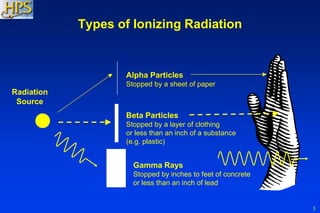
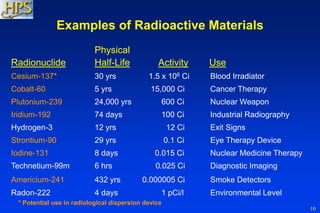
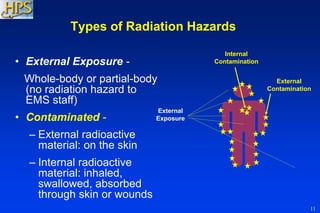
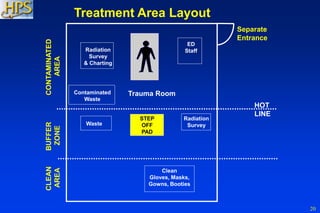
The document provides a comprehensive overview for training emergency department staff on the management of radiation casualties, including the characteristics of ionizing radiation, differentiation between exposure and contamination, and procedures for patient assessment and decontamination. It highlights the importance of facility preparation, staff safety measures, and psychological support for affected individuals. The guidelines emphasize triage, patient management, decontamination priorities, and resources for effective response during radiation emergencies.