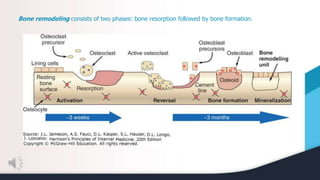
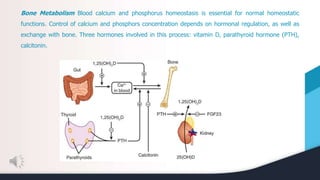
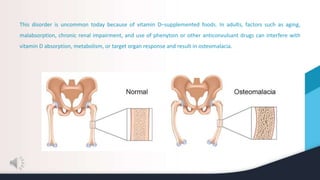
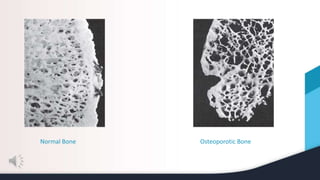
This document summarizes and compares osteomalacia and osteoporosis. It begins with background on bone structure and remodeling and the role of calcium, phosphorus, and hormones like vitamin D and parathyroid hormone in bone metabolism. It then describes osteomalacia as a disease of inadequate bone mineralization typically due to vitamin D deficiency, preventing calcium absorption and weakening bones. Osteoporosis is characterized by gradual bone mass loss and weakness, influenced by aging, nutrition, and other risk factors. While both result in fragile bones that fracture easily, osteomalacia specifically involves low blood calcium and decreased mineralization compared to normal mineralization in osteoporosis.