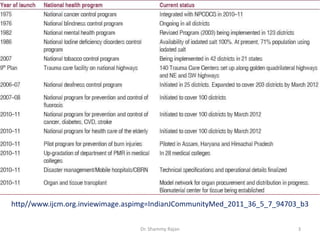
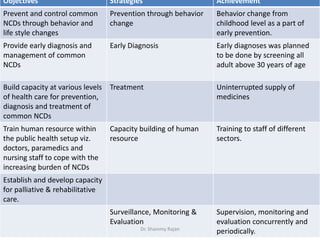
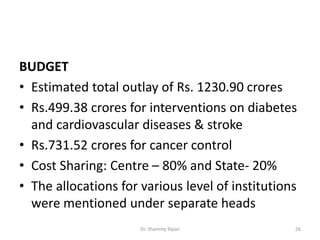
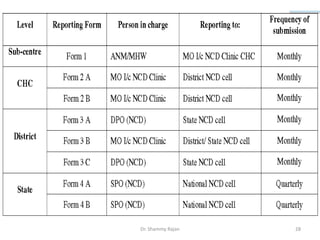
This document summarizes India's National Programme for Prevention and Control of Cancer, Diabetes, Cardiovascular diseases and Stroke (NPCDCS). It began as separate programs in the 1970s and was established as a national program in 2008, aiming to prevent and control non-communicable diseases through early diagnosis, management, building healthcare capacity, and changing behaviors. The program was implemented in 100 districts across 15 states by 2011-2012 but faced issues with lack of sustained funding, poor infrastructure development, and minimal prevention efforts.

























![References
1. Harper K, Armelagos G. The Changing Disease-Scape in the Third Epidemiological
Transition. Int J Environ Res Public Health. 2010 Feb;7(2):675–97.
2. Agyei-Mensah S, de-Graft Aikins A. Epidemiological Transition and the Double
Burden of Disease in Accra, Ghana. J Urban Health Bull N Y Acad Med. 2010
Sep;87(5):879–97.
3. Albala C, Vio F, Yáñez M. [Epidemiological transition in Latin America: a
comparison of four countries]. Rev Médica Chile. 1997 Jun;125(6):719–27.
4. Amuna P, Zotor FB. Epidemiological and nutrition transition in developing countries:
impact on human health and development. Proc Nutr Soc. 2008 Feb;67(1):82–90.
5. Victora CG, Hanson K, Bryce J, Vaughan JP. Achieving universal coverage with
health interventions. The Lancet. 2004 Oct 29;364(9444):1541–8.
6. Duran A, Khot A. Strengthening the Health System to Better Confront
Noncommunicable Diseases in India. Indian J Community Med Off Publ Indian
Assoc Prev Soc Med. 2011 Dec;36(Suppl1):S32–S37.
33Dr. Shammy Rajan](https://image.slidesharecdn.com/ncdpolicyanalysis-140801030651-phpapp01/85/Non-Communicable-Diseases-Policy-of-India-An-analysis-33-320.jpg)
