BPH.pdf
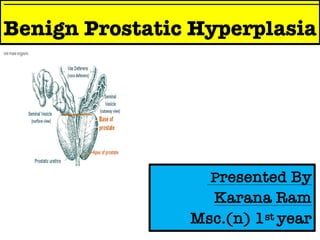
- 1. Benign Prostatic Hyperplasia Presented By Karana Ram Msc.(n) 1st year
- 2. Anatomy of Prostate Gland ❑
- 4. ➢BPH is one of the most common pathologic conditions in older men . ➢50% of men start experiencing symptoms between the age of 51-60 years. ➢Enlargement compresses the urethra, resulting in partial or complete obstruction. • Benign – not cancer. • Prostatic – to do with the prostate. • Hyperplasia – an increase in size. INTRODUCTION
- 5. Definition Benign prostatic hyperplasia (BPH), a noncancerous enlargement of the prostate gland which involves hyperplasia of prostatic stomal and glandular epithelial cell resulting in formation of large, fairly discrete nodules in transitional zone of prostate, which push on and narrow the urethra resulting in an increase resistance to flow of urine from the bladder.
- 6. Epidemiology •BPH typically occurs in men older than 40 years. •Relatives and brothers had a 4- fold and 6-fold increase chances for developing BPH
- 8. Risk factors Modifiable •Obesity •Sedentary life style •Erectile dysfunction. •Hormones •Metabolic syndrome •Increase prostatic specific antigen
- 9. Non-modi fi able •40 years and older. •Family history of BPH
- 10. Pathophysiology- Enzyme aromatase and 5-α reductase increase in activity Convert androgen hormones into estrogen and DHT(Dihydroxytestosterone) Increase in estrogen and DHT but decrease in testosterone Hyperplasia of epithelial cells and stromal cells
- 11. . Compression of urethra leading to obstruction Incomplete emptying of bladder Infections Hydronephrosis Frequeny Ascend to kidney Kidney damage
- 12. Stages of BPH •Stage 1- No bothersome symptoms and no significant obstruction •Stage 2- Those with bothersome symptoms but without significant obstruction, they can be treated with pharmacotherapy/ thermotherapy.
- 13. Contd,,, •Stage 3- Significant obstruction defined as uroflow of less than 10 ml/ s with persistent residual urine of > 100 ml, transurethral prostatic resection (turp) would be recommended. • Stage 4- Complications of bph such as chronic retention of urine and bladder stone, they would need turp
- 14. Clinical manifestation •Weak stream of urine •Urinary frequency •Urinary urgency •Hesistency •Straining •Nocturia •Urinary retention and bladder distention •Hematuria
- 15. Cont,, •Dysuria and bladder pain •Incontinence or dribling of urine •Nausea and vomitting •Pelvic discomfort and pain •Azotemia •Recurrent UTI
- 17. Dignostic evaluation ✓Personal and Family Medical History- ✓Physical examination- ✓Digital rectal Examination
- 19. Medical tests- Urinalysis- ❖For the test, a strip of chemically treated paper called a dipstick is dip into the urine. ❖Patches on the dipstick change color to indicate signs of infection in urine.
- 20. PSA blood test- ❖ Blood for a PSA test is drawn and send for lab analysis ❖ Prostate cells create a protein called PSA. ❖BPH, prostate infections, inflammation, aging, and normal fluctuations often cause high PSA levels
- 21. Urodynamic tests ➢ Uroflowmetry ➢ Postvoid residual measurement ➢ Reduced urine flow.
- 22. Cystoscopy ❖ To look inside the urethra and bladder for blockage or stones in the urinary tract.
- 23. Cystoscopy
- 24. Transrectal ultrasound ❖ Safe, painless sound waves send off to organs to create an image of their structurae. ❖The ultrasound image shows the size of the prostate and any abnormalities, such as tumors.
- 26. Management of BPH Watchful waiting- •Symptoms are mild and not causing any change in the day- to-day activities, wait and watch. •Regular check-up is recommended.
