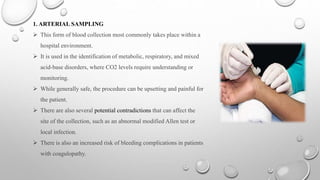
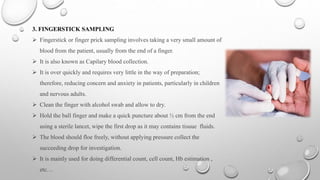
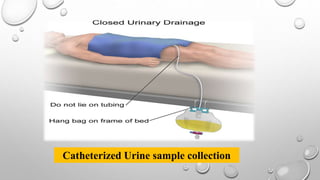
Clinical pathology is the laboratory analysis of bodily fluids and tissues to diagnose disease. It involves collecting samples such as blood, urine, and tissues and analyzing them via techniques including virology, bacteriology, clinical chemistry, serology, and histology. Blood can be collected via arterial sampling, venipuncture, or fingerstick while urine is usually collected via clean-catch, catheterization, or suprapubic aspiration. Samples must be properly labeled and either immediately transported or preserved/refrigerated to maintain integrity for laboratory analysis and diagnosis.