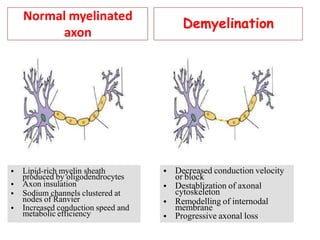
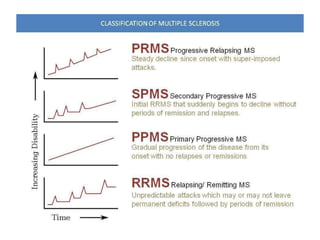
The document provides a comprehensive overview of demyelination and its key aspects, particularly focusing on multiple sclerosis (MS), a chronic degenerative disorder characterized by inflammation, demyelination, and gliosis. It discusses the disease's epidemiology, risk factors, pathophysiology, clinical features, diagnosis, and management strategies, emphasizing the importance of MRI and clinical findings in diagnosing MS. Furthermore, it outlines the various clinical presentations and types of MS, as well as treatment options such as corticosteroids and disease-modifying therapies.