Muscular system-and-nervous-system
•
0 likes•60 views
The muscular system has several general functions including movement, posture, communication through body language, and digestion. There are four types of muscles: prime movers, antagonists, fixators, and synergists. Skeletal muscles are attached to bones and are voluntary. They contract through the alternating bonding of actin and myosin fibers. Muscles create movement through actions like flexion, extension, abduction, and rotation. The nervous system has a central nervous system of the brain and spinal cord and a peripheral nervous system of cranial and spinal nerves. It is divided into somatic and autonomic systems for voluntary and involuntary control.
Report
Share
Report
Share
Download to read offline
Recommended
Presentation: The Locomotor System

The Locomotor System
Rafa's Classroom
CLIL material
Primary Education
Year 5
Natural Science
Bilingual Education
Recommended
Presentation: The Locomotor System

The Locomotor System
Rafa's Classroom
CLIL material
Primary Education
Year 5
Natural Science
Bilingual Education
More Related Content
What's hot
What's hot (20)
3 Skeleton, Joints, Muscles, Circulatory + Respiratory Sys

3 Skeleton, Joints, Muscles, Circulatory + Respiratory Sys
Similar to Muscular system-and-nervous-system
Lesson 13 skeletal and muscular system

This presentation contains the Human Skeletal and Muscular System. Components and Physiological Processes were also discussed. Naming of muscles was highly emphasized.
#1 anatomy-anatomical overview

This presentation is very important to study the musculoskeletal system and the sports.
UNIT- II, SKELETAL SYSTEM BY SANJAY SIR

THIS PRESENTATION IS UPLOADED TO HELP MEDICAL, NURSING & ALLIED HEALTH SCIENCES EDUCATOR FOR THEIR STUDENTS. IT WILL ALSO CREATE AWARENESS AMONG COMMON PEOPLE ABOUT OUR BODY STRUCTURE.
The muscular system

This PowerPoint presentation covers the anatomy, physiology and common disorders of the muscular system.
Similar to Muscular system-and-nervous-system (20)
Recently uploaded
New Directions in Targeted Therapeutic Approaches for Older Adults With Mantl...

i3 Health is pleased to make the speaker slides from this activity available for use as a non-accredited self-study or teaching resource.
This slide deck presented by Dr. Kami Maddocks, Professor-Clinical in the Division of Hematology and
Associate Division Director for Ambulatory Operations
The Ohio State University Comprehensive Cancer Center, will provide insight into new directions in targeted therapeutic approaches for older adults with mantle cell lymphoma.
STATEMENT OF NEED
Mantle cell lymphoma (MCL) is a rare, aggressive B-cell non-Hodgkin lymphoma (NHL) accounting for 5% to 7% of all lymphomas. Its prognosis ranges from indolent disease that does not require treatment for years to very aggressive disease, which is associated with poor survival (Silkenstedt et al, 2021). Typically, MCL is diagnosed at advanced stage and in older patients who cannot tolerate intensive therapy (NCCN, 2022). Although recent advances have slightly increased remission rates, recurrence and relapse remain very common, leading to a median overall survival between 3 and 6 years (LLS, 2021). Though there are several effective options, progress is still needed towards establishing an accepted frontline approach for MCL (Castellino et al, 2022). Treatment selection and management of MCL are complicated by the heterogeneity of prognosis, advanced age and comorbidities of patients, and lack of an established standard approach for treatment, making it vital that clinicians be familiar with the latest research and advances in this area. In this activity chaired by Michael Wang, MD, Professor in the Department of Lymphoma & Myeloma at MD Anderson Cancer Center, expert faculty will discuss prognostic factors informing treatment, the promising results of recent trials in new therapeutic approaches, and the implications of treatment resistance in therapeutic selection for MCL.
Target Audience
Hematology/oncology fellows, attending faculty, and other health care professionals involved in the treatment of patients with mantle cell lymphoma (MCL).
Learning Objectives
1.) Identify clinical and biological prognostic factors that can guide treatment decision making for older adults with MCL
2.) Evaluate emerging data on targeted therapeutic approaches for treatment-naive and relapsed/refractory MCL and their applicability to older adults
3.) Assess mechanisms of resistance to targeted therapies for MCL and their implications for treatment selection
Evaluation of antidepressant activity of clitoris ternatea in animals

