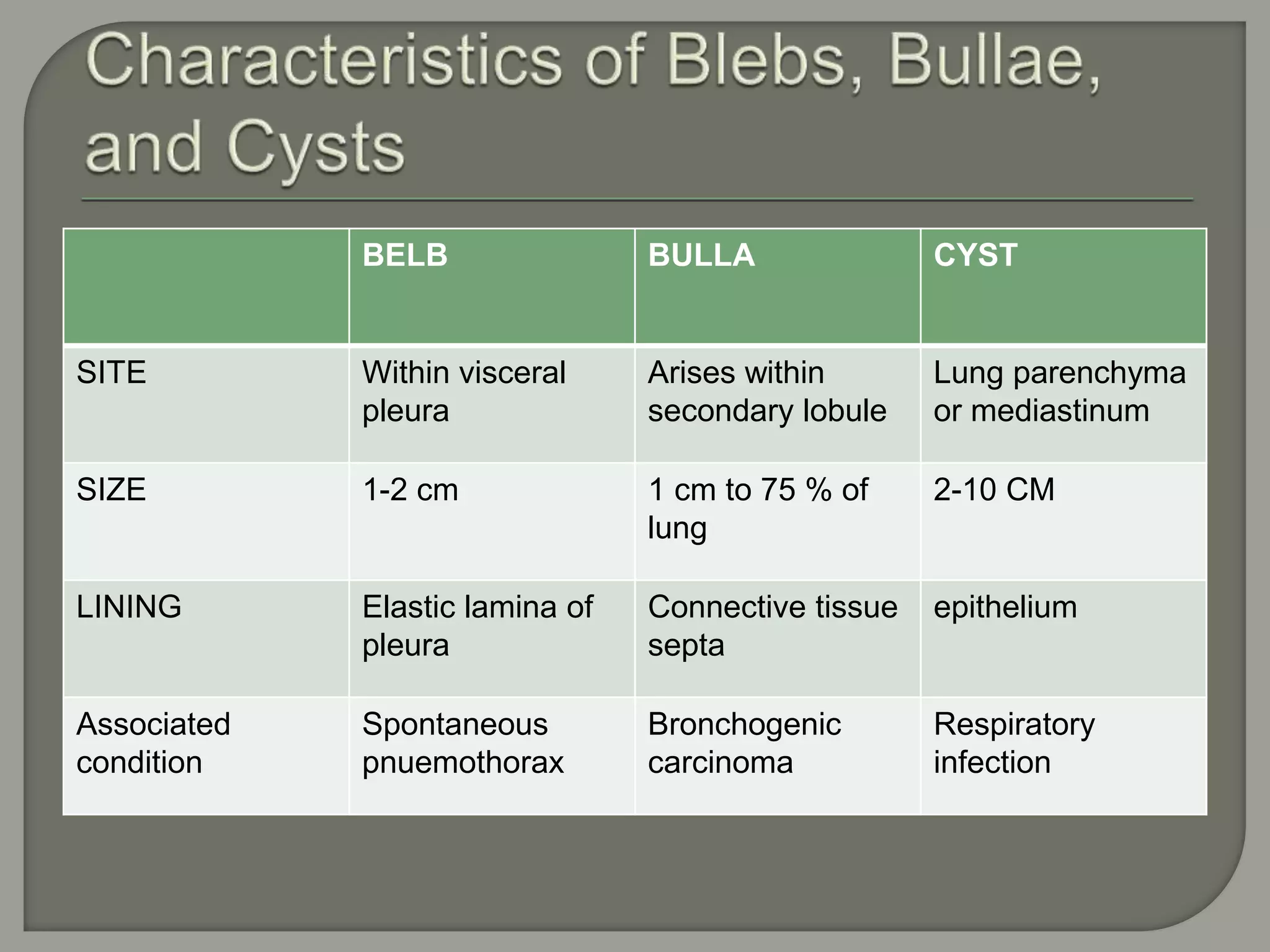
