This document provides information on various nemathelminth parasites. It discusses the diagnostic stages, infective stages, modes of transmission, signs and symptoms of infection, and treatment for several parasites including:
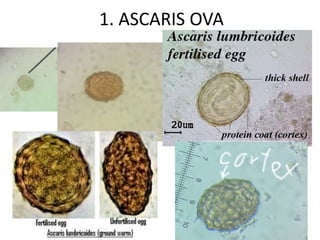
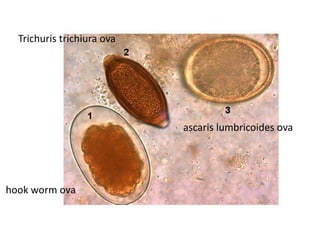
1. Ascaris lumbricoides
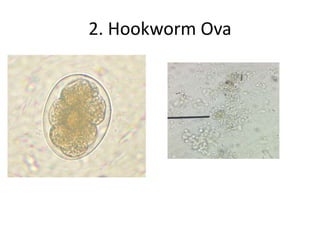
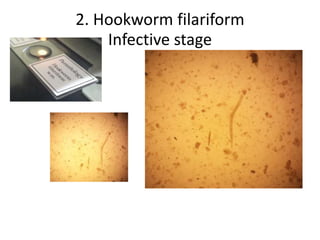
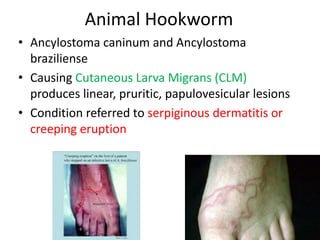
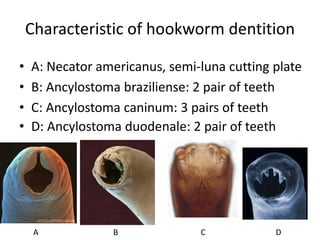
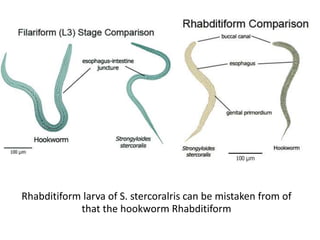
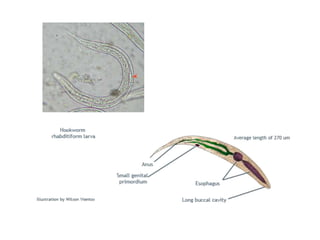
2. Hookworms
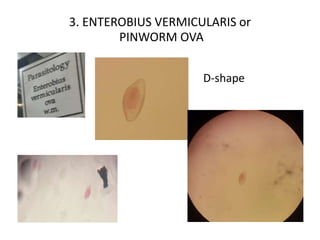
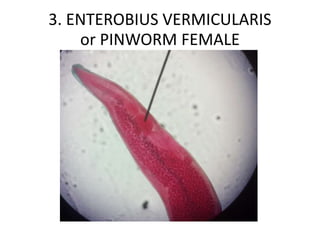
3. Enterobius vermicularis
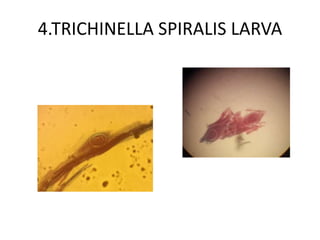
4. Trichinella spiralis
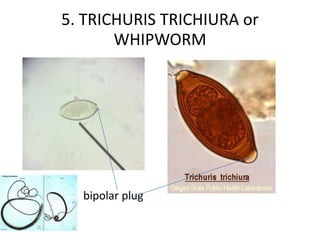
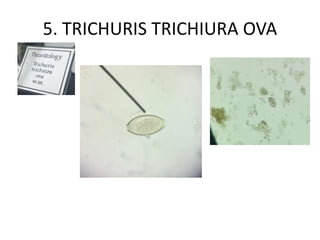
5. Trichuris trichiura
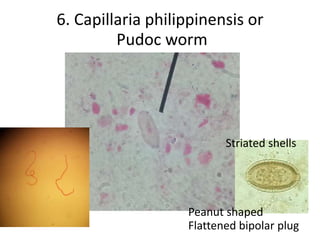
6. Capillaria philippinensis
7. Strongyloides stercoralis
8. Wuchereria bancrofti
9. Brugia malayi
10. Onchocerca volvulus
11. Dirofilaria immitis