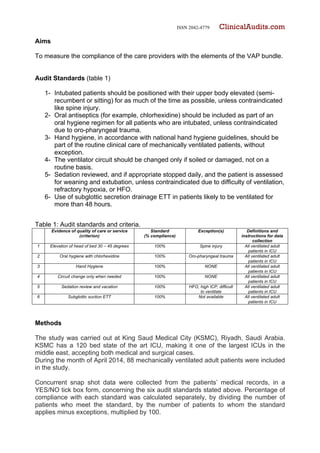
This study aimed to measure compliance with ventilator-associated pneumonia (VAP) bundle components in an intensive care unit (ICU) in Saudi Arabia. An audit of 88 mechanically ventilated patients found high compliance (87.5-100%) with hand hygiene, mouth care, and avoiding routine ventilator tubing changes. Compliance was lower for head-of-bed elevation (95.2%) and daily sedation vacations (65.5%). No patients received endotracheal tubes with subglottic suction ports due to unavailability. The authors recommend increasing education, minimizing provider workload, improving equipment maintenance, and ensuring access to recommended ventilation equipment.