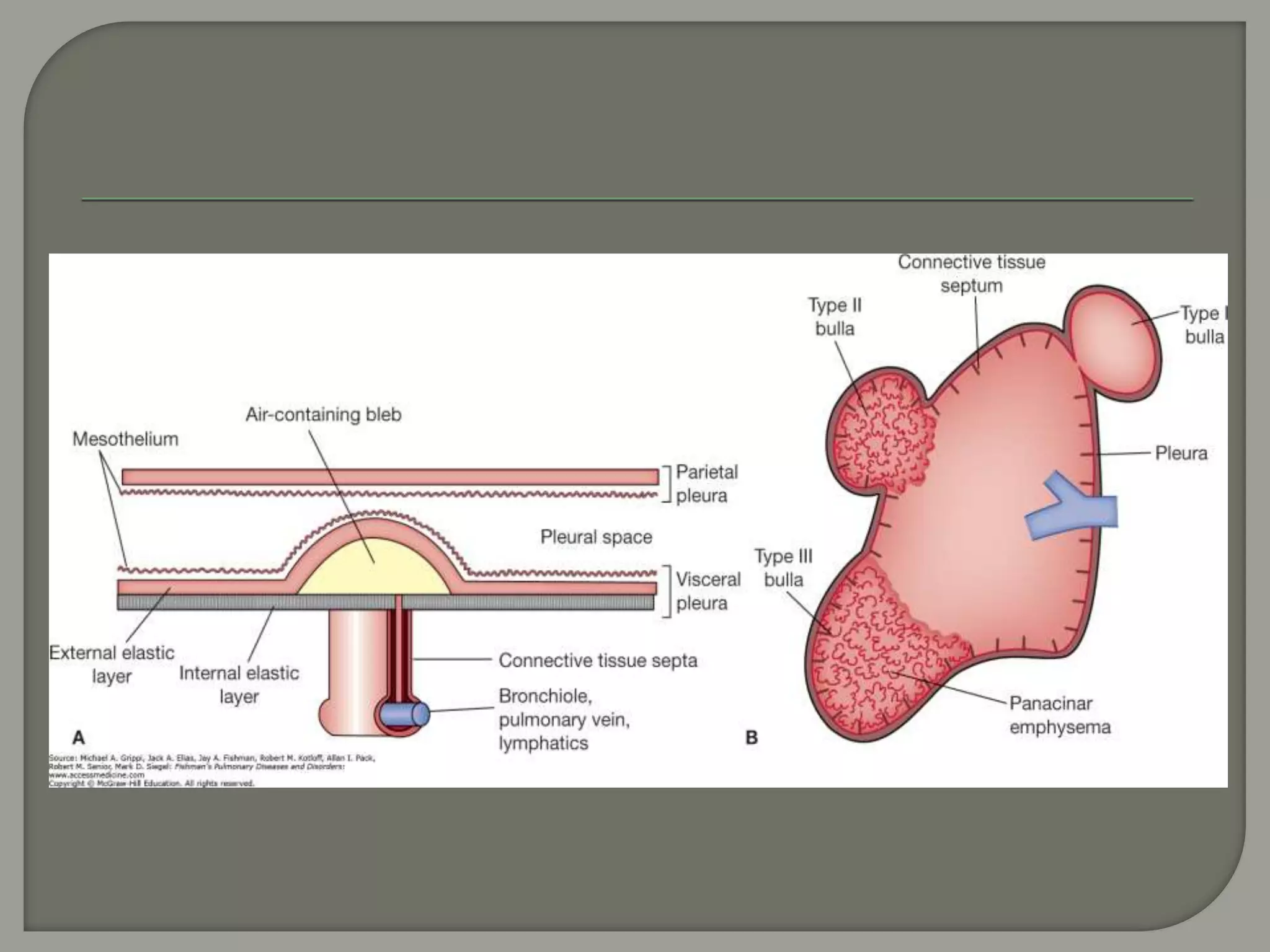
