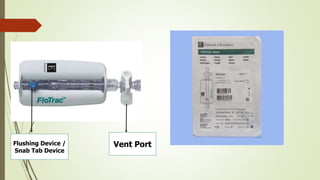
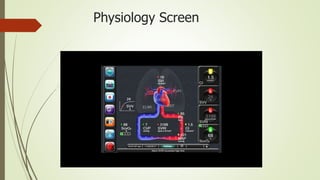
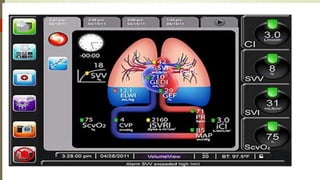
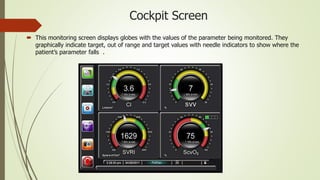
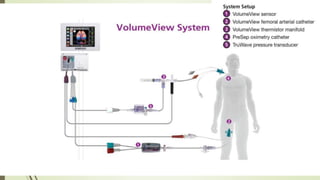
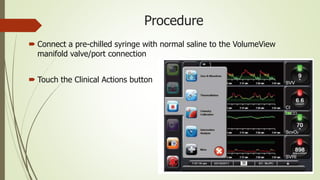
Flotrac is a hemodynamic monitoring platform that continuously measures cardiac output and stroke volume using a patient's arterial pressure waveform, with parameters updated every 20 seconds. It is primarily used for critical care patients requiring assessments of cardiac function, fluid status, and vascular resistance, with both continuous and intermittent measurement options. This minimally invasive system provides dynamic insights into a patient's hemodynamics while requiring no manual calibration and is designed for mechanically ventilated patients.