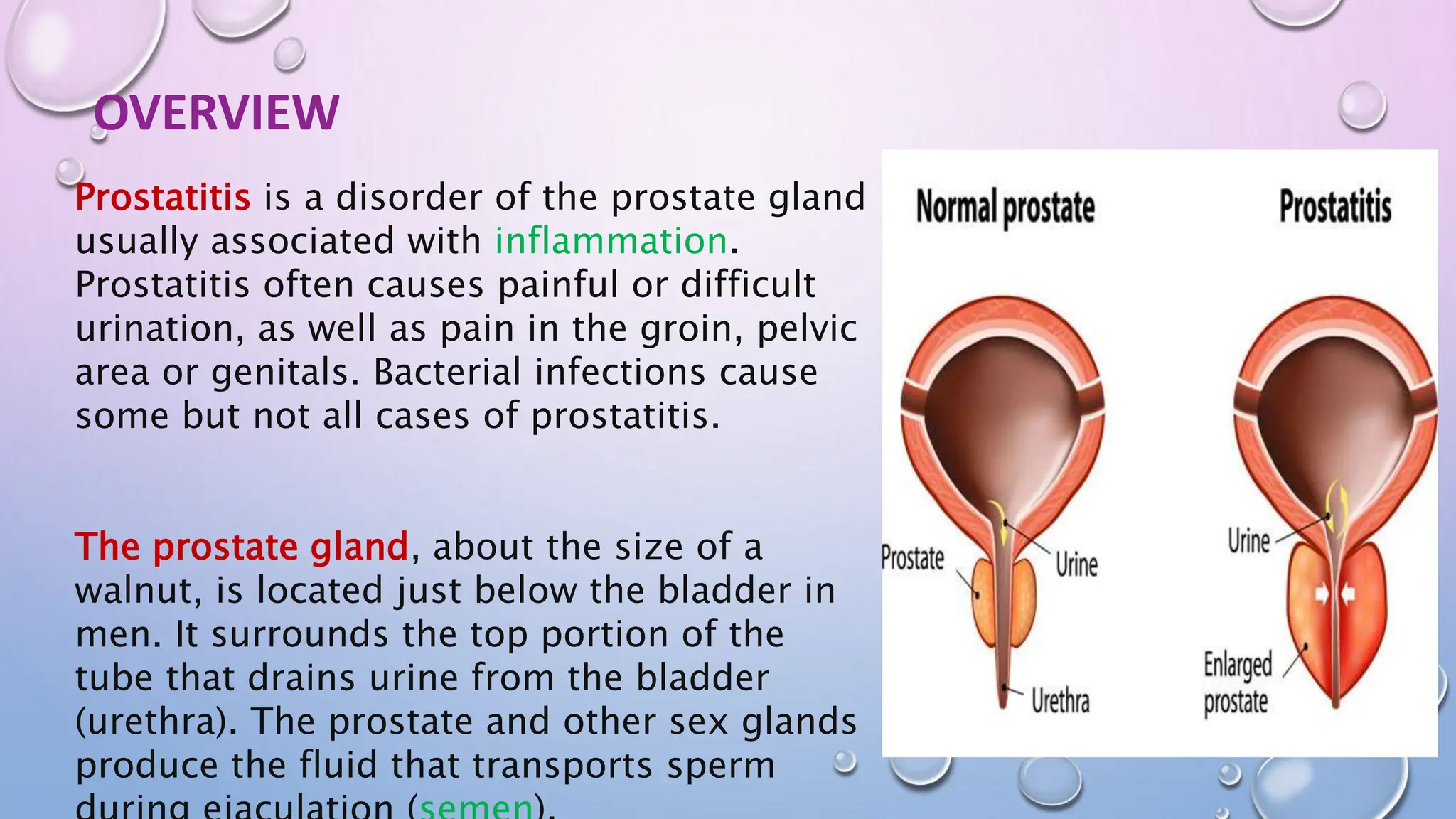
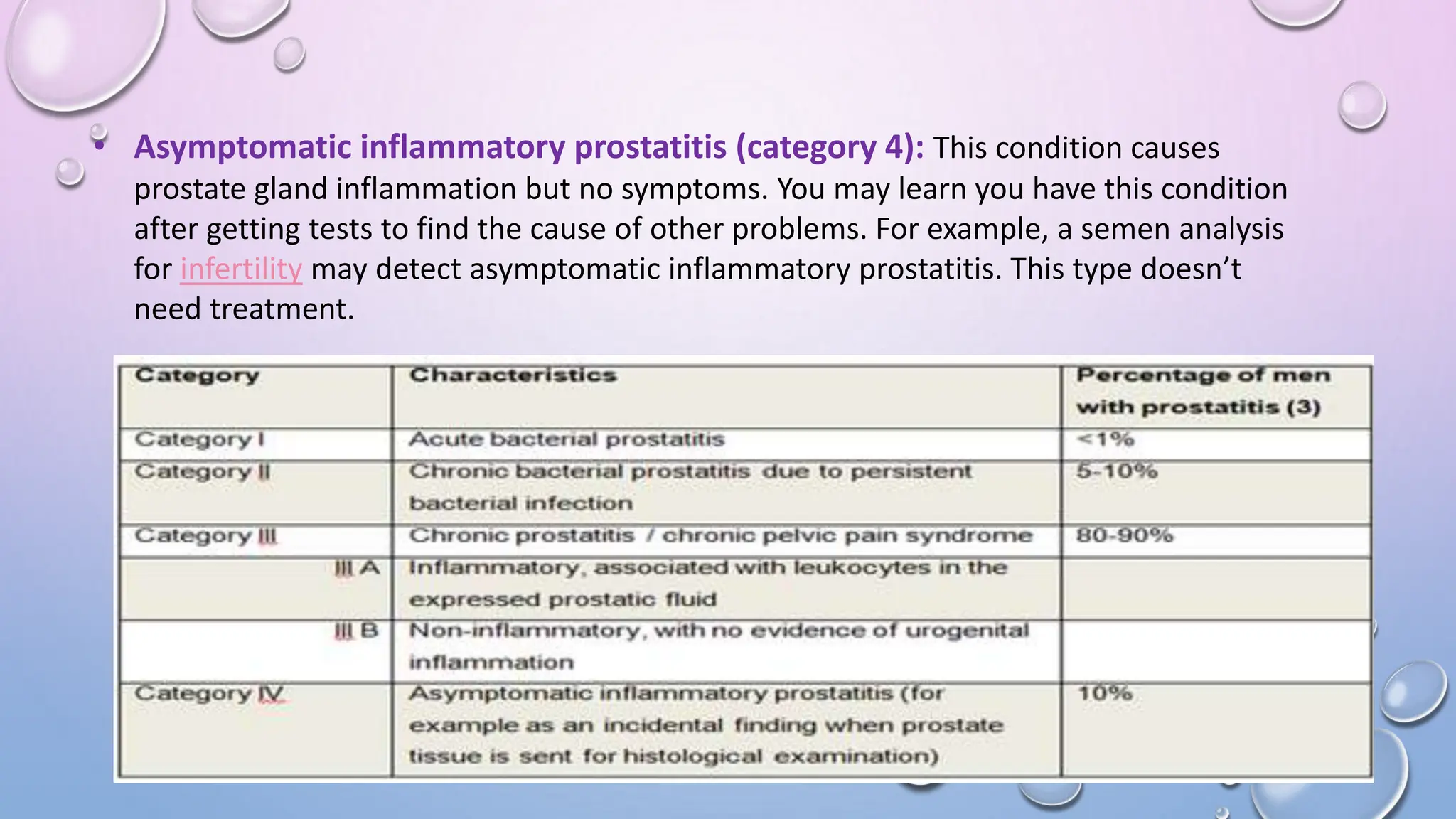
Prostatitis is inflammation of the prostate gland that causes painful or difficult urination. It has multiple types including acute bacterial prostatitis caused by urinary tract infections, chronic bacterial prostatitis where bacteria become trapped in the prostate, and chronic pelvic pain syndrome which is the most common type and causes chronic pelvic pain. Diagnosis involves digital rectal exams, urinalysis, and more invasive tests like ultrasounds or cystoscopies. Treatment depends on the type but may include antibiotics, medications to improve urine flow, stress management, supplements, and pain relievers.