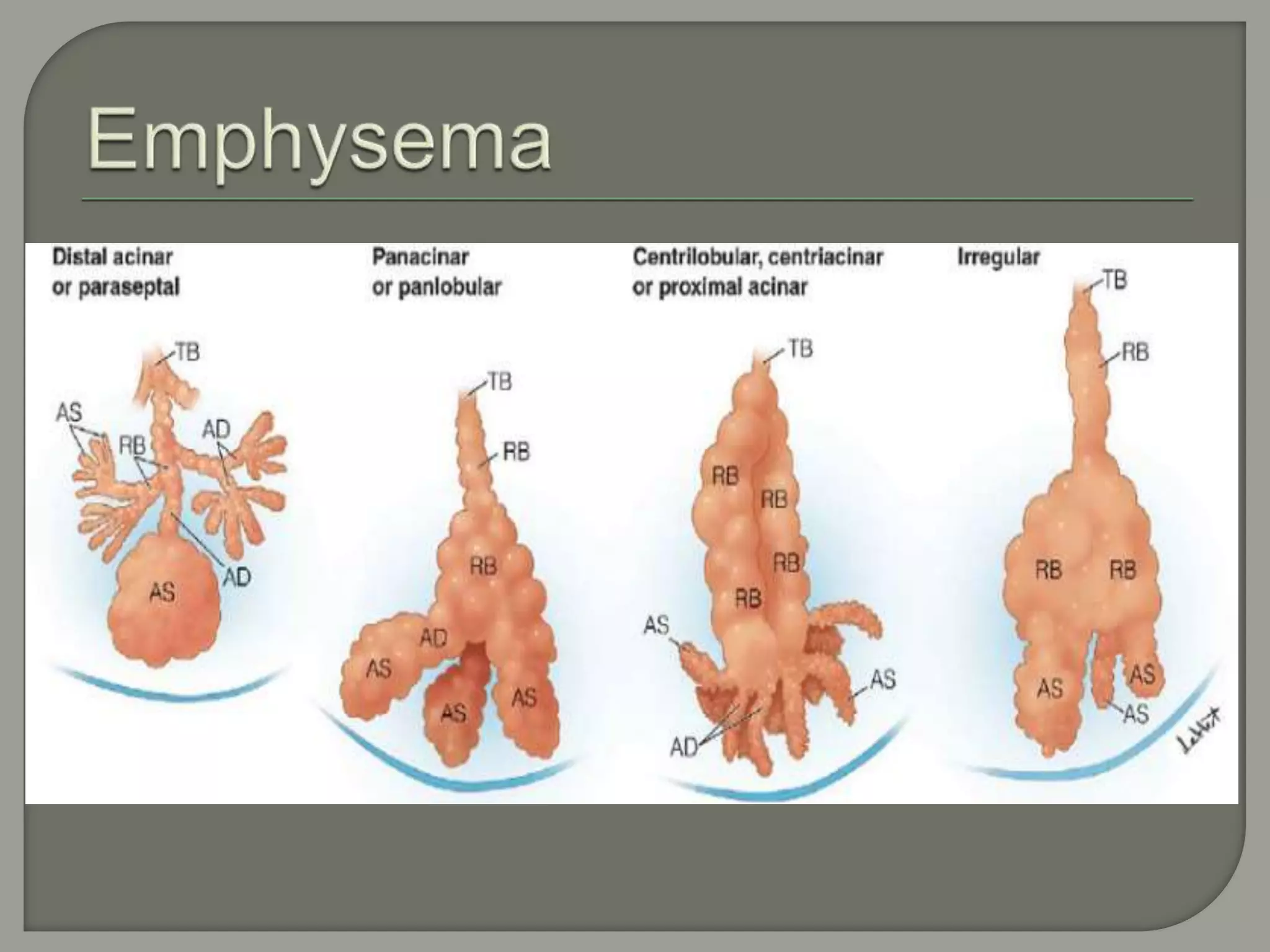
