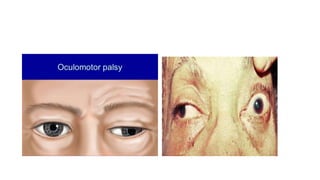
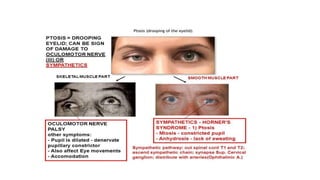
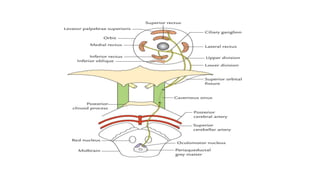
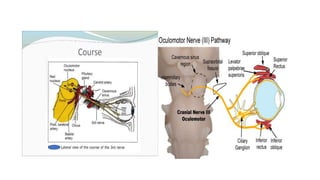
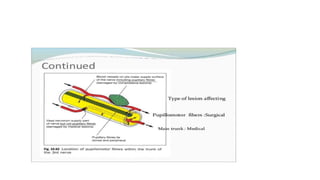
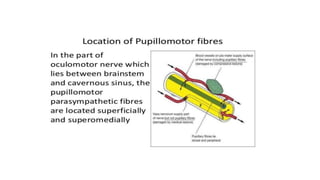
The document discusses congenital and acquired oculomotor nerve palsy, a rare condition predominantly affecting children, with various causes including trauma, inflammation, and genetic factors. It outlines diagnostic approaches, clinical findings, and management strategies, emphasizing the need for imaging and careful examination to prevent complications such as amblyopia. Treatment options include both conservative measures and surgical interventions, tailored to the specific needs and anatomical variations of the patient.