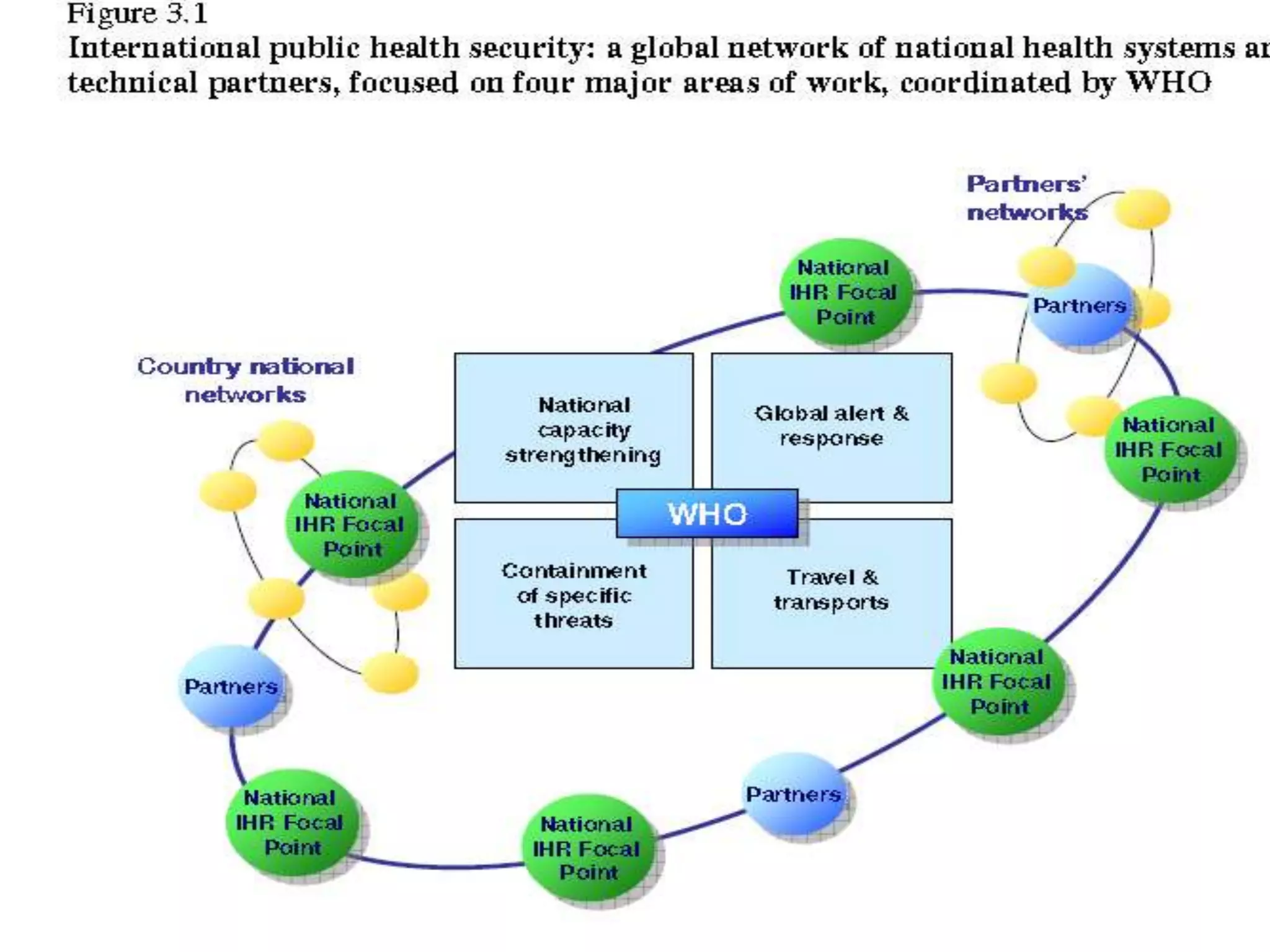
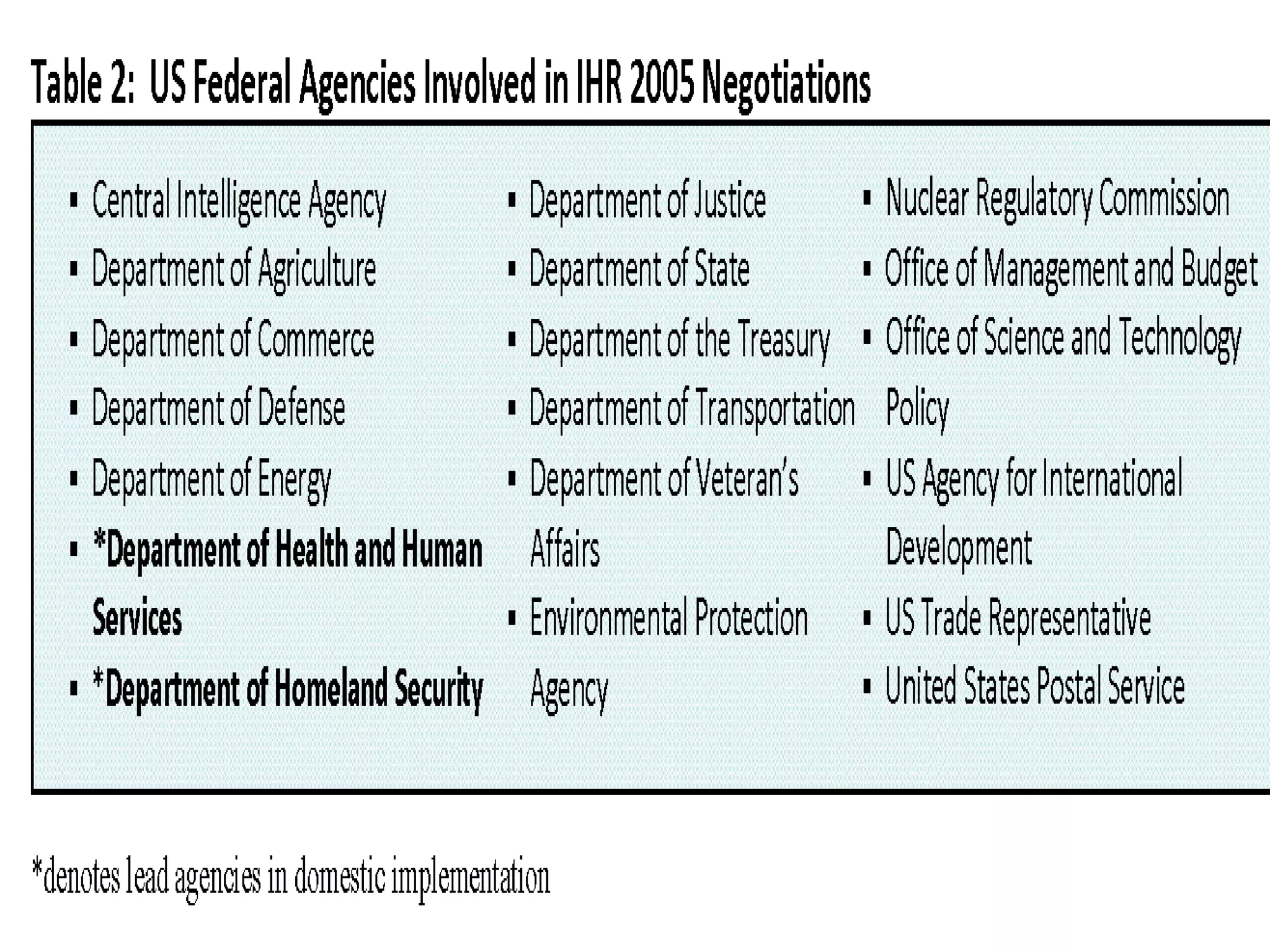
The International Health Regulations originated in 1851 to promote international cooperation and limit interference with trade during disease outbreaks. The IHR have been revised multiple times to address new public health challenges, including the 2005 revision to strengthen surveillance and response systems for infectious diseases and public health emergencies. The IHR (2005) require countries to develop core surveillance and response capacities and obligate information sharing during public health events of international concern in order to rapidly detect and respond to global health threats.