- 27. Drug name Dosage Mechanism Side effects 1.Finasteride 2. Dutasteride 5 mg once daily 0.5 mg once daily 5- alpha reductase inhibitors ➢Block the production of DHT ➢Decrease prostate growth. ➢Shrink the size of prostate decreased libodo, decreased semen quantity decreased semen prostate specific antigen, gynecomastia
- 28. Drug name Dosage Mechanism Side effects 1. Terazosin 2. Doxazosin 1 mg/day may upto 10 mg/ day 1mg/day may upto 8 mg/day Α1-adrenergic receptor antagonist ➢Relax the smooth muscle of prostate and bladder ➢Improve urine flow ➢Reduce bladder blockage hypotension, dizziness, dyspnea, aggrevate GI problem such as peptic ulcer.
- 29. Surgical management Minimally invasive therapy- Transurethral electrovaporization (TUVP) •In TUVP, the surgeon inserts a thin, tube- like instrument (resectoscope) into the urethra. This instrument has a lens, a light, and a tool that sends out an electrical current to destroy prostate tissue. Heat from the electrical current seals small blood vessels, reducing the risk of bleeding
- 30. Transurethral microwave thermotherapy (TUMT) ➢More specific destruction of malignant cells without affecting normal cells. ➢ Can be achieved by raising the temperature of the cells using low-level radiofrequency (microwave) in the prostate up to 40 to 45°C, 46 to 60°C (thermotherapy), and 61 to 75°C (transrectal thermal ablation).
- 32. Transurethral needle ablation (TUNA) ➢Utilizes needle to deliver High- frequency radio waves to destroy the enlarged prostatic tissue ➢ Successful for small-sized gland. ➢ Poses a low or no risk for Incontinence and impotence.
- 34. Transurethral ethanol ablation of the prostate ➢Transurethral injection of absolute ethanol into the lateral lobes of prostate ➢Produces necrotic effect on prostatic tissue
- 35. Transurethral Water Jet Ablation (TWJA) ➢ Simple technique that uses a cylindrical balloon to circulate hot water ➢Resulting in even coagulation necrosis in the prostate by raising the temperature of the prostatic cells up to 60 to 70°C
- 36. Water induced thermotherapy This procedure uses heated water to destroy prostate tissue.
- 37. INVASIVE PROCEDURE- Transurethral resection of prostate (TURP) •Three-way indwelling catheter with a 30-mL balloon is inserted into the bladder after the procedure to provide hemostasis and to facilitate urinary drainage. The bladder is irrigated, either continuously or intermittently, usually for the first 24 hours to prevent obstruction from mucus and blood clots.
- 38. Transurethral Resection of Prostate • gold standard for surgical treatments of obstructing BPH.
- 39. Transurethral incision of the prostate (TUIP) •Several small incisions are made into the prostate gland to expand the urethra, which relieves pressure on the urethra and improves urine flow. •option for patients with a small or moderately enlarged prostate gland
- 40. Transurethral Incision of Prostate
- 41. Open prostatectomy ➢Incision or cutis made through the skin to reach the prostate. ➢ The urologist can remove all or part of the prostate through the incision. ➢ Indicated when the prostate is greatly enlarged, complications occur, or the bladder is damaged and needs repair.
- 43. Nursing management Nursing diagnosis Acute pain related to musosal irritation secondary to bladder distension.
