This document discusses the purposes and techniques of taping in physical therapy. It can be summarized as follows:
1) Taping is used for a variety of purposes including support, protection, pain relief, edema control, and injury prevention. It works through biomechanical and neurophysiological mechanisms.
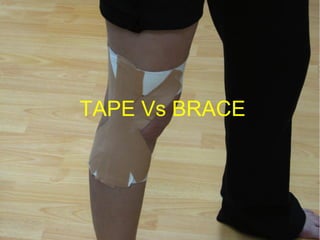
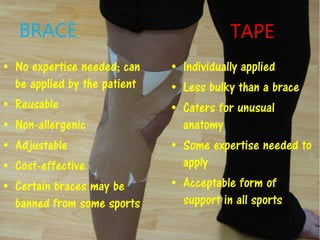
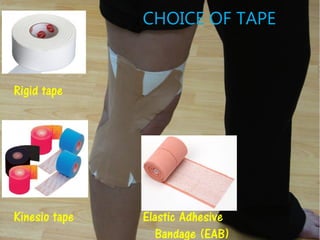
2) There are different types of tape that are used including rigid tape, elastic adhesive bandages, and kinesio tape. The choice depends on the intended purpose and injury stage.
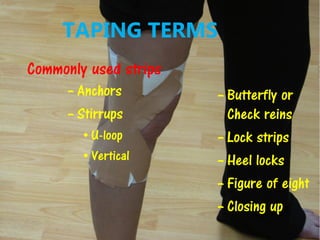
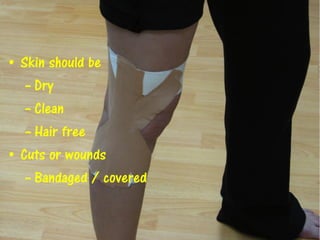
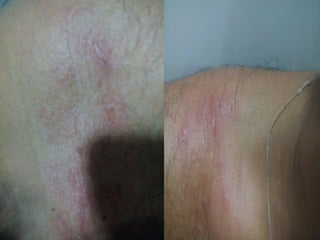
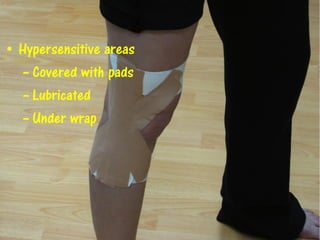
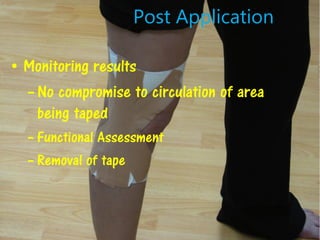
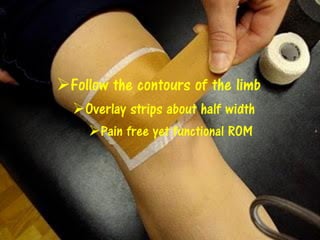
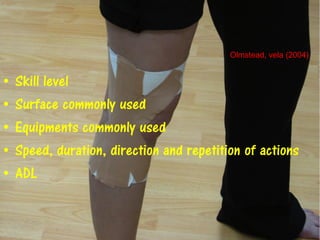
3) Proper taping requires assessment of the injury, skin preparation, and application using specific techniques. Ongoing monitoring is needed to ensure the tape remains functional without compromising circulation. Extensive practice is required to master