This document provides an introduction to principles of anti-microbial therapy. It discusses key topics including:
- Sir Alexander Fleming's discovery of penicillin in 1928.
- The definition of chemotherapy and agents used to treat infections and cancer.
- Factors considered in selecting appropriate anti-microbial agents, including the infecting organism, site of infection, and patient factors.
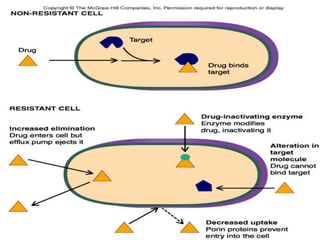
- Mechanisms of anti-microbial resistance that can develop, including genetic alterations in microbes and changes in target sites or drug accumulation.
- Complications of anti-microbial therapy like hypersensitivity, direct toxicity, and superinfections.