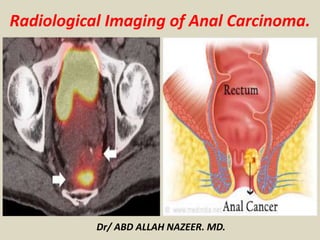
Presentation1, radiological imaging of anal carcinoma.
- 1. Radiological Imaging of Anal Carcinoma. Dr/ ABD ALLAH NAZEER. MD.
- 2. Normal Anatomy: The anal canal begins at the narrowing of the rectal ampulla at the anorectal junction where the rectum enters the puborectalis sling at the apex of the anal sphincter complex. It extends distally for approximately 4 cm and ends at the anal verge where the squamous mucosa blends with the perianal skin. The anal margin is the circular rim of pigmented skin with folds surrounding the anus, extending over an approximately 5-cm radius away from the anal verge. The most significant landmark of the anal canal is the dentate line, which lies 2.5–3 cm proximal to the anal verge and is visible macroscopically but not on MRI. Its position can be estimated either by measuring 2.5 cm above the anal verge or by dividing the anal canal into thirds so that the dentate line lies at the junction of the middle and upper thirds. The anal canal is divided by the dentate line into an upper part, lined with transitional or rectal glandular mucosa, and a lower part, lined by nonkeratinizing squamous epithelium, that merges with the perianal skin. The anal transition zone is defined as the histologic zone interposed between uniform rectal glandular mucosa above and uninterrupted squamous epithelium below, and it often has a heterogeneous histologic appearance.
- 3. Illustrative anatomy of anal canal. A, Line diagram shows anal anatomy. B, Healthy 67-year-old man (with treated prostate cancer).Coronal T2-weighted image that corresponds to A shows ischioanal fossa (IAF), external sphincter (ES), and internal sphincter (IS).
- 4. C, Healthy 53-year-old woman (with treated carcinoma cervix). Axial T2-weighted image through upper anal canal shows urethra (Ur) and vagina (Va). D, 67-year-old woman (post TAH and BSO for endometrial sarcoma). Sagittal T2-weighted image shows pubococcygeal line (long straight line), which is generally at level of anorectal junction. Angled line shows reference plane that one should use when reporting distance of epicenter of abnormality from anal verge.
- 5. Anal cancer is a relatively uncommon malignancy. It accounts for less than 2% of large bowel malignancies and 1-6% of anorectal tumours (~1.5% of all gastro-intestinal tract malignancies in the Unites States). Epidemiology There may be a slight male predilection where its incidence has been reported to be approximately 0.5 per 100 000 in men and 1.0 per 100 000 in women. Its incidence is thought to be rising over the years. Clinical presentation Approximately 45% of patients may present with bleeding per rectum. Around 30% of patients may have pain and/or a sensation of a mass. Pathology Anal carcinoma typically originates between the anorectal junction above and the anal verge below. The vast majority of anal canal cancers are squamous cell cancers.
- 6. Risk factors Both male and female: HPV / HIV infection immunosuppression number of lifetime sexual partners, and receptive anal intercourse smoking In females: previous in situ or invasive cervical, vulval or vaginal cancer. Lymphatic spread tumour above dentate line: to pararectal and paravertebral nodes tumour below dentate line: to inguinal and femoral nodes
- 7. The accepted TNM staging of anal cancer is as follows: Primary tumour (T) TX: primary tumour cannot be assessed T0: no evidence of primary tumour Tis: carcinoma in situ T1: tumour 2 cm or less in greatest dimension T2: tumour >2 cm but <5 cm in greatest dimension T3: tumour >5 cm in greatest dimension T4: tumour of any size invades adjacent organ(s), e.g. vagina, urethra, bladder Regional lymph nodes (N) Nx: regional lymph nodes cannot be assessed N0: no regional lymph node metastasis N1: metastasis in perirectal lymph nodes(s) N2: metastasis in unilateral internal iliac and/or inguinal lymph node(s) N3: metastasis in perirectal and inguinal lymph nodes and/or bilateral internal iliac lymph nodes Distant metastasis (M) Mx: distant metastasis cannot be assessed M0: no distant metastasis M1: distant metastasis
- 8. Radiologic staging is supplemented by clinical assessment of the anal margin, verge, and canal. This assessment often involves an examination with the patient under anesthesia and biopsy. Biopsy or fine-needle aspiration cytology of any enlarged or suspicious-appearing inguinal nodes is also essential. Transanal Endoscopic Ultrasound Transanal endoscopic ultrasound has results comparable to MRI for the detection of local tumor spread in patients with anal carcinoma and may be superior to MRI for the detection of small superficial tumors. However, regional lymph nodes higher in the pelvis or groins are outside the FOV of endosonography and supplementary MRI is needed for N staging. A meta-analysis of staging rectal cancer using endorectal ultrasound revealed other limitations including operator dependency and inability to assess stenotic tumors ; these limitations likely apply equally to anal cancer.
