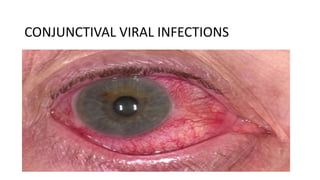
This document discusses conjunctival viral infections, summarizing:
1) Adenovirus is the most common cause, responsible for over 90% of cases, and can cause nonspecific acute follicular conjunctivitis, pharyngoconjunctival fever, or epidemic keratoconjunctivitis.
2) Other causes include herpes simplex, herpes zoster, enteroviruses, poxviruses, cytomegalovirus, and molloscum contagiosum.
3) Symptoms vary but generally include redness, irritation, watering and photophobia, while signs involve eyelid edema and conjunctival hyperemia and follicles.