Evaluation of antidepressant activity of clitoris ternatea in animals
Charaka Samhita Sutra Sthana 9 Chapter khuddakachatuspadadhyaya

Charaka Samhita Sutra Sthana 9 Chapter khuddakachatuspadadhyaya
MANAGEMENT OF ATRIOVENTRICULAR CONDUCTION BLOCK.pdf

Cardiac conduction defects can occur due to various causes.
Atrioventricular conduction blocks ( AV blocks ) are classified into 3 types.
This document describes the acute management of AV block.
The POPPY STUDY (Preconception to post-partum cardiovascular function in prim...

Carmel McEniery
University of Cambridge
Surat @ℂall @Girls ꧁❤8527049040❤꧂@ℂall @Girls Service Vip Top Model Safe

Surat @ℂall @Girls ꧁❤8527049040❤꧂@ℂall @Girls Service Vip Top Model Safe
Physiology of Special Chemical Sensation of Taste

Title: Sense of Taste
Presenter: Dr. Faiza, Assistant Professor of Physiology
Qualifications:
MBBS (Best Graduate, AIMC Lahore)
FCPS Physiology
ICMT, CHPE, DHPE (STMU)
MPH (GC University, Faisalabad)
MBA (Virtual University of Pakistan)
Learning Objectives:
Describe the structure and function of taste buds.
Describe the relationship between the taste threshold and taste index of common substances.
Explain the chemical basis and signal transduction of taste perception for each type of primary taste sensation.
Recognize different abnormalities of taste perception and their causes.
Key Topics:
Significance of Taste Sensation:
Differentiation between pleasant and harmful food
Influence on behavior
Selection of food based on metabolic needs
Receptors of Taste:
Taste buds on the tongue
Influence of sense of smell, texture of food, and pain stimulation (e.g., by pepper)
Primary and Secondary Taste Sensations:
Primary taste sensations: Sweet, Sour, Salty, Bitter, Umami
Chemical basis and signal transduction mechanisms for each taste
Taste Threshold and Index:
Taste threshold values for Sweet (sucrose), Salty (NaCl), Sour (HCl), and Bitter (Quinine)
Taste index relationship: Inversely proportional to taste threshold
Taste Blindness:
Inability to taste certain substances, particularly thiourea compounds
Example: Phenylthiocarbamide
Structure and Function of Taste Buds:
Composition: Epithelial cells, Sustentacular/Supporting cells, Taste cells, Basal cells
Features: Taste pores, Taste hairs/microvilli, and Taste nerve fibers
Location of Taste Buds:
Found in papillae of the tongue (Fungiform, Circumvallate, Foliate)
Also present on the palate, tonsillar pillars, epiglottis, and proximal esophagus
Mechanism of Taste Stimulation:
Interaction of taste substances with receptors on microvilli
Signal transduction pathways for Umami, Sweet, Bitter, Sour, and Salty tastes
Taste Sensitivity and Adaptation:
Decrease in sensitivity with age
Rapid adaptation of taste sensation
Role of Saliva in Taste:
Dissolution of tastants to reach receptors
Washing away the stimulus
Taste Preferences and Aversions:
Mechanisms behind taste preference and aversion
Influence of receptors and neural pathways
Impact of Sensory Nerve Damage:
Degeneration of taste buds if the sensory nerve fiber is cut
Abnormalities of Taste Detection:
Conditions: Ageusia, Hypogeusia, Dysgeusia (parageusia)
Causes: Nerve damage, neurological disorders, infections, poor oral hygiene, adverse drug effects, deficiencies, aging, tobacco use, altered neurotransmitter levels
Neurotransmitters and Taste Threshold:
Effects of serotonin (5-HT) and norepinephrine (NE) on taste sensitivity
Supertasters:
25% of the population with heightened sensitivity to taste, especially bitterness
Increased number of fungiform papillae
Phone Us ❤85270-49040❤ #ℂall #gIRLS In Surat By Surat @ℂall @Girls Hotel With...