- 9. MRI MRI has become the imaging modality of choice for locoregional staging and assessment of tumor response after chemoradiotherapy. MRI provides high-resolution multiplanar information about the location, size, circumferential and craniocaudal extent of the primary tumor and information regarding the involvement of adjacent structures. There is no significant difference in diagnostic value between pelvic surface coils and endoluminal coils. Moreover, endoluminal coil imaging is limited by a narrow FOV and near-field artifact and may not be tolerated by patients with anal cancer. MRI with a pelvic surface coil is easy, is more acceptable to the patient, and shows both local spread of the disease as well as lymph node involvement. We routinely perform MRI of anal cancers with a standard technique using a body coil; we obtain transaxial T1-weighted images with a 5-mm slice thickness to cover the abdomen and pelvis. High-resolution thin-section T2-weighted images are obtained with a 3-mm slice thickness in three orthogonal planes through the anal canal using a pelvic surface coil. In our experience, contrast-enhanced MRI offers limited advantages over standard T2-weighted sequences in routine primary staging but can be helpful to assess fistulation to other organs. Fat-suppressed imaging can help improve the conspicuity of the primary tumor, and STIR sequences are also useful to show fistula tracks. Diffusion-weighted imaging has an emerging role, particularly for detection of recurrent tumor after therapy, and can aid in differentiation of suspected residual or recurrent tumor from treatment-related change.
- 10. 8F-FDG PET/CT FDG PET/CT has an increasing role in staging and treatment planning of anal carcinoma, particularly because up to 98% of anal tumors are FDG-avid. At diagnosis, FDG PET/CT is used to evaluate primary tumor size, lymph node status, and whether distant metastases are present. FDG PET/CT can also be useful for planning radiation therapy by clearly defining sites of metabolically active tumor. Several studies have shown that FDG PET/CT (in comparison with standard imaging) alters staging of anal carcinoma in approximately 20% of cases and treatment intent in approximately 3–5% of cases. Although PET/CT has a lower sensitivity in detecting perirectal nodes than MRI, this shortcoming does not affect management because perirectal nodes are routinely irradiated. The main impact of PET/CT on therapy stems from its superiority in detecting involved pelvic or inguinal lymph nodes, provoking the radiation oncologist to include them in the radiotherapy field.
- 11. T staging of rectal cancer according to depth of tumor invasion as seen on axial T2-weighted MR images. (a) T1 cancers invade the submucosa (arrows) but do not involve the muscularis propria. (b) T2 cancers invade the muscularis propria but do not reach the subserosa (arrow). (c) T3 cancers invade beyond the muscularis propria (arrow). (d) T4 cancers invade through the serosal covering (T4a) or another fascial plane (T4b) and/or involve an adjacent organ (T4b) (arrows).
- 12. A 32-year-old HIV-positive woman with clinical diagnosis of anovaginal fistula. Axial T2-weighted (a) and post-contrast fat-suppressed axial T1-weighted (b) images show inhomogeneous anal tissue invading the left aspect of the vagina (arrowheads), with internal non-enhancing necrosis and peripheral enhancement. Biopsy diagnosed SCAC with superimposed infection
- 13. Early anal tumour, MR image shows that normal low signal of anal canal muscle has been replaced by intermediate-signal tumor (arrow) that is less than 2 cm. Early anal carcinoma, anterior T2 anal canal carcinoma. MR image shows that lesion measures more than 2 cm and hence achieves T2 status. There is invasion of external sphincter (arrow).
- 14. A 40-year-old MSM with bioptic diagnosis of SCAC. Axial (a) and sagittal (b) T2-weighted images show 2-cm hyperintense nodule contained within the internal sphincter muscle, intensely enhancing as seen on post-contrast fat-suppressed coronal T1-weighted image (c), consistent with T1 tumour (arrowheads).
