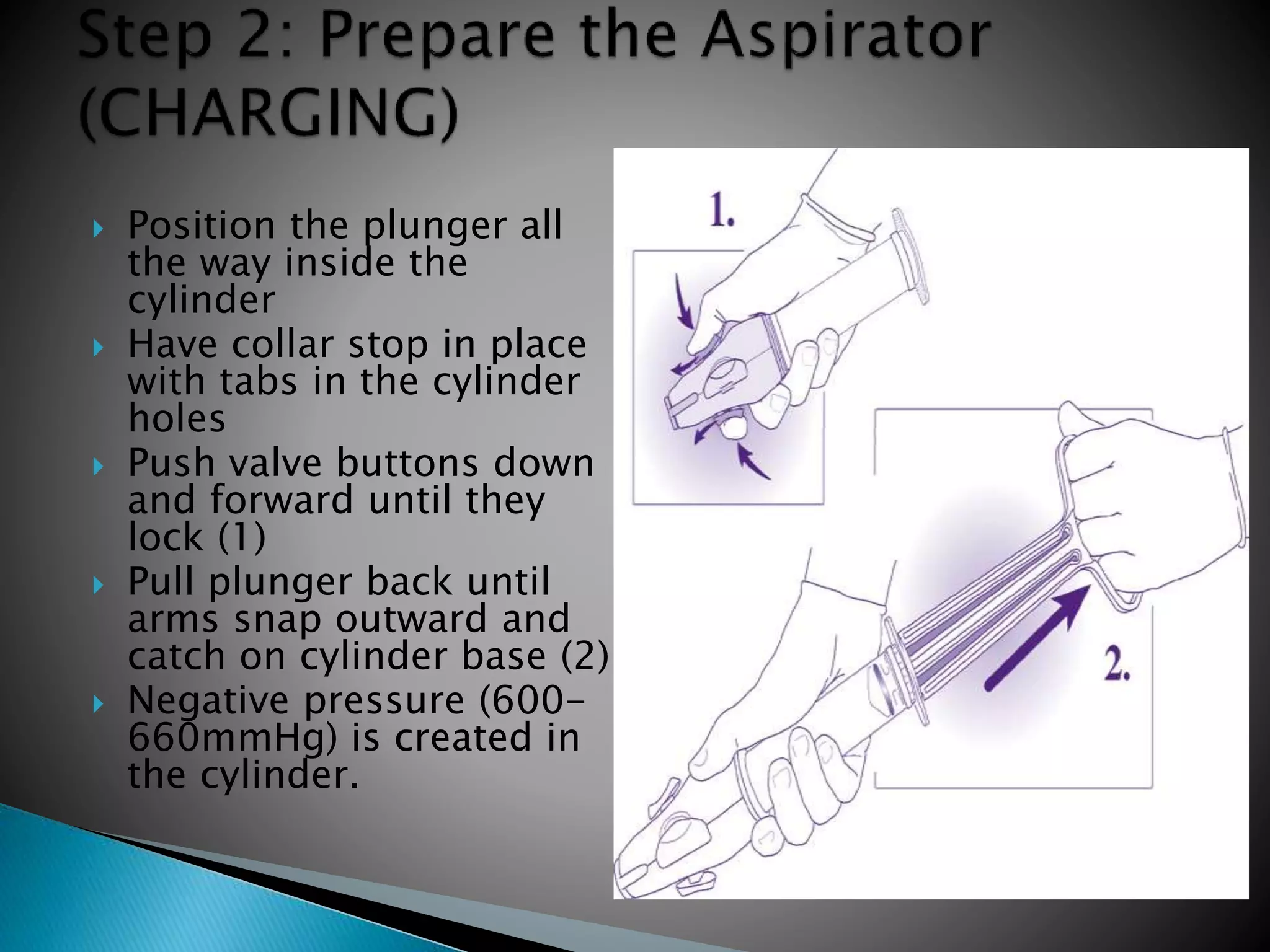
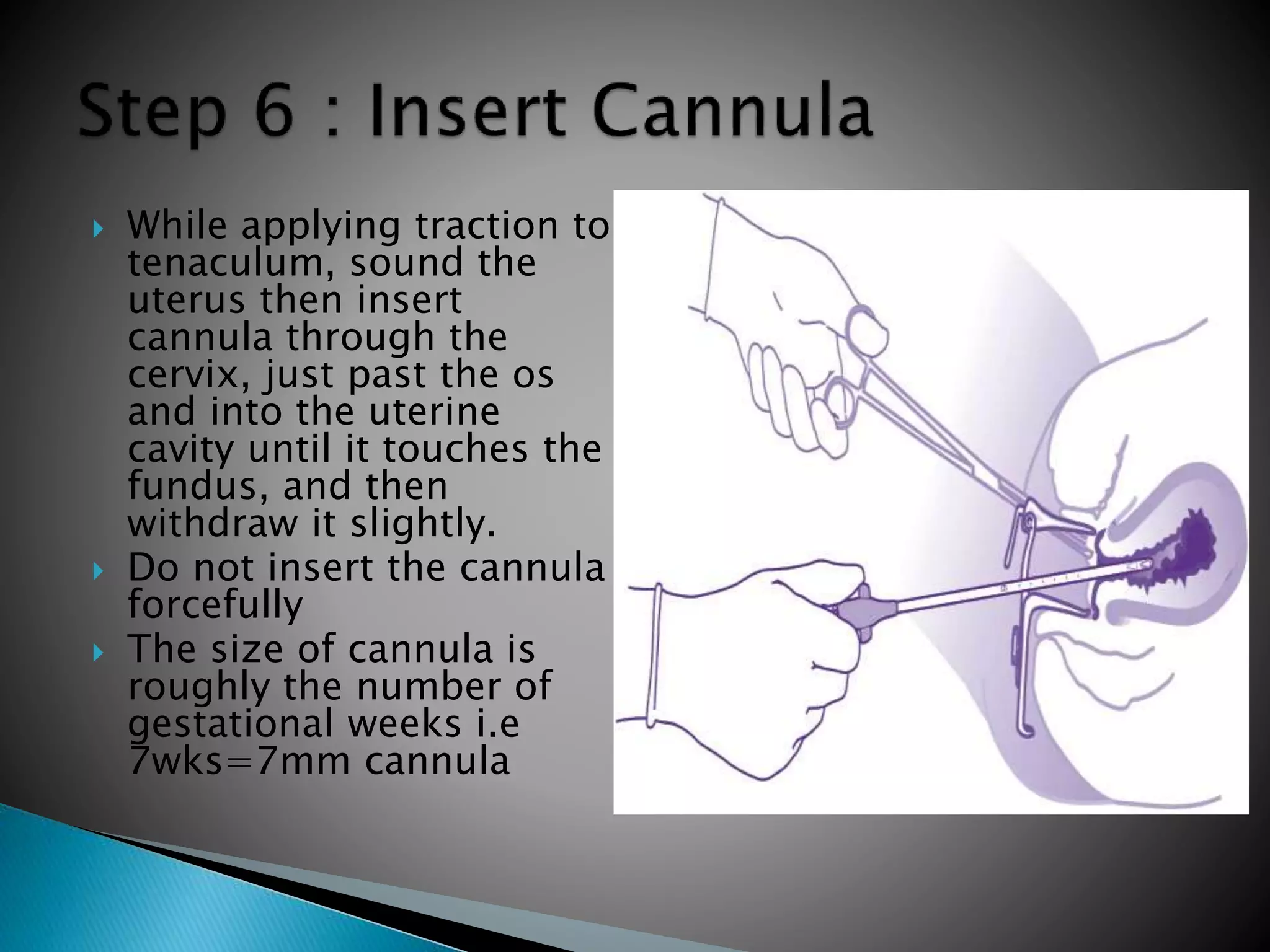
This document presents a case of a 29-year-old woman who is 3 months pregnant and experiencing bleeding and abdominal pain. On examination, she is found to have an incomplete miscarriage. The document then discusses manual vacuum aspiration (MVA) as a procedure to evacuate the uterine contents in cases of incomplete miscarriage. It covers the advantages, indications, contraindications, equipment, precautions, procedure steps, and potential complications of MVA. MVA is described as a safe, affordable option for uterine evacuation that is easy to learn and use without requiring electricity.