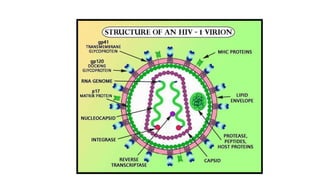
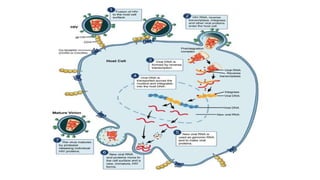
This document discusses HIV and its relationship to surgeons. It provides an overview of HIV, including its history, epidemiology, structure, life cycle, and pathophysiology. It then discusses how HIV impacts surgeons, including managing HIV-positive patients before, during, and after surgery. It also covers factors that affect HIV transmission risk, how to handle needle sticks or exposure to bodily fluids, and the use of post-exposure prophylaxis. The document concludes by noting how HIV affects surgeons in operating on patients with or without HIV-related conditions.