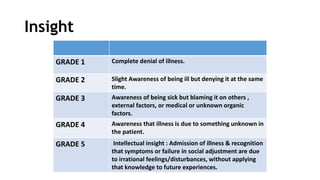
This document provides an overview of how to conduct a mental status examination (MSE). An MSE systematically evaluates a patient's appearance, behavior, mood, thought processes, cognition and insight. It covers domains like speech, thought content, perception, orientation, attention/concentration, memory, intelligence and judgment. The MSE gives clinicians a snapshot of a patient's current mental well-being and helps with diagnostic formulation and treatment planning. A thorough MSE is an important psychiatric evaluation tool.