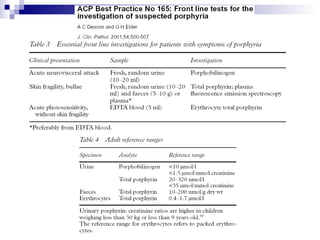
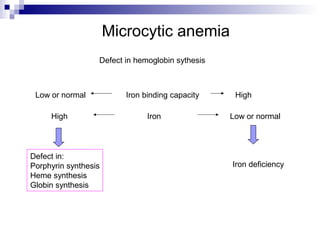
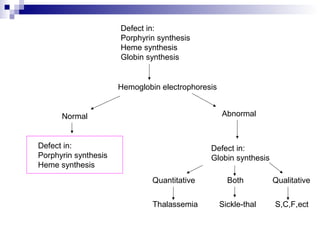
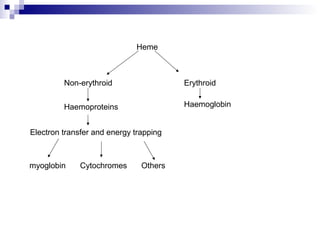
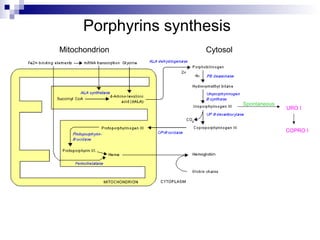
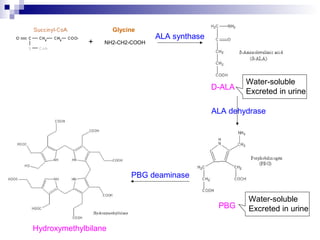
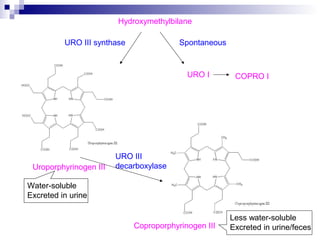
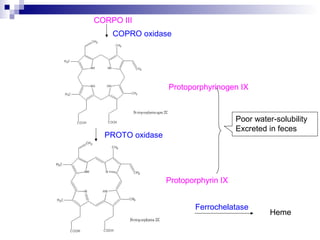
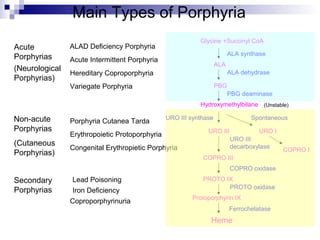
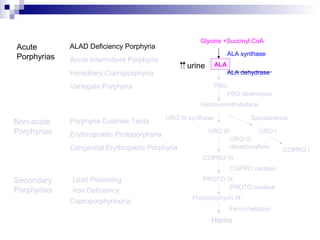
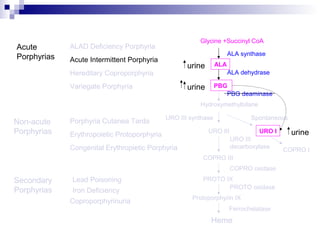
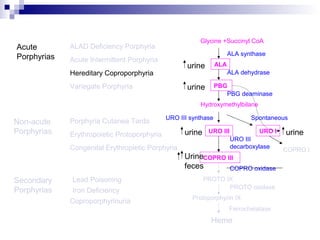
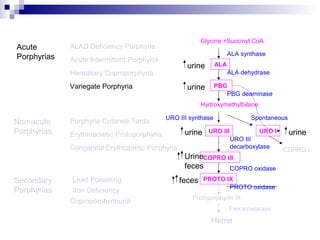
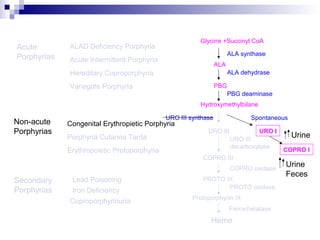
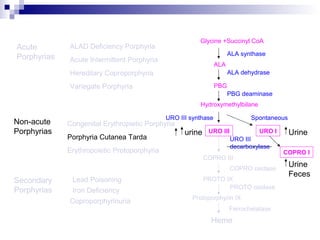
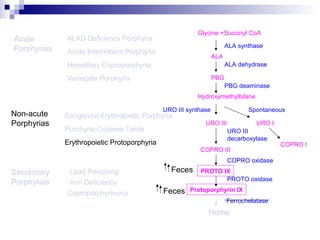
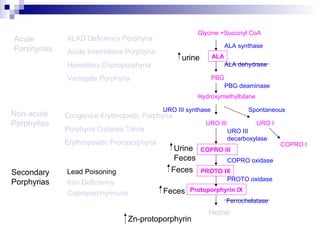
This document discusses various types of porphyrias, which are disorders of heme biosynthesis. It describes the pathways of porphyrin synthesis and the enzymes involved at each step. It then classifies the main types of porphyria as either acute or non-acute, and lists examples such as acute intermittent porphyria, variegate porphyria, hereditary coproporphyria, porphyria cutanea tarda, congenital erythropoietic porphyria, ALAD deficiency porphyria, and erythropoietic protoporphyria. It indicates the tissues affected, inheritance, and abnormal metabolites detected in urine, feces, or blood for each type of porphy











![General Symptomology:
__Abdominal pain
___Abdominal tenderness
___Loss of appetite
___Nausea
___Vomiting
___Constipation
___Carbohydrate craving
___Breast secretions
___Diarrhea
___Partial ileus [Intestinal blockage]
___Abdominal distention
___Dysuria [Painful Urination]
___Bladder Dysfunction
___Urinary Retention
___Amenorrhea [Lack of menses]
Physical Findings of Acute Attack
__Red or dark urine
___Tachycardia [Pulse] >100
___Labile hypertension >90 diastolic [blood pressure]
___Fever [Pyrexia]
___Profused sweating
___Edema [Retention of fluids] [Swelling]
___Postural Hypotension [Low Blood Pressure]
___Hypertrichosis [excessive body hair growth]
___Hyperpigmentation [skin coloring]](https://image.slidesharecdn.com/porphyria-r1-150111094442-conversion-gate01/85/Porphyria-r-1-29-320.jpg)
![Neurological Symptoms of Acute Attack
