1) The document describes various methods of oxygen therapy used in intensive care units (ICU), including their history, mechanisms, and types.
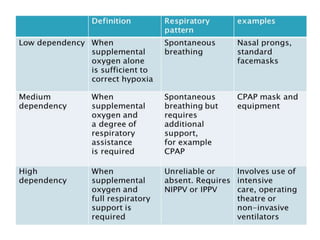
2) Oxygen therapy systems are classified based on their performance as either variable (no control of fraction of inspired oxygen or FiO2) or fixed (controlled FiO2), and based on their design as either low-flow, reservoir, or high-flow systems.
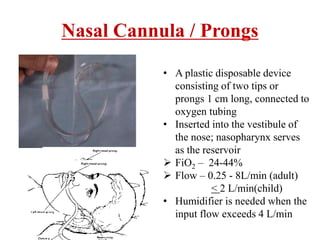
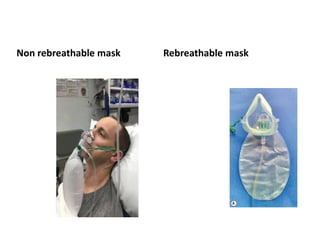
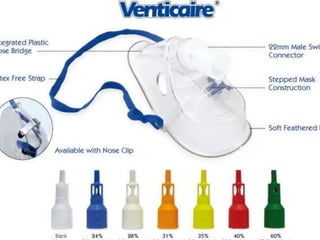
3) Common oxygen delivery devices discussed include nasal cannulas, masks, venturi masks, and high flow nasal cannulas. Each has distinct mechanisms to provide a range of FiO2 depending on the flow rate and patient factors.