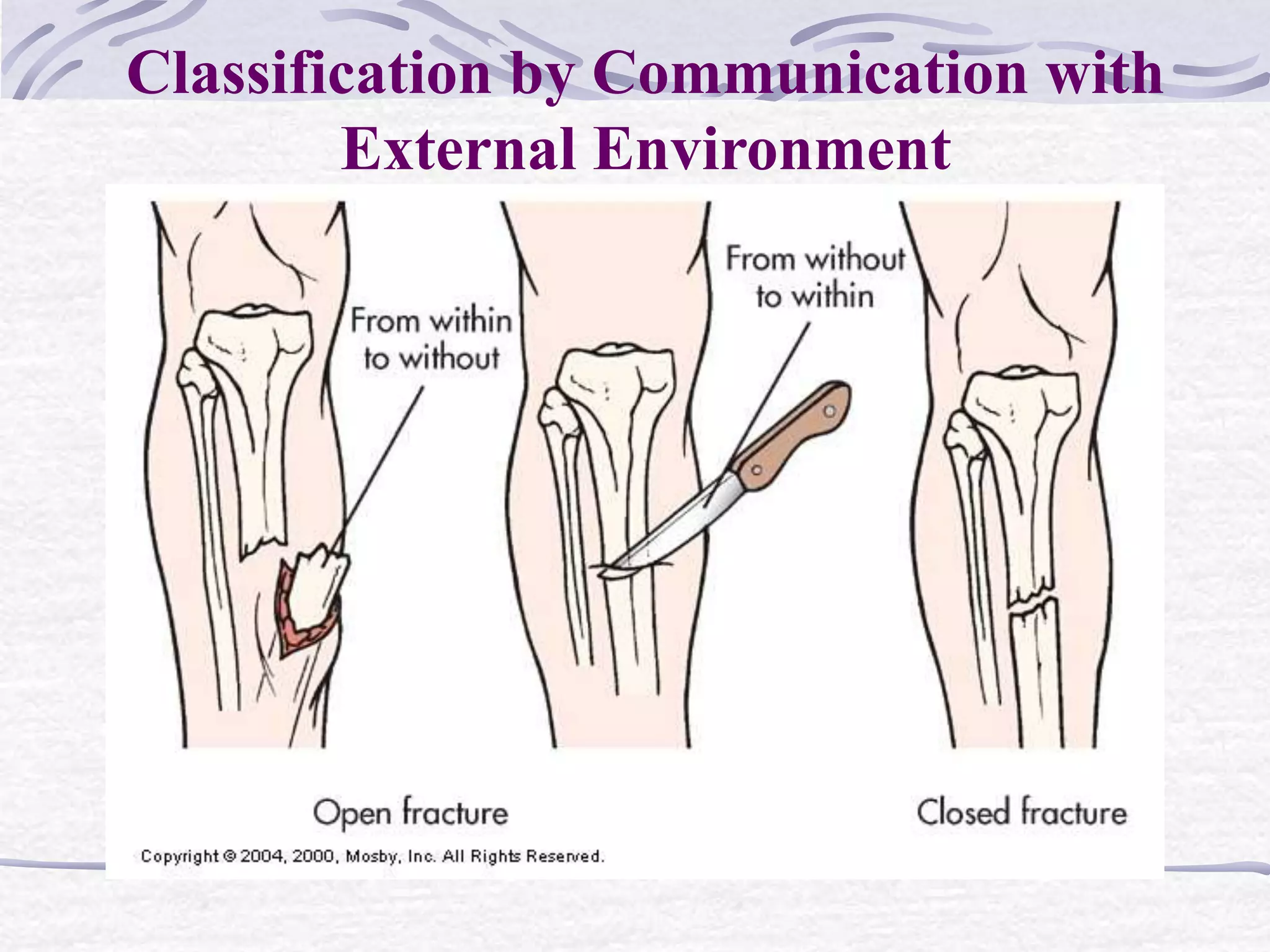
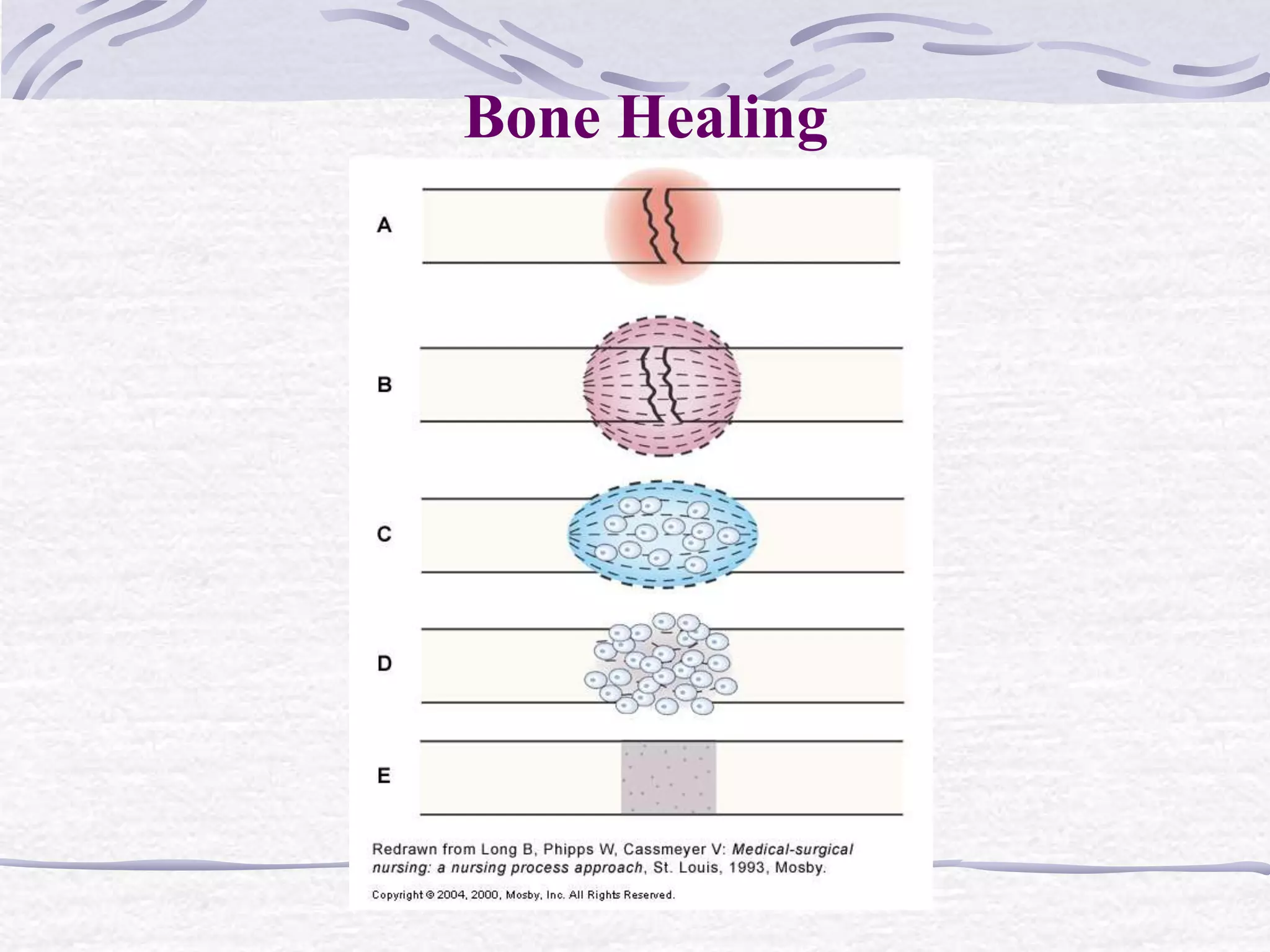
Fractures are breaks in the continuity of bone that are usually caused by trauma. They are described and classified based on their type, communication with the external environment, and anatomic location. The goals of treatment are to realign bone fragments through reduction, immobilize using casts, plates or traction to maintain alignment during healing, and restore normal function. Complications can include infection, compartment syndrome which decreases blood flow, venous thrombosis, fat embolism syndrome, and issues with healing like malunion, non-union or osteomyelitis.