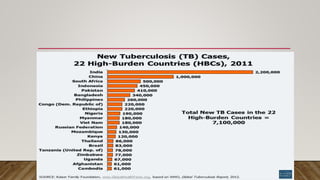
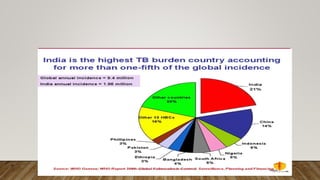
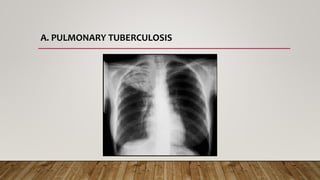
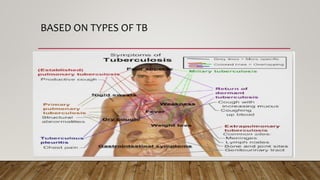
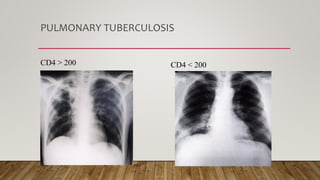
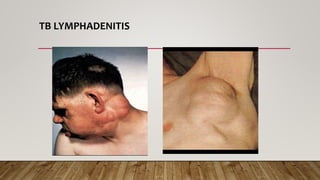
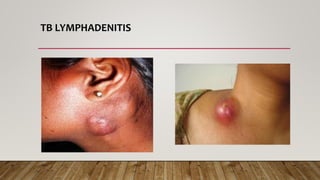
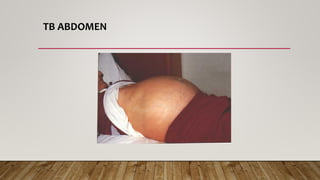
The document provides a comprehensive overview of tuberculosis (TB), including its definition, causative organisms, epidemiology, risk factors, clinical presentation, and diagnosis processes. It details the differences between pulmonary and extrapulmonary TB, the diagnostic methods used, and the challenges posed by drug-resistant forms like MDR-TB and XDR-TB. It emphasizes the importance of early diagnosis and effective treatment strategies to manage TB and prevent its spread, particularly in high-burden regions.