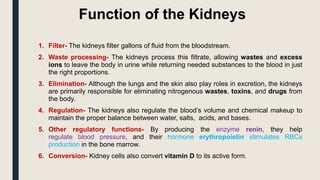
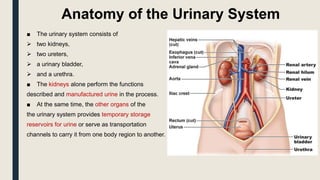
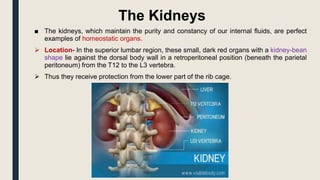
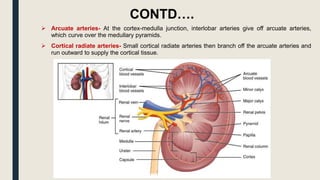
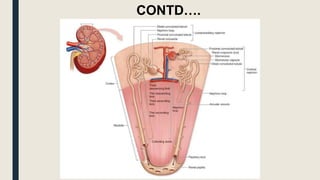
The document summarizes the structure and function of the urinary system. It describes how the kidneys filter waste from the bloodstream and regulate fluid and electrolyte balance through millions of nephrons. Urine is transported from the kidneys to the bladder via ureters. The bladder stores urine temporarily before it is emptied through the urethra. Together, these organs work to eliminate waste from the body while maintaining homeostasis.