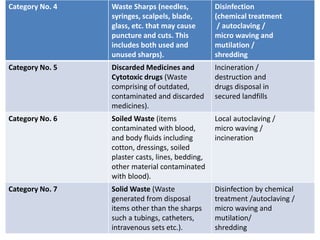
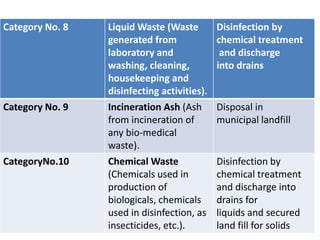
This document discusses bio-medical waste management. It defines bio-medical waste and outlines the dangers of improper management, which can lead to public health hazards and environmental pollution. It describes the sources and categories of healthcare waste and how waste should be treated and disposed of according to regulations. Methods of treatment discussed include incineration, chemical disinfection, thermal treatment, and land disposal. The document also provides information on bio-medical waste management in India, including generation amounts, treatment facilities, and an example of a common treatment facility called IMAGE in Kerala.