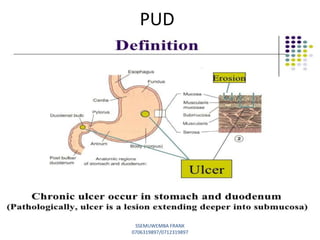
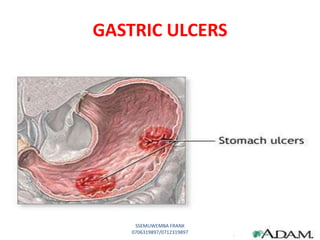
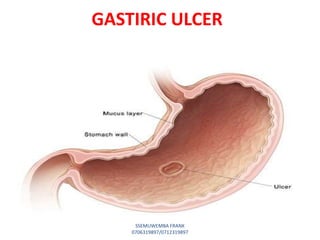
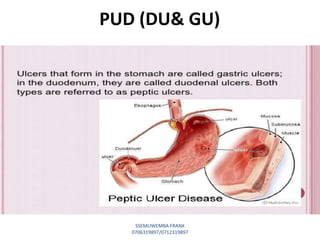
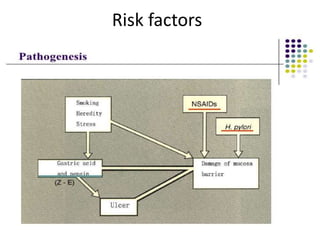
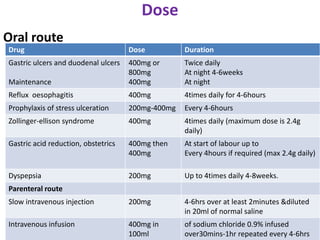
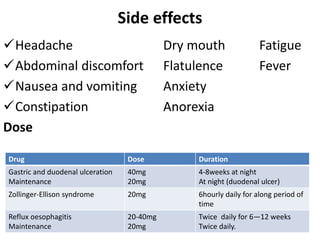
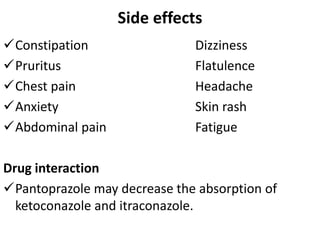
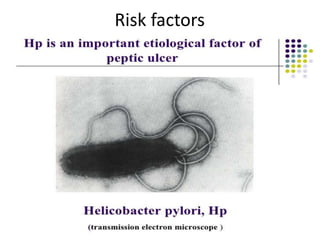
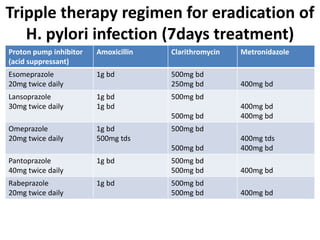
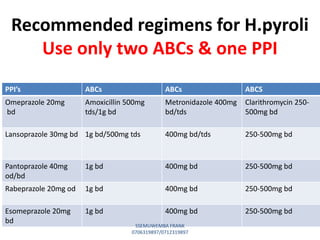
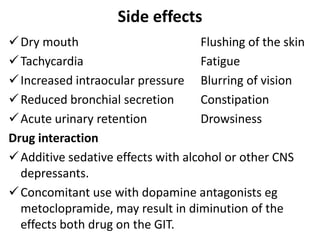
This document discusses drugs used to treat peptic ulcer diseases. It outlines 5 main classes of drugs: anti-acids, H2 receptor antagonists, proton pump inhibitors, antispasmodics, and antibiotics. For each drug class, it provides examples of common drugs and discusses their indications, mechanisms of action, dosages, side effects, and drug interactions. The document focuses in depth on several proton pump inhibitors (omeprazole, esomeprazole, lansoprazole) and H2 receptor antagonists (cimetidine, famotidine, ranitidine), outlining their pharmacokinetics, indications, contraindications, dosages, and key considerations for use.