Phone Us ❤85270-49040❤ #ℂall #gIRLS In Surat By Surat @ℂall @Girls Hotel With 100% Satisfaction
BENIGN PROSTATIC HYPERPLASIA.BPH. BPHpdf

The prostate is an exocrine gland of the male mammalian reproductive system
It is a walnut-sized gland that forms part of the male reproductive system and is located in front of the rectum and just below the urinary bladder
Function is to store and secrete a clear, slightly alkaline fluid that constitutes 10-30% of the volume of the seminal fluid that along with the spermatozoa, constitutes semen
A healthy human prostate measures (4cm-vertical, by 3cm-horizontal, 2cm ant-post ).
It surrounds the urethra just below the urinary bladder. It has anterior, median, posterior and two lateral lobes
It’s work is regulated by androgens which are responsible for male sex characteristics
Generalised disease of the prostate due to hormonal derangement which leads to non malignant enlargement of the gland (increase in the number of epithelial cells and stromal tissue)to cause compression of the urethra leading to symptoms (LUTS
Are There Any Natural Remedies To Treat Syphilis.pdf

Explore natural remedies for syphilis treatment in Singapore. Discover alternative therapies, herbal remedies, and lifestyle changes that may complement conventional treatments. Learn about holistic approaches to managing syphilis symptoms and supporting overall health.
Report Back from SGO 2024: What’s the Latest in Cervical Cancer?

Are you curious about what’s new in cervical cancer research or unsure what the findings mean? Join Dr. Emily Ko, a gynecologic oncologist at Penn Medicine, to learn about the latest updates from the Society of Gynecologic Oncology (SGO) 2024 Annual Meeting on Women’s Cancer. Dr. Ko will discuss what the research presented at the conference means for you and answer your questions about the new developments.
For Better Surat #ℂall #Girl Service ❤85270-49040❤ Surat #ℂall #Girls

For Better Surat #ℂall #Girl Service ❤85270-49040❤ Surat #ℂall #Girls
Lung Cancer: Artificial Intelligence, Synergetics, Complex System Analysis, S...

RESULTS: Overall life span (LS) was 2252.1±1742.5 days and cumulative 5-year survival (5YS) reached 73.2%, 10 years – 64.8%, 20 years – 42.5%. 513 LCP lived more than 5 years (LS=3124.6±1525.6 days), 148 LCP – more than 10 years (LS=5054.4±1504.1 days).199 LCP died because of LC (LS=562.7±374.5 days). 5YS of LCP after bi/lobectomies was significantly superior in comparison with LCP after pneumonectomies (78.1% vs.63.7%, P=0.00001 by log-rank test). AT significantly improved 5YS (66.3% vs. 34.8%) (P=0.00000 by log-rank test) only for LCP with N1-2. Cox modeling displayed that 5YS of LCP significantly depended on: phase transition (PT) early-invasive LC in terms of synergetics, PT N0—N12, cell ratio factors (ratio between cancer cells- CC and blood cells subpopulations), G1-3, histology, glucose, AT, blood cell circuit, prothrombin index, heparin tolerance, recalcification time (P=0.000-0.038). Neural networks, genetic algorithm selection and bootstrap simulation revealed relationships between 5YS and PT early-invasive LC (rank=1), PT N0—N12 (rank=2), thrombocytes/CC (3), erythrocytes/CC (4), eosinophils/CC (5), healthy cells/CC (6), lymphocytes/CC (7), segmented neutrophils/CC (8), stick neutrophils/CC (9), monocytes/CC (10); leucocytes/CC (11). Correct prediction of 5YS was 100% by neural networks computing (area under ROC curve=1.0; error=0.0).
CONCLUSIONS: 5YS of LCP after radical procedures significantly depended on: 1) PT early-invasive cancer; 2) PT N0--N12; 3) cell ratio factors; 4) blood cell circuit; 5) biochemical factors; 6) hemostasis system; 7) AT; 8) LC characteristics; 9) LC cell dynamics; 10) surgery type: lobectomy/pneumonectomy; 11) anthropometric data. Optimal diagnosis and treatment strategies for LC are: 1) screening and early detection of LC; 2) availability of experienced thoracic surgeons because of complexity of radical procedures; 3) aggressive en block surgery and adequate lymph node dissection for completeness; 4) precise prediction; 5) adjuvant chemoimmunoradiotherapy for LCP with unfavorable prognosis.
The Normal Electrocardiogram - Part I of II