[Peripheral manifestations]
___Peripheral neuropathy
___Muscle weakness
___Paresis . paralysis
___Sensory disorde
___Respiratory paralysis
___Foot drop
___Wrist drop
___Abnormal Gait
___Pain: Arms, legs, hips and/or lower back
___Loss of sensation
___Dyesthesia
___Numbness
___Tingling
___Burning Sensation
___Bulbar paresis
___Tongue paralization
___Mouth paralization
___Throat paralization
[Cerebral manifestations]
___Behavorial change
___Anxiety
___Irritability
___Delirium
___Depression
___Confusion
___Hallucination
___Insomnia
___ANS [altered neurological state]
___Restlessness
___Sensory loss
___Seizure
___Depressed or absent tendon reflexes
___Cranial nerve involvement](https://image.slidesharecdn.com/porphyria-r1-150111094442-conversion-gate01/85/Porphyria-r-1-30-320.jpg)
![Hematology/Blood Chemistry
___Hyponatremia [Below normal sodium level] <130
___Increased Bun [Urea Nitrogen]
___Increased AST [Aspartate Aminotransferase]
___Elevated Alkaline Phosphatase [Liver panel test]
___Increased ALT [Aspartate Aminotransferase]
___Hypokalemia [Below normal potassium level]
___Leukocytosis [Abnormal increase in WBC] > 10,000
___Increased ESR >22
___Hypochloremia < 90 [A decrease in the chloride level]
___Anemia [Iron deficiency]
Cutaneous manifestations
___Skin photosensitivity
___Blistering
___Severe Tissue Scarring
___Increased Hair growth
___Pigmentation Darkening
___Thickening of skin
___Severe Itching
Special lab studies
___Decreased blood volume
___EEG abnormalities
___Electromyographic abnormalities
___Muscle denervation
___Decreased nerve conduction velocity
___Abnormal CSF
___Increased fibrillation potential](https://image.slidesharecdn.com/porphyria-r1-150111094442-conversion-gate01/85/Porphyria-r-1-31-320.jpg)