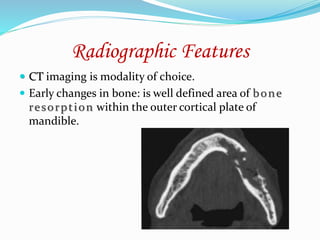
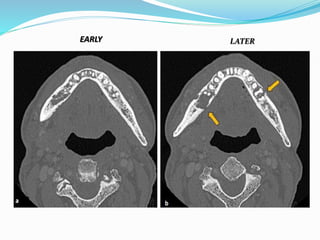
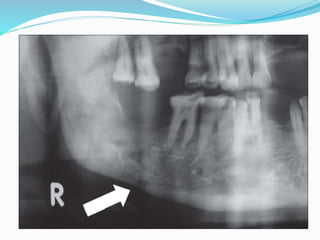
Osteoradionecrosis is an inflammatory bone condition that occurs after exposure to therapeutic radiation doses, usually for head and neck cancers. It is characterized by exposed bone for at least 3 months after radiation therapy. The mandible is most commonly affected due to its anatomy and low vascularity. Management includes conservative approaches like antibiotics and debridement to maintain bone integrity and prevent infection, as well as hyperbaric oxygen therapy to reduce hypoxia and improve healing. Prevention involves dental work before radiation and careful oral hygiene during and after treatment.