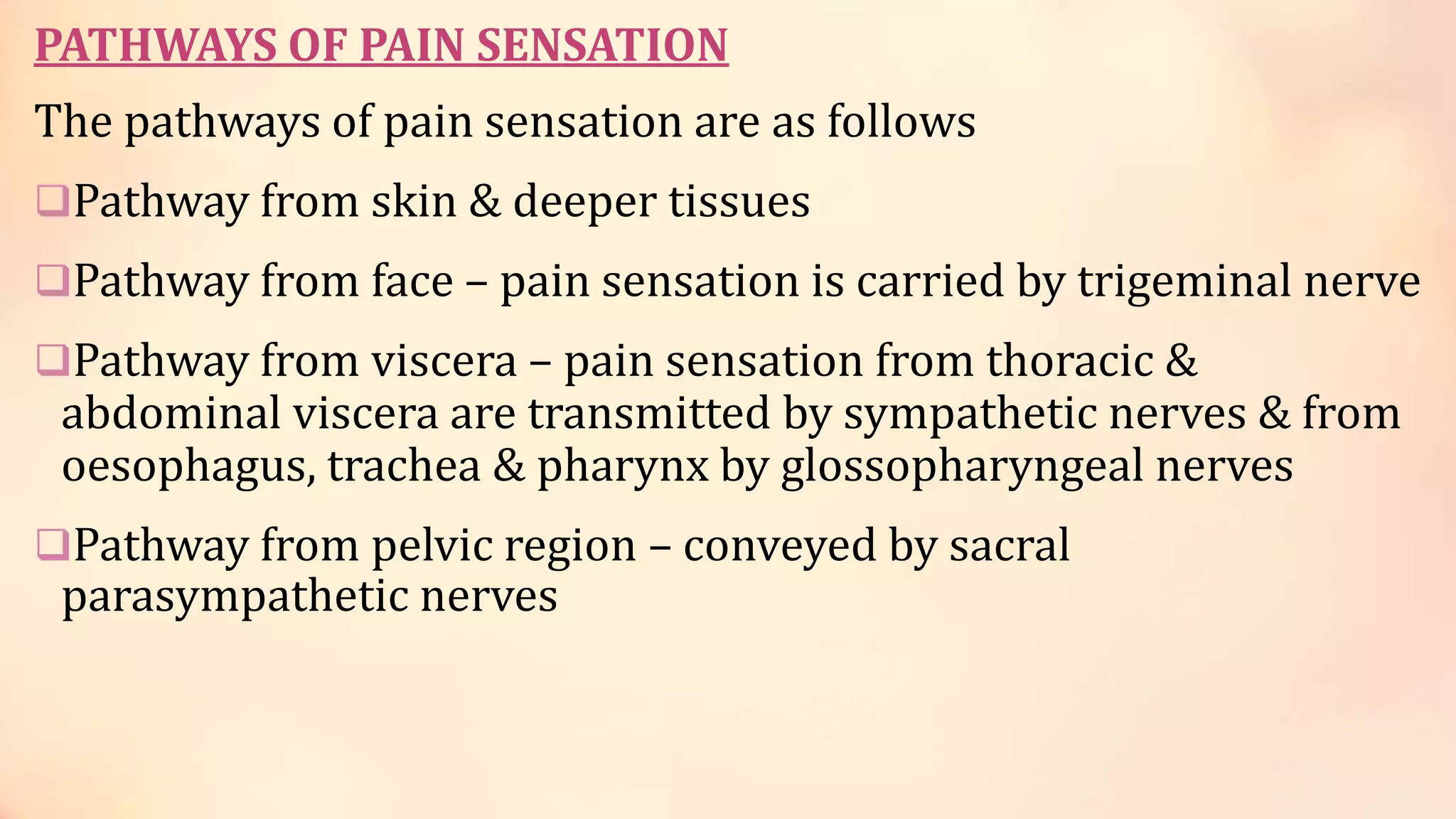
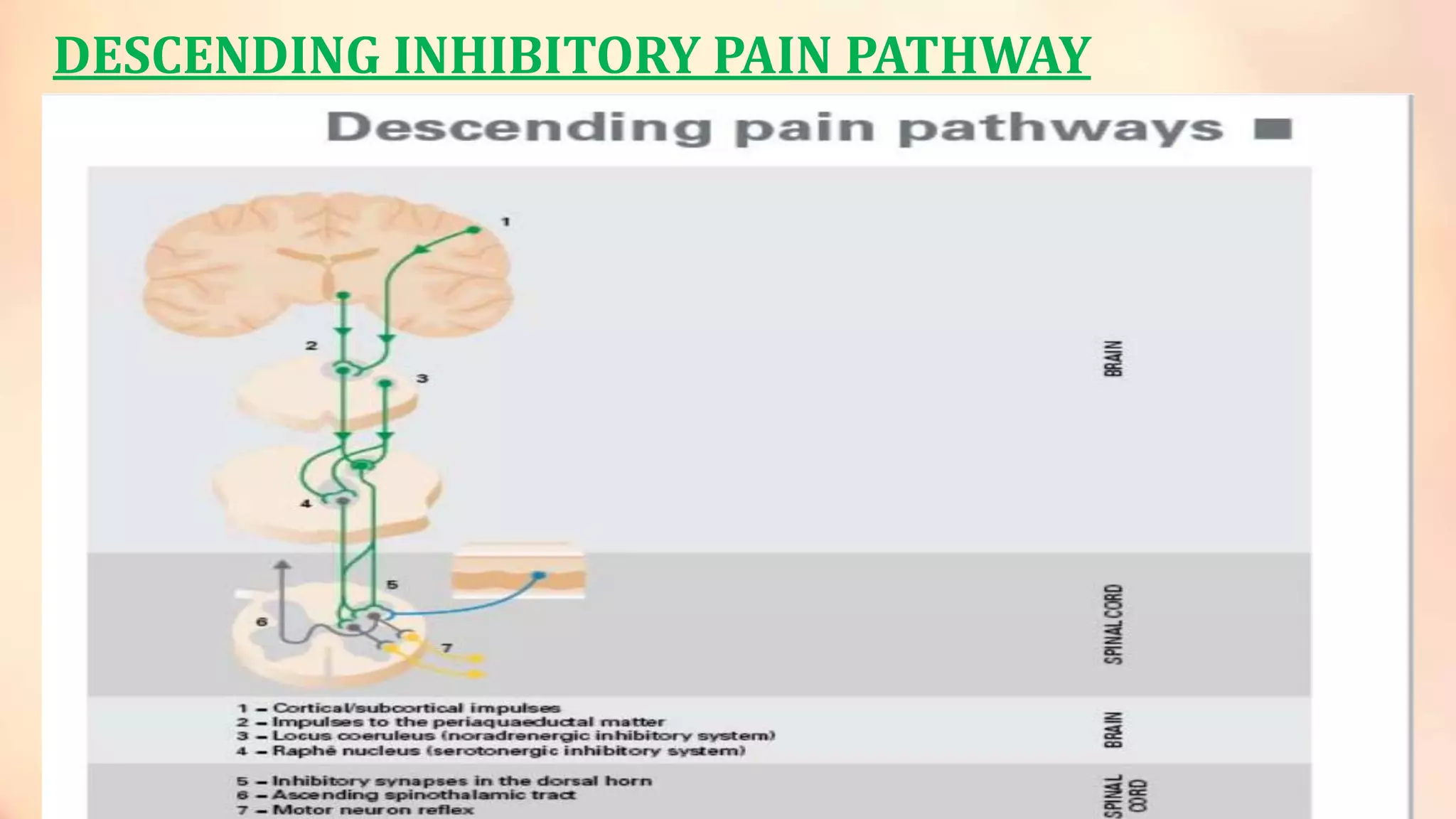
Pain is an unpleasant sensory and emotional experience caused by actual or potential tissue damage. It serves a protective function by warning us of damage. Pain is transmitted through specialized pain pathways and is classified based on duration, location, and source. There are different types of pain receptors that detect various painful stimuli and transmit signals through different nerve fiber types to the central nervous system where pain is perceived.