- 44. Intervention •Assess the level of pain •Tape drainage tube to thigh to prevent pull on bladder and erosion of the penile- scrotal junction •Recommend bed rest as indicated •Provide comfort measures such as back rub •Helping patient assume position of comforts
- 45. Incomplete emptying of the bladder /urinary retention related to mechanical obstruction secondary to enlarged prostate gland. Intervention- •Encourage the patient to void every 2-4 hours and when urge is felt. •Asses for S/s of urinary retention, amount and frequency of urination, suprapubic distention, complaint of urgency and discomfort
- 46. Anxiety related to concern and lack of knowledge about diagnosis treatment plan and prognosis Intervention • Determine patient’s concern, level of understanding whether he is aware of diagnosis and prognosis • Explain the investigations and diagnosis in simple term and in language known to the patient • Asses his psychological reaction
- 47. Risk for fluid volume related post obstructive diuresis from rapid drainage of chronically overdistended bladder. Intervention •Monitor intake and output carefully. Note outputs of 100 to 200 ml/hour •Encourage increased oral intake based on individual needs. •Monitor BP, pulse. Evaluate capillary refill and oral mucosa membranes
- 48. Risk of infection related to surgical incision, immobility and presence of catheter Intervention •Assess the health status of patient •Observe urine for cloudiness, colour, •Observe testicular swelling, pain, tenderness, and redness •Provide adequate perineal care
- 49. Complications- 1. urinary retention 2. Urinary tract infections 3. Bladder stones 4. Bladder damage 5. Kidney damage 6. Renal stone
- 50. RESEARCH ARTICLE HoLEP: The new gold standard for surgical treatment of benign prostatic hyperplasia Abstract INTRODUCTION Transurethral resection of the prostate (TURP) was considered the "gold standard" surgical treatment for medication-refractory benign prostatic hyperplasia (BPH) for decades. With the desire to reduce hospital stay, complications, and cost, less invasive procedures.With the advent of a soft tissue morcellator, holmium laser enucleation of the prostate (HoLEP) was introduced as an efficacious alternative to TURP and due to its advantageous side effect profile compared to TURP,
- 51. Contd,, Materials and methods: We provide a review on the evolution of HoLEP as a gold standard compared to the historical reference procedures for BPH, and provide a review of emerging laser technologies. Results: A growing body of literature has shown HoLEP(holmium laser prostate surgery) to be a safe and efficient procedure for the treatment of BPH for all prostate sizes. Long term studies have proven the durability of HoLEP, as a first line surgical therapy for BPH.
- 52. Conclusion •BPH is the nonmalignant enlargement of the prostate gland and a common cause of voiding dysfunction in men. •The primary goal of the treatment is not only to improve urinary flow and reduce symptoms scores, but also to prevent serious complications and improve quality of life. Selection of therapy depends on a number of factors like history, severity of symptoms, procedural complications, and associated side effects
- 53. SUMMARY- We have learnt about- •Definitions of benign prostatic hyperplasia,Its epidemiology and causes,Pathophysioly of BPH ,Clinical manifestation,Diagnostic evaluation,Management and its prognosis.
- 54. References 1)Brunner and Suddarth; Textbook of Medical Surgical Nursing 13th Edition Volume II. New Delhi; Wolters Kluwer Publication. 2)Lewis. Medical Surgical Nursing Assessment and Management of clinical problems.2015. New Delhi. Elsevier. 2nd Edition. Volume II. 3)Petrica A. Potter; Fundamentals of Nursing South Asian Edition Volume I. New Delhi; Elsevier Publications 4)Joyce M. Black, Jane Hokanson Hawks. Medical Surgical Nursing Clinical Management of Positive Outcomes.2015. New Delhi. Reed Elsevier India Private Limited. Volume II.
- 55. Contd, •Deters LA. Benign prostatic hypertrophy. Emedicine website. http://emedicine.medscape.com . Updated March 28, 2014. Accessed september 30, 2018. •BPH: surgical management. Urology Care Foundation website. www.urologyhealth.org . Updated July 2013. Accesse October 1, 2018 •Enlarged prostate. MedlinePlus website. www.nlm.nih.gov . Updated October 2, 2013. Accessed October 7, 2018 •Wikepedia.com. benign prostatic hyperplasis [Internet]. 2018[updated 2018 Sept]. available from: URL: http:// en.wikipedia.org/wiki/ benign prostatic hyperplasis.htm. Retrieved on: 17 Sept 2018
