This document provides an overview of bronchial asthma, including its definition, pathophysiology, types, triggers, symptoms, diagnosis, management, and differences from COPD. Key points include:
- Asthma is a disease characterized by reversible airway obstruction and inflammation in response to various stimuli. It is an IgE-mediated hypersensitivity reaction.
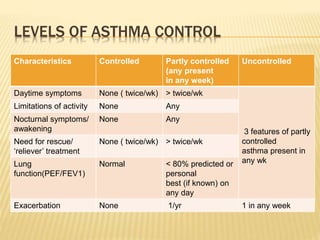
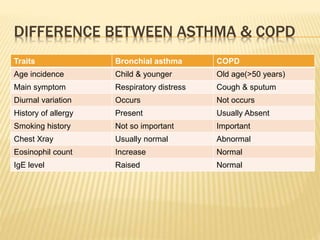
- Common symptoms include wheezing, chest tightness, cough and breathlessness. Diagnosis is based on clinical history and pulmonary function tests showing improved airflow with bronchodilators.
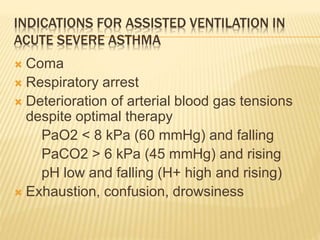
- Management involves avoidance of triggers, bronchodilators, inhaled corticosteroids, and a stepped treatment plan escalating medications based on asthma control. Acute