These lecture slides, by Dr Sidra Arshad, offer a quick overview of physiological basis of a normal electrocardiogram.
Learning objectives:
1. Define an electrocardiogram (ECG) and electrocardiography
2. Describe how dipoles generated by the heart produce the waveforms of the ECG
3. Describe the components of a normal electrocardiogram of a typical bipolar leads (limb II)
4. Differentiate between intervals and segments
5. Enlist some common indications for obtaining an ECG
Study Resources:
1. Chapter 11, Guyton and Hall Textbook of Medical Physiology, 14th edition
2. Chapter 9, Human Physiology - From Cells to Systems, Lauralee Sherwood, 9th edition
3. Chapter 29, Ganong’s Review of Medical Physiology, 26th edition
4. Electrocardiogram, StatPearls - https://www.ncbi.nlm.nih.gov/books/NBK549803/
5. ECG in Medical Practice by ABM Abdullah, 4th edition
6. ECG Basics, http://www.nataliescasebook.com/tag/e-c-g-basics
Recently uploaded (20)
New Directions in Targeted Therapeutic Approaches for Older Adults With Mantl...

New Directions in Targeted Therapeutic Approaches for Older Adults With Mantl...
Evaluation of antidepressant activity of clitoris ternatea in animals

Evaluation of antidepressant activity of clitoris ternatea in animals
Charaka Samhita Sutra Sthana 9 Chapter khuddakachatuspadadhyaya

Charaka Samhita Sutra Sthana 9 Chapter khuddakachatuspadadhyaya
MANAGEMENT OF ATRIOVENTRICULAR CONDUCTION BLOCK.pdf

MANAGEMENT OF ATRIOVENTRICULAR CONDUCTION BLOCK.pdf
The POPPY STUDY (Preconception to post-partum cardiovascular function in prim...

The POPPY STUDY (Preconception to post-partum cardiovascular function in prim...
Surat @ℂall @Girls ꧁❤8527049040❤꧂@ℂall @Girls Service Vip Top Model Safe

Surat @ℂall @Girls ꧁❤8527049040❤꧂@ℂall @Girls Service Vip Top Model Safe
Phone Us ❤85270-49040❤ #ℂall #gIRLS In Surat By Surat @ℂall @Girls Hotel With...

Phone Us ❤85270-49040❤ #ℂall #gIRLS In Surat By Surat @ℂall @Girls Hotel With...
Are There Any Natural Remedies To Treat Syphilis.pdf

Are There Any Natural Remedies To Treat Syphilis.pdf
Report Back from SGO 2024: What’s the Latest in Cervical Cancer?

Report Back from SGO 2024: What’s the Latest in Cervical Cancer?
For Better Surat #ℂall #Girl Service ❤85270-49040❤ Surat #ℂall #Girls

For Better Surat #ℂall #Girl Service ❤85270-49040❤ Surat #ℂall #Girls
Maxilla, Mandible & Hyoid Bone & Clinical Correlations by Dr. RIG.pptx

Maxilla, Mandible & Hyoid Bone & Clinical Correlations by Dr. RIG.pptx
Lung Cancer: Artificial Intelligence, Synergetics, Complex System Analysis, S...