- 15. A 62-year-old female with biopsy-proven SCAC. Axial T2-weighted (a), post-contrast fat-suppressed axial (b) and coronal (c) T1-weighted images, and corresponding enhanced image from body CT (d) show a 5.5- cm long (T3) enhancing tumour with infiltration of the left ischioanal fatty space (arrowheads).
- 16. A 57-year-old woman undergoing abdomino-pelvic MDCT for unrelated reasons. Post-contrast axial (a) and coronal reformatted (b) detailed images of the anorectal region identify an unexpected 2-cm right-sided enhancing anal nodule. Subsequent clinical and bioptic assessment confirmed poorly symptomatic ulcerated SCAC.
- 17. 46-year-old man with T3 anal carcinoma. A, Coronal T2- weighted image shows that neoplasm (bracket) extends from anal margin into lower rectum and is more than 5 cm in maximum dimension and therefore is T3. There is invasion of external sphincter and of left levator ani muscle (arrow). 46-year-old man with T3 anal carcinoma. B, MR image shows no evidence of adjacent organ invasion, as evidenced by complete low-signal rim (arrowheads) separating tumor from prostate anteriorly.
- 18. Axial contrast-enhanced MR images in a patient with stage IIIB (cT3N2M0) adenocarcinoma of the rectum. (a) Image shows a low rectal mass with a small focus of extension into the adjacent mesorectal fat (arrow) (T3 disease). (b, c) Multiple enhancing subcentimeter mesorectal lymph nodes (arrows in b) and a left internal iliac lymph node (arrow in c) suggest N2 disease on the basis of the number of potentially involved lymph nodes. The patient subsequently underwent neoadjuvant chemotherapy and radiation therapy and resection.
- 19. Stage IIIB (cT3N2M0) squamous cell carcinoma of the anus. (a, b) Coronal CT images obtained at different levels show a locally extensive mass extending superiorly from the anorectal junction (arrows in a). Pathologic analysis demonstrated squamous cell carcinoma consistent with anal cancer, despite the relatively superior location. A prominent left internal iliac lymph node is also seen (arrow in b). (c, d) Coronal CT images obtained at different levels 3 months after completion of definitive chemoradiation therapy show a partial radiographic response of both the primary mass and the left internal iliac lymph node.
- 20. An elderly, 92-year-old man with previous prostatectomy and kidney failure has unenhanced MRI. Sagittal T2- (a) and axial T1-weighted (b) images show 5-cm long solid, inhomogeneous neoplastic tissue (*) extending from the anus to encase the proximal urethra (note catheter in place).
- 21. A 65-year-old woman with history of previously treated small SCAC 3 years earlier. Axial T2- (a) and post-contrast T1-weighted (b) images show roundish 1-cm left inguinal node (arrowheads) with internal fluid-like necrosis and inhomogeneous enhancement, confirmed by ultrasound (c) as hypoechoic with loss of normal nodal structure. Surgical exeresis (postoperative status as seen in d, follow-up MRI) confirmed metastatic node from SCAC.
- 22. Axial T2-weighted (a, b) and post-contrast fat-suppressed T1-weighted (c) images show inguinal nodal metastases, larger on left side (arrowheads) plus bilateral enhancing perirectal adenopathies (arrows)
- 23. 35-year-old woman with T4 anal cancer. MR image shows lobulated tumor with central necrosis and invasion into posterior vagina (arrow).
- 24. Axial fused FDG PET/CT images of 45- year-old man with upper anal cancer. A, Bulky anal cancer shows increased FDG uptake (arrow) and metabolically active right inguinal node (arrowhead). Axial fused FDG PET/CT images of 45-year-old man with upper anal cancer. B, Increased uptake in pelvic sidewall lymph node (arrowhead) is consistent with disease involvement. Axial fused FDG PET/CT images of 45-year- old man with upper anal cancer. C, Increased uptake in unsuspected liver lesion (arrowhead) was subsequently shown to be metastasis on liver MRI (not shown). Ability of FDG PET/CT to stage regional and metastatic disease accurately in single examination is its great strength
- 25. A, Coronal T2-weighted MR image shows bulky T3 tumor in upper anal canal (arrow) that was subsequently treated with chemoradiotherapy. Coronal T2-weighted image obtained 8 weeks after therapy shows that tumor has diminished in size and there is tram-track appearance of low-signal fibrotic tissue encasing anal canal wall (arrowhead). Note that mass like pseudotumor of high signal in rectal mucosa (arrow) is edema from radiotherapy.
