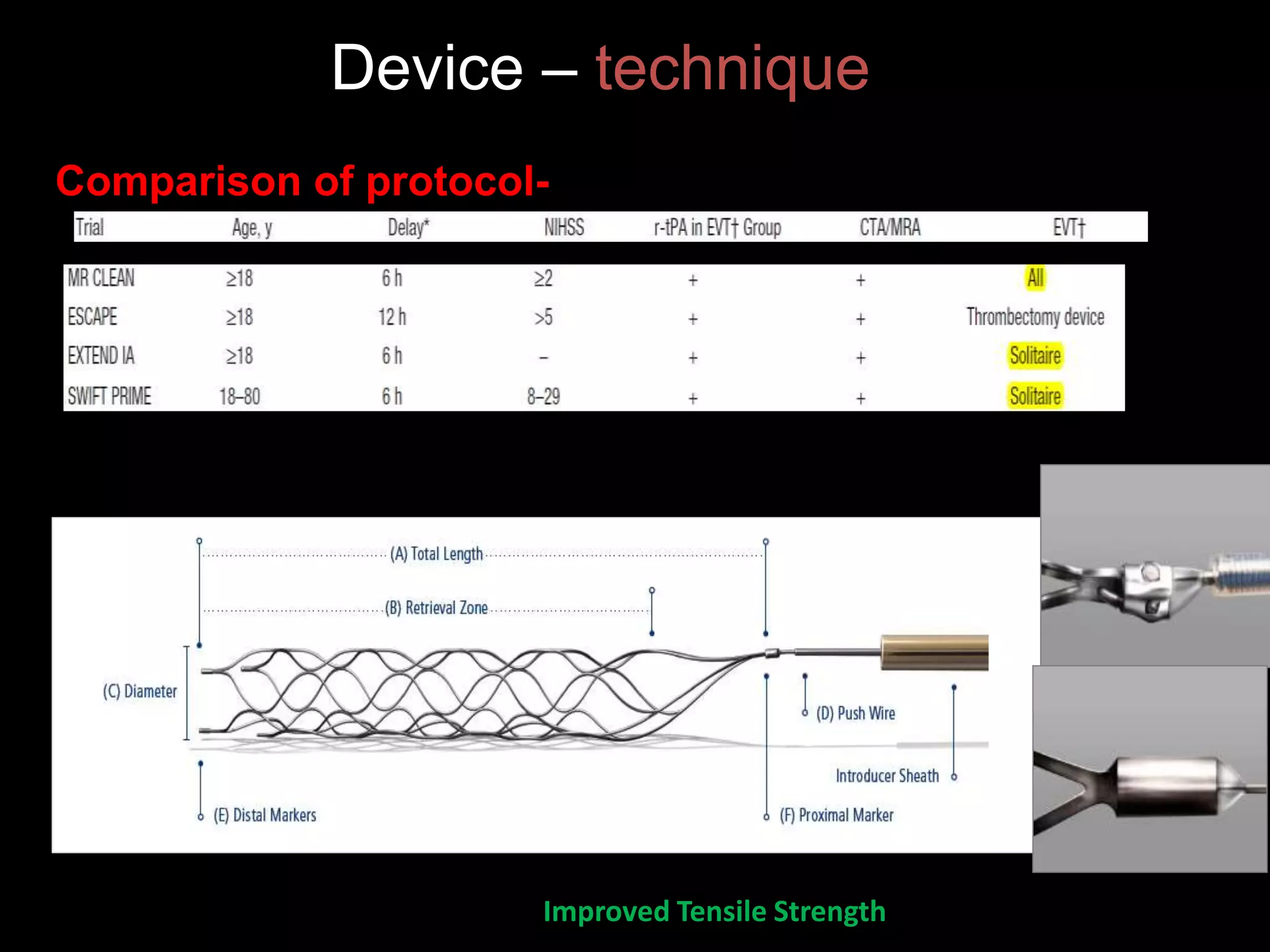
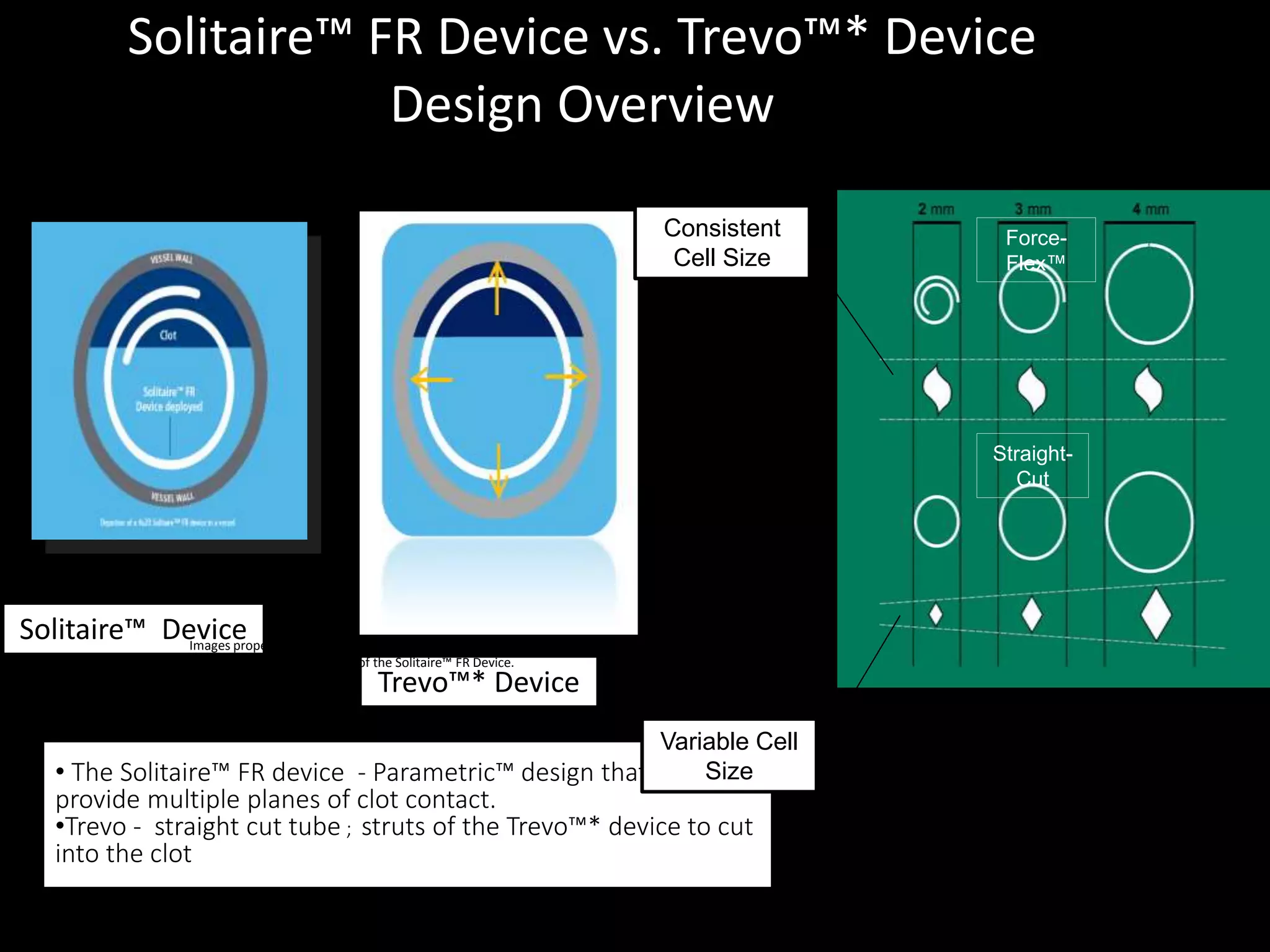
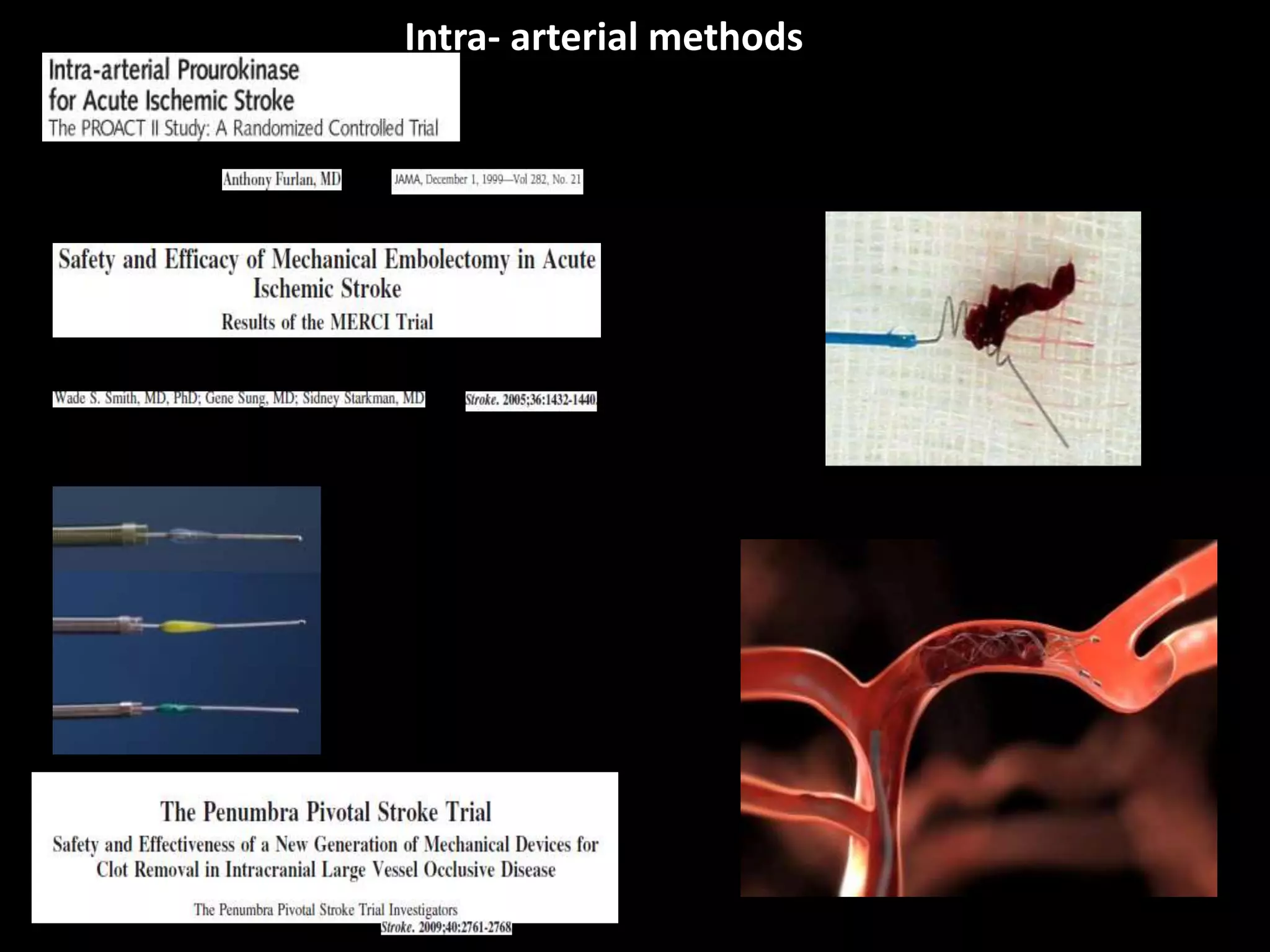
Vipul Gupta discusses balloon assisted coiling in ruptured cerebral aneurysms and mechanical thrombectomy with stent retrievers. He summarizes several key randomized controlled trials that demonstrated the benefits of endovascular therapy using stent retrievers over standard medical therapy alone for acute ischemic stroke. The trials showed significant improvements in revascularization, clinical outcomes, and mortality. The 2015 AHA/ASA guidelines recommend endovascular therapy with stent retrievers for select patients within 6 hours of stroke onset based on the evidence from these trials. The document also reviews techniques for mechanical thrombectomy and strategies to optimize outcomes.



























![980 patients: GA in 44%
Poor neurological outcome:
OR 2.3 (with GA)
Higher mortality: OR 1.6 (with
GA)
1956 patients: GA in 41%
Good outcome: OR 0.5 (with GA)
Higher mortality: OR 2.5 (with GA)
Successful angiographic outcome:
OR 0.5 (with GA)
• Sedation vs Intubation for Endovascular Stroke TreAtment
Trial (SIESTA) is a prospective, randomised controlled,
monocentric, two-armed, comparative trial.
• ESOC - We did not see a difference in the primary outcome of
change in NIHSS [National Institutes of Health Stroke Severity]
score at 24 hours between patients receiving general
anesthesia and those given conscious sedation," he
concluded. "However, this data is preliminary and we don't
yet have the main secondary outcome of modified Rankin
scores at 3 months. These will be reported at the World
Stroke Congress in October](https://image.slidesharecdn.com/acutestrokevganvi2016-170405115750/75/Mechanical-thrombectomy-with-stent-retriever-33-2048.jpg)