IV site. Ensure adequate pain relief; use pain assessment tool.
- 43. • Failure to grow and develop. • Dehydration. Frequent vomiting can cause dehydration and a mineral (electrolyte) imbalance. Electrolytes help regulate many vital functions. • Stomach irritation. Repeated vomiting can irritate your baby's stomach and may cause mild bleeding. • Jaundice. Rarely, a substance secreted by the liver (bilirubin) can build up, causing a yellowish discoloration of the skin and eyes.
