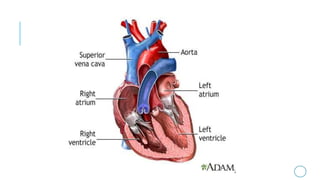
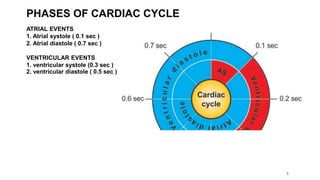
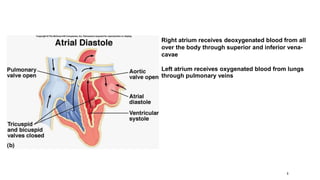
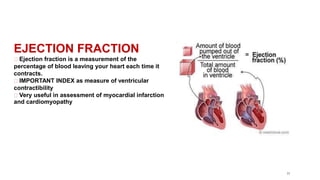
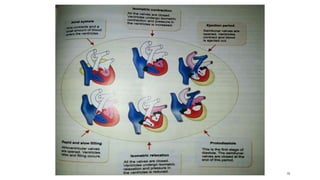
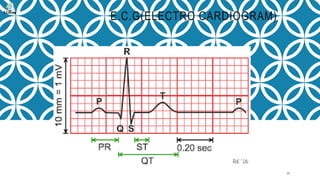
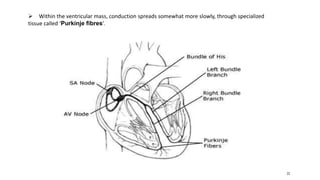
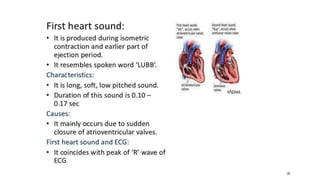
This document outlines the cardiac cycle, ECG, and heart sounds, detailing their phases and physiological significance. It describes the sequence of heart events, including atrial and ventricular systole and diastole, as well as the electrical conduction system of the heart. Additionally, it covers the importance of ECG in diagnosing cardiac conditions and includes key questions related to the topics discussed.