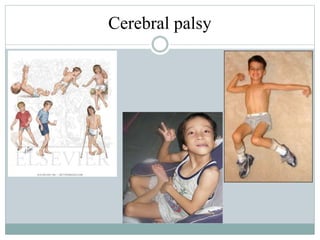
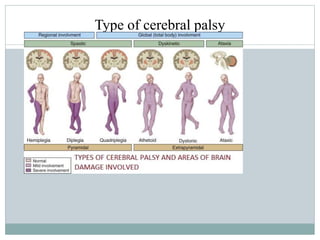
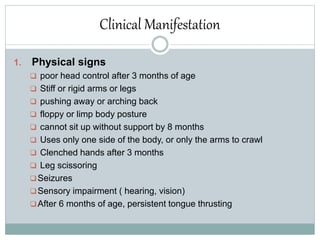
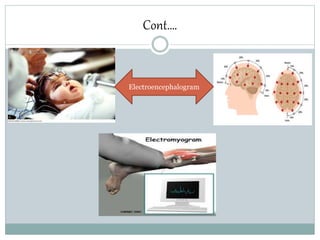
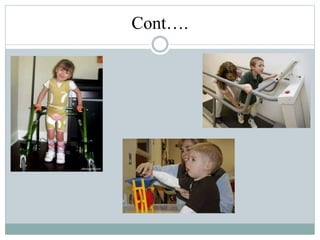
Cerebral palsy (CP) is a group of disorders that affect movement and posture, caused by damage to the developing brain either during pregnancy or shortly after birth. The main types of CP are spastic, dyskinetic, and ataxic. Symptoms vary but may include stiff muscles, poor coordination, weak muscles, and issues with speech and vision. Diagnosis involves neurological and imaging exams. Treatment focuses on physical, occupational, and speech therapy as well as medications or surgery to manage symptoms. Nursing care involves monitoring the child, assisting with therapies, educating families, and addressing issues like mobility, nutrition, and sensory problems.