Lung Cancer: Artificial Intelligence, Synergetics, Complex System Analysis, S...
Muscular system-and-nervous-system
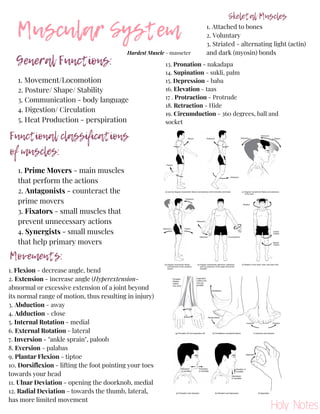
- 1. Muscular System General Functions: 1. Movement/Locomotion 2. Posture/ Shape/ Stability 3. Communication - body language 4. Digestion/ Circulation 5. Heat Production - perspiration 1. Prime Movers - main muscles that perform the actions 2. Antagonists - counteract the prime movers 3. Fixators - small muscles that prevent unnecessary actions 4. Synergists - small muscles that help primary movers Functional classifications of muscles: Skeletal Muscles 1. Attached to bones 2. Voluntary 3. Striated - alternating light (actin) and dark (myosin) bonds Movements: 1. Flexion - decrease angle, bend 2. Extension - increase angle (Hyperextension- abnormal or excessive extension of a joint beyond its normal range of motion, thus resulting in injury) 3. Abduction - away 4. Adduction - close 5. Internal Rotation - medial 6. External Rotation - lateral 7. Inversion - "ankle sprain", paloob 8. Eversion - palabas 9. Plantar Flexion - tiptoe 10. Dorsiflexion - lifting the foot pointing your toes towards your head 11. Ulnar Deviation - opening the doorknob, medial 12. Radial Deviation - towards the thumb, lateral, has more limited movement Hardest Muscle - masseter 13. Pronation - nakadapa 14. Supination - sukli, palm 15. Depression - baba 16. Elevation - taas 17 . Protraction - Protrude 18. Retraction - Hide 19. Circumduction - 360 degrees, ball and socket Holy Notes
- 2. Muscular System Two points of attachment: Holy Notes 1. Origin - relatively fixed/ proximal 2. Insertion - where you expect movement/ distal Two ways by which the muscles develops: 1. Hypertrophy- increase in diameter of the muscle fibers 2. Hyperplasia - increase in number of muscle fibers Names of muscle 1. Occipitofrontalis - wrinkles in the forehead 2. Orbicularis oculi - blinking/ winking muscle 3. Orbicularis oris - kissing muscle 4. Buccinator - blowing muscle 5. Masseter- strongest muscle 6. Zygomaticus - smiling muscle 7. Trapezius - elevates shoulder/ stressed/ stiff neck (muscle spasm) 8. Sternocleidomastoid (SCM)- flexes the neck 9. Deltoid - forms the bulk of your shoulder 10. Pectoralis Major - 11. Serratus - saw muscle 12. Latissimus Dorsi - 13. Gluteus Maximus - hip extension; Gluteus Medius - supports the hip 14. Hamstring - PM for knee flexion 15. Gastrocnemius - PM for ankle-plantar flexion 16. Quadriceps Femoris 17. Sartorius - longest muscle 18. Anterior Tibialis - PM for ankle dorsiflexion
- 3. Nervous System Anatomical Division Holy Notes 1. Central Nervous System : brain & spinal cord 2. Peripheral Nervous System : cranial nerves (12 pairs), spinal nerves (31 pairs), ganglia Functional Divisions 1. Somatic NS (skeletal muscles) - voluntary movements 2. Autonomic NS (smooth and cardiac) - involuntary movements; sympathetic division, parasympathetic division; Fight and flight Spinal Nerves 7 cervical bones = 8 cervical nerve roots (1 above each bone) 12 thoracic vertebrae = 12 nerve roots (1 above each thoracic vertebrae) 5 lumbar = 5 5 sacral = 5 1 coccyx = 1 Cranial Nerves I. Olfactory (se) II. Optic (se) III. Occulomotor (mo) IV. Trochlear (mo) V. Trigeminal (mi) VI. Abducens (mo) VII. Facial (mi) VIII. Auditory (se) IX. Glossopharyngeal (mi) X. Vagus (mi) XI. Accessory (mo) XII. Hypoglossal (mo) Classification of nerves: SENSORY - Afferent; environment to the brain or spinal cord MOTOR - Efferent (Contraction & Secretion) MIXED - both sensory and motor If ever na kulang po yung notes ko sorry po kasi ang bilis maglesson ni sir hehe saka areng notes na are ay halo halo din nanguha ako from other classmates hihi -yloh