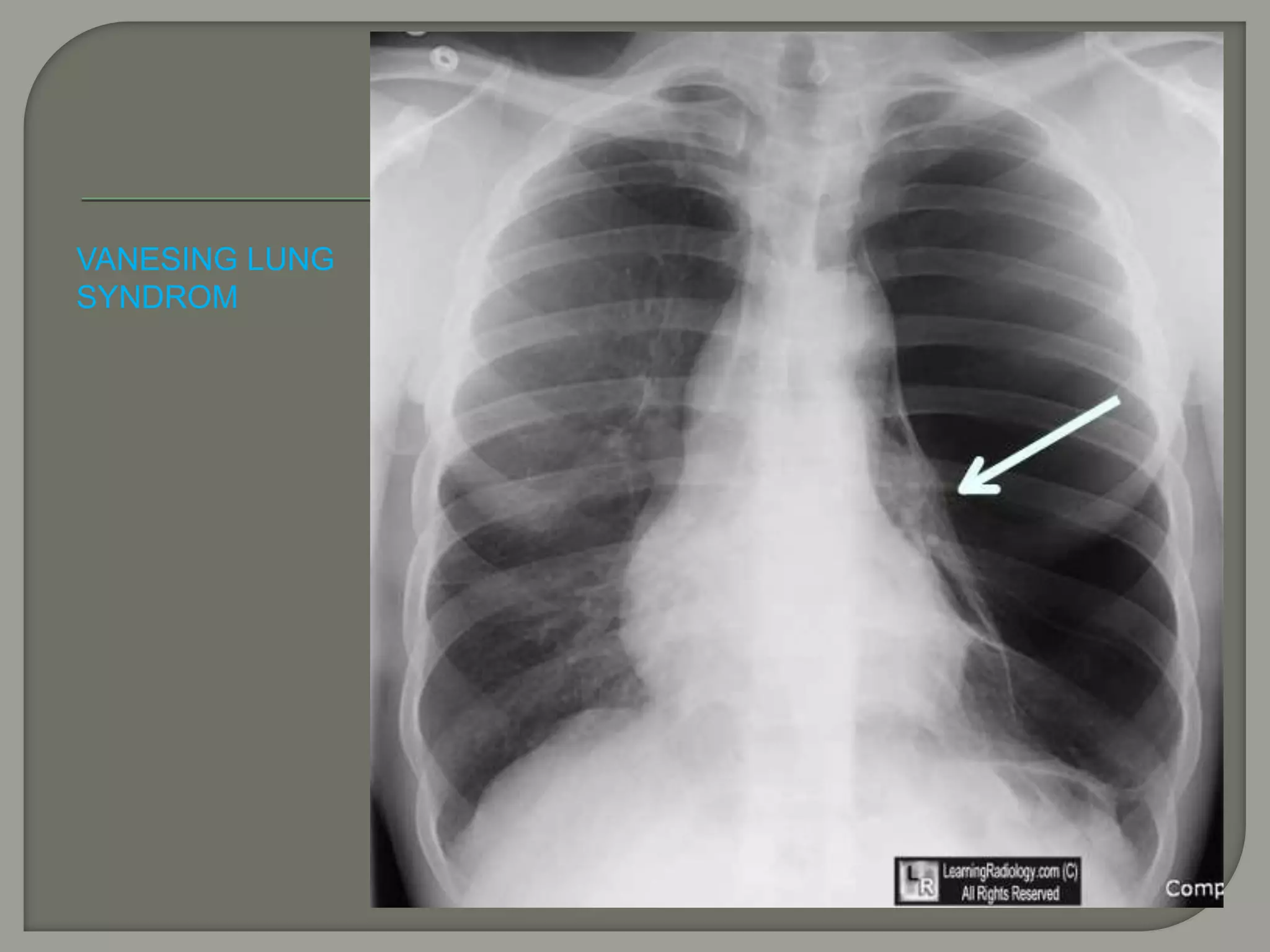
