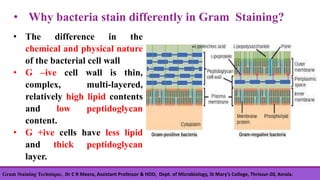
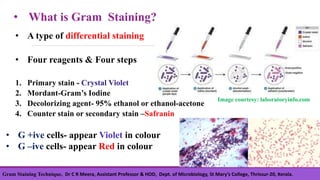
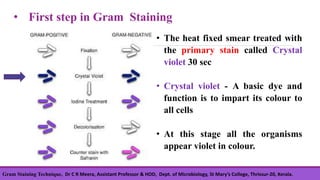
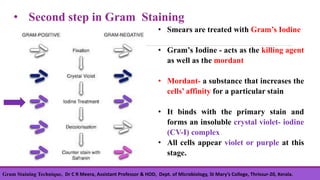
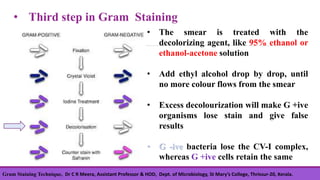
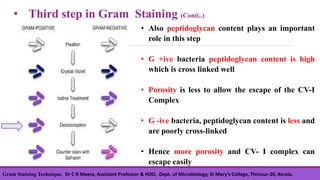
Gram staining is a differential staining technique developed by Christian Gram in 1880, crucial for classifying bacteria into gram-positive and gram-negative groups based on cell wall composition. The process involves four main steps: applying crystal violet, using gram's iodine as a mordant, decolorizing with ethanol, and counterstaining with safranin, with positive cells retaining the violet color and negative cells taking on a red hue. Understanding the chemical differences in bacterial cell walls is essential for interpreting gram staining results.