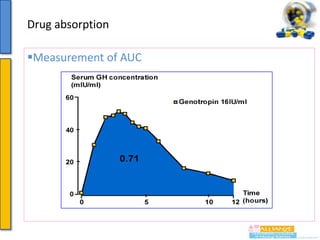
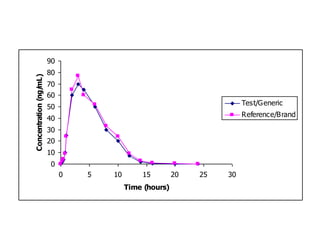
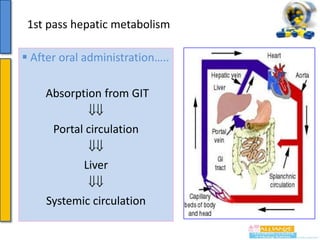
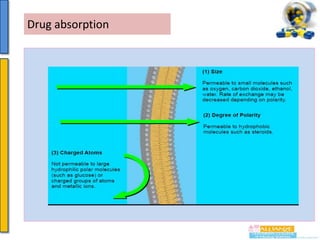
This document provides an overview of pharmacokinetics and drug absorption. It defines key terms like bioavailability, discusses factors that influence drug absorption like lipid solubility and ionization, and mechanisms of drug transport including passive diffusion. Specific topics covered include the first-pass effect, importance of drug and environmental pH on absorption, and how molecular weight impacts absorption. Measurement of areas under the curve is presented as a method for assessing bioavailability.













![Lipid Diffusion
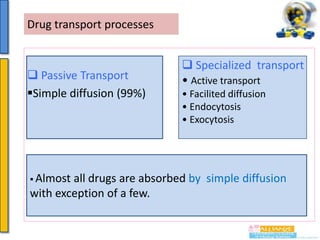
•
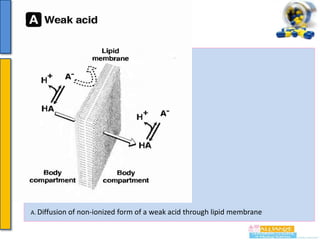
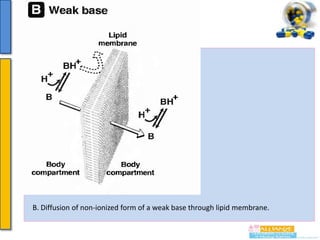
In the case of weak acids and weak bases the ability to move
from aqueous to lipid or vice versa varies with the pH of the
medium.
•
Henderson-Hasselbalch equation (can be use to predict
the effect of pH change on ABSORPTION):
Acid: pH = pKa + log [A-]/[HA]
Base: pH = pKa + log [B]/ [HB+]](https://image.slidesharecdn.com/drugabsorption-131026003926-phpapp01/85/Drug-absorption-22-320.jpg)








![Where
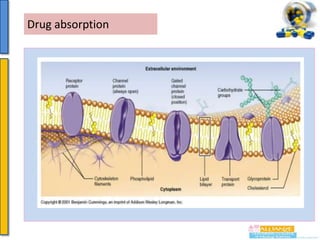
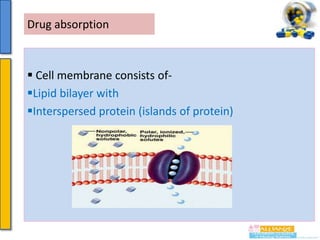
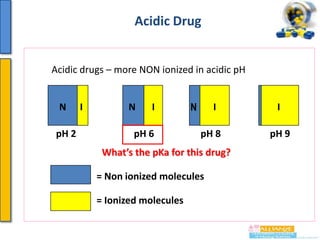
Drug absorption more
drug???
Acid: pH = pKa + log [A-]/[HA]
Log [A-]/[HA] = (pH – pKa)
[A-]/[HA] = 10 (pH –pKa)
In plasma:
[A-]/[HA] = 10 (7.4-3.4) = 104 =10,000
In gastric juice:
[A-]/[HA] = 10 (1.4-3.4) = 10-2 = 0.01](https://image.slidesharecdn.com/drugabsorption-131026003926-phpapp01/85/Drug-absorption-35-320.jpg)