Cellular adaptations include reversible changes in cells' size, number, phenotype, or functions in response to environmental changes. Physiologic adaptations represent responses to normal stimulation, while pathologic adaptations allow cells to avoid injury but compromise normal function. Common cellular adaptations include:
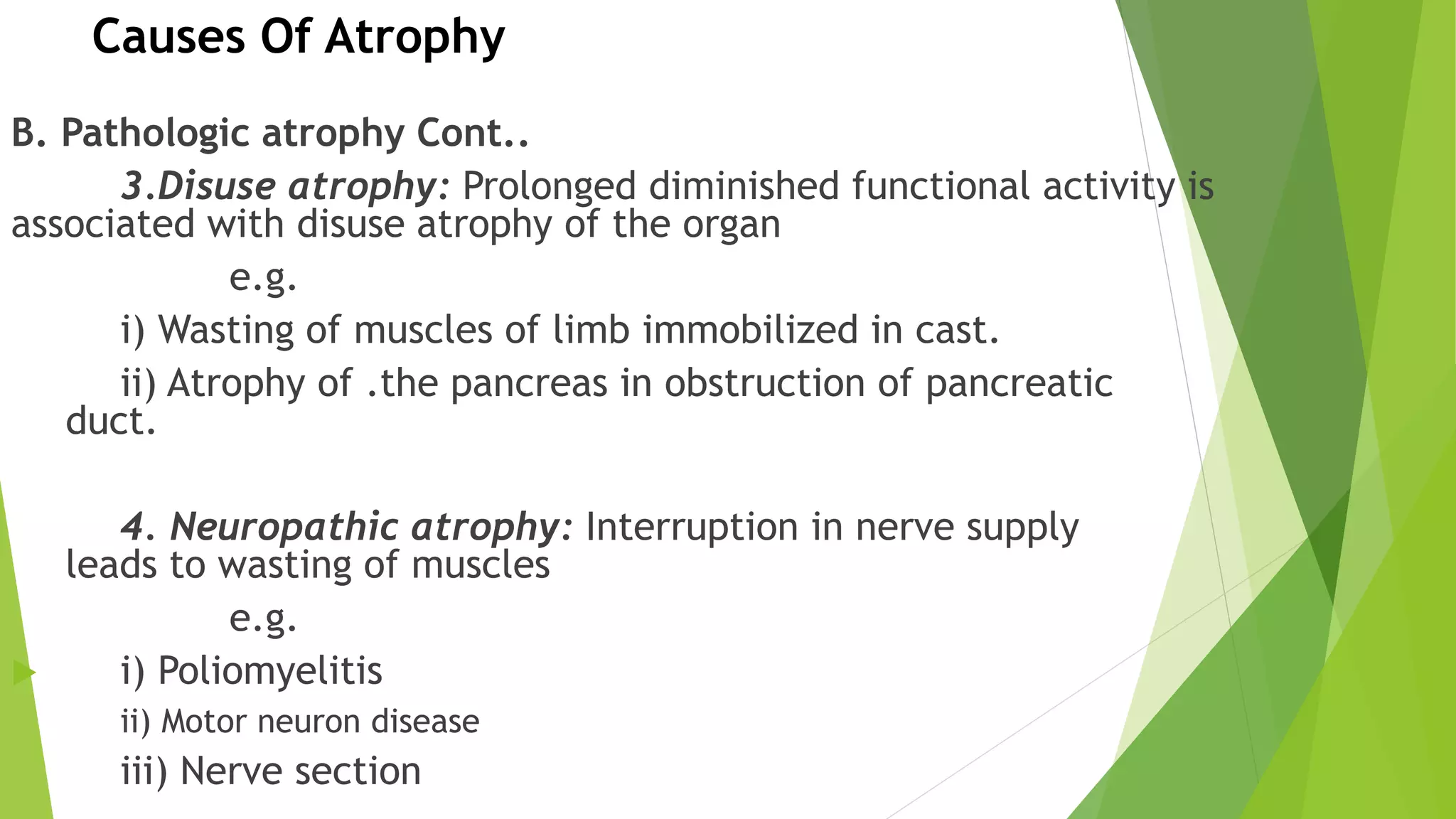
- Atrophy, a shrinkage in cell size from loss of substance.