- 26. 37-year-old man with bulky T3 anal cancer. A, Axial T2-weighted MR image obtained before treatment. 37-year-old man with bulky T3 anal cancer. B, Axial T2- weighted image obtained 3 months after therapy depicts low-signal fibrosis in place of tumor (arrow). Patient had complete response clinically and radiologically.
- 27. A, T2-weighted MR image obtained at time of initial staging shows abnormal tumor tissue in lower anal canal, which was treated with chemoradiotherapy. B, T2-weighted MR image obtained 8 weeks after therapy shows significant size reduction and fibrotic reaction, but residual nodule (arrow) suspicious for remnant tumor is seen. C, Repeat T2-weighted MR image obtained immediately before resection shows nodule (arrow) has enlarged compared to initial post treatment (B). This nodule was confirmed to be tumor at histology after salvage abdominoperineal resection.
- 28. A, Coronal T2-weighted MR image shows small tumor involving lower anal canal and anal margin (arrow) that was treated with chemoradiotherapy with good initial response B, Coronal MR image obtained for surveillance 1 year after chemoradiotherapy shows intermediate- to high-signal abnormality (arrow) suspicious for recurrent tumor at site of original primary. C, Axial T2-weighted MR image from same examination as B shows areas of small-volume, linear post- therapy fibrosis (arrowhead) and bulky intermediate- to high-signal abnormality (arrow) suspicious for recurrence. D, Apparent diffusion coefficient map from diffusion- weighted imaging series shows rim of restricted diffusion (arrow) in intermediate T2 signal areas indicative of high cellular content.
- 29. A 60-year-old man with AIDS and clinical finding of ulcero-fungating anal mass. Axial (a) and coronal reformatted (b) CT images show moderately heterogeneous tissue (*) in its entire longitudinal extent from the anorectal junction to below the anal verge, associated with large necrotic iliac adenopathies (* in c). Biopsy confirmed super infected SCAC.
- 30. An 83-year-old man with known SCAC. Initial MRI shows moderate circumferential thickening of the anus with T2-hyperintense signal (a) and contrast enhancement (b) (arrowheads). Complete disappearance of the lesion is observed on axial T2 (c) and post-contrast fat-suppressed T1-weighted (d) images following chemo-radiotherapy.
- 31. An elderly, 85-year-old lady with biopsy-proven SCAC and multiple comorbidities. Initial MRI (a, b) shows showed circumferential anal wall thickening with abnormal solid signal (arrowheads) measuring 6 cm in length, plus a suspicious centimetric left inguinal lymph node (arrow in a), findings consistent with T3N2 lesion. After reduced chemo-radiotherapy, follow-up MRI (c, d) 4 months later disclosed progression and partial necrosis of both primary tumour (arrowhead) and inguinal adenopathy (arrow), plus appearance of an exophytic tissue mass protruding from the external anal orifice (* in d)
- 32. A 40-year-old male patient with long-standing perianal Crohn’s disease, being treated with seton. Contrast-enhanced MDCT images (a, b, c in cranio-caudal order) show right-sided levator ani abscess (*), extensive perianal fistulization occupying the ischioanal space (arrow), and marked solid-appearing circumferential anorectal thickening (arrowheads). Abdomino-perineal resection for SCAC was performed
- 33. Image shows an HIV-positive 41-year-old male with squamous cell carcinoma of the anus. Pretreatment FDG-PET/CT (left) demonstrated increased uptake in the anal canal (arrows) and a left internal iliac lymph node. Post-treatment FDG-PET/CT (right) demonstrated persistent uptake in the anal canal and new activity in the right lobe of the liver (arrows). The patient had biopsy- proven local and distant disease and died from local and metastatic disease 12 months after completion of chemoradiation.
- 34. Image shows a 47-year-old female with squamous cell carcinoma of the anus. Pretreatment FDG-PET/CT (left) demonstrated increased uptake in the right anal canal and two 5-mm perirectal lymph nodes. Post-treatment FDG-PET/CT (right) showed complete metabolic response. She remains without evidence of disease 31 months after chemoradiation.
- 35. Thank You.
