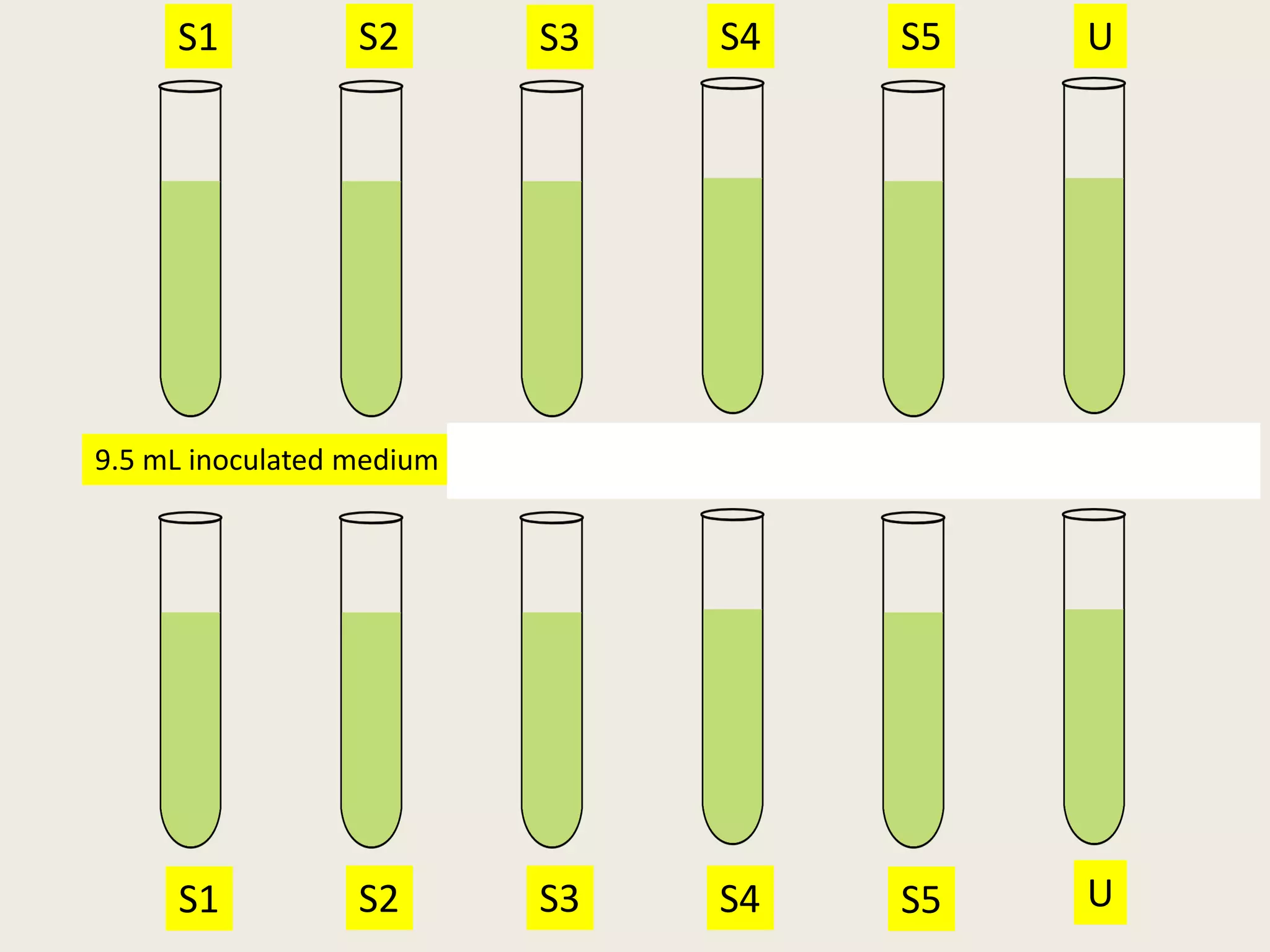
This document describes the microbiological assay method for quantifying antibiotics. It involves preparing standard solutions of known antibiotic concentrations and measuring their zones of inhibition against a test microbe. An unknown sample is also tested and its zone of inhibition is compared to the standard curve to determine its concentration. The key steps are:
1) Preparing standard solutions in increasing concentrations and an unknown at a median level.
2) Inoculating agar plates with a test microbe and creating wells for the solutions.
3) Measuring the zones of inhibition and calculating averages for the standards.
4) Comparing the unknown's zone of inhibition to the standard curve to determine its concentration.