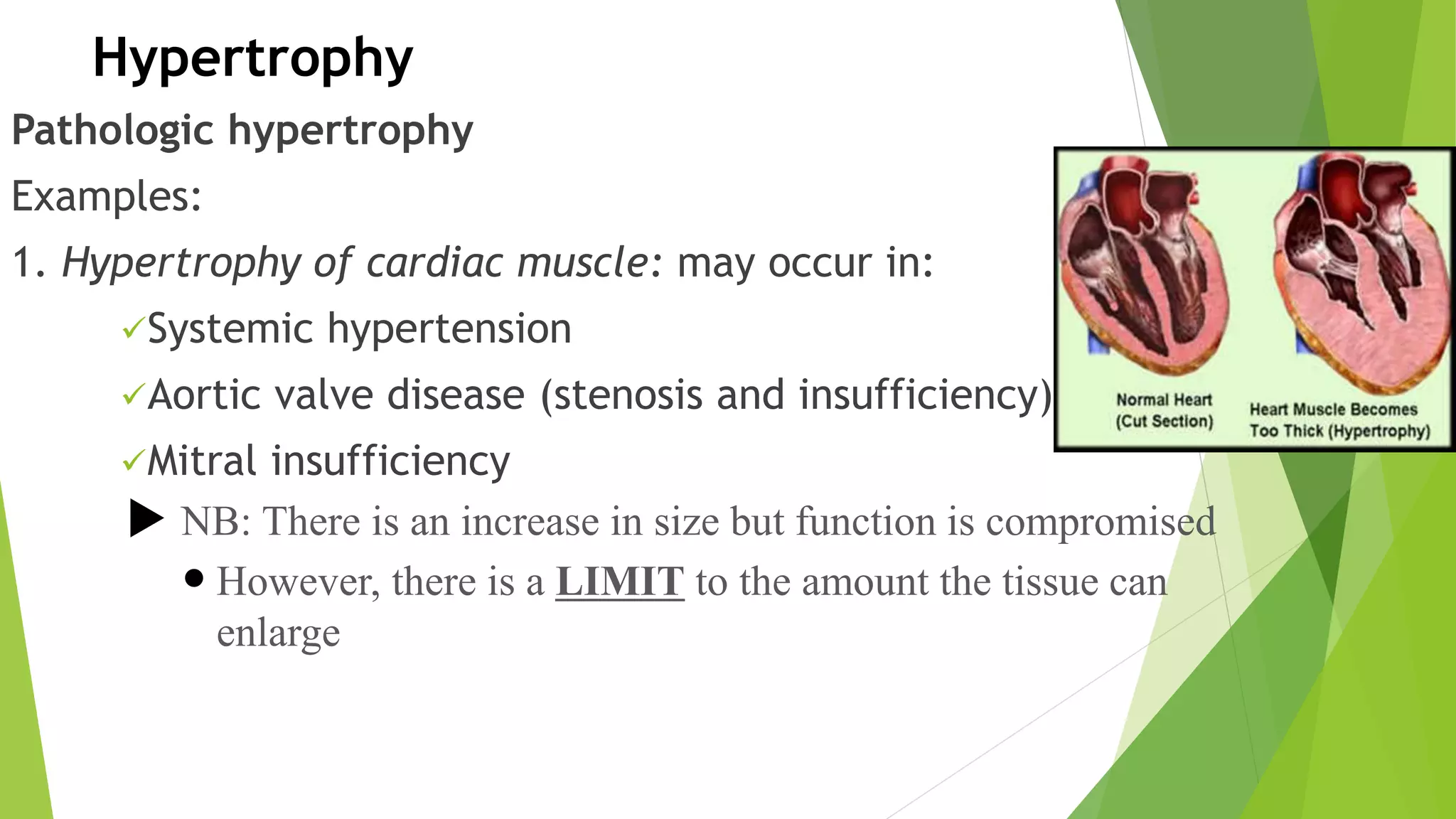
- Hypertrophy, an increase in cell size from increased organelles and proteins.
- Hyperplasia, an increase in cell number through cell division.
- Metaplasia, replacement of one adult cell type with another better suited to stresses.
- Dysplasia, disordered cell development with proliferation and cytologic changes that can progress to carcinoma