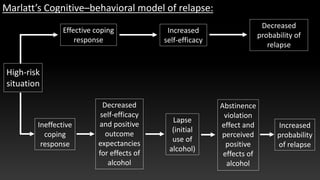
The document provides an overview of cognitive behavioral therapy (CBT) as a method for managing emotional and behavioral issues, emphasizing its role in relapse prevention (RP) for individuals recovering from substance abuse. It discusses the importance of identifying high-risk situations, developing effective coping strategies, and the cognitive-behavioral model in addressing relapses. Additionally, it highlights intervention strategies and the significance of supportive social networks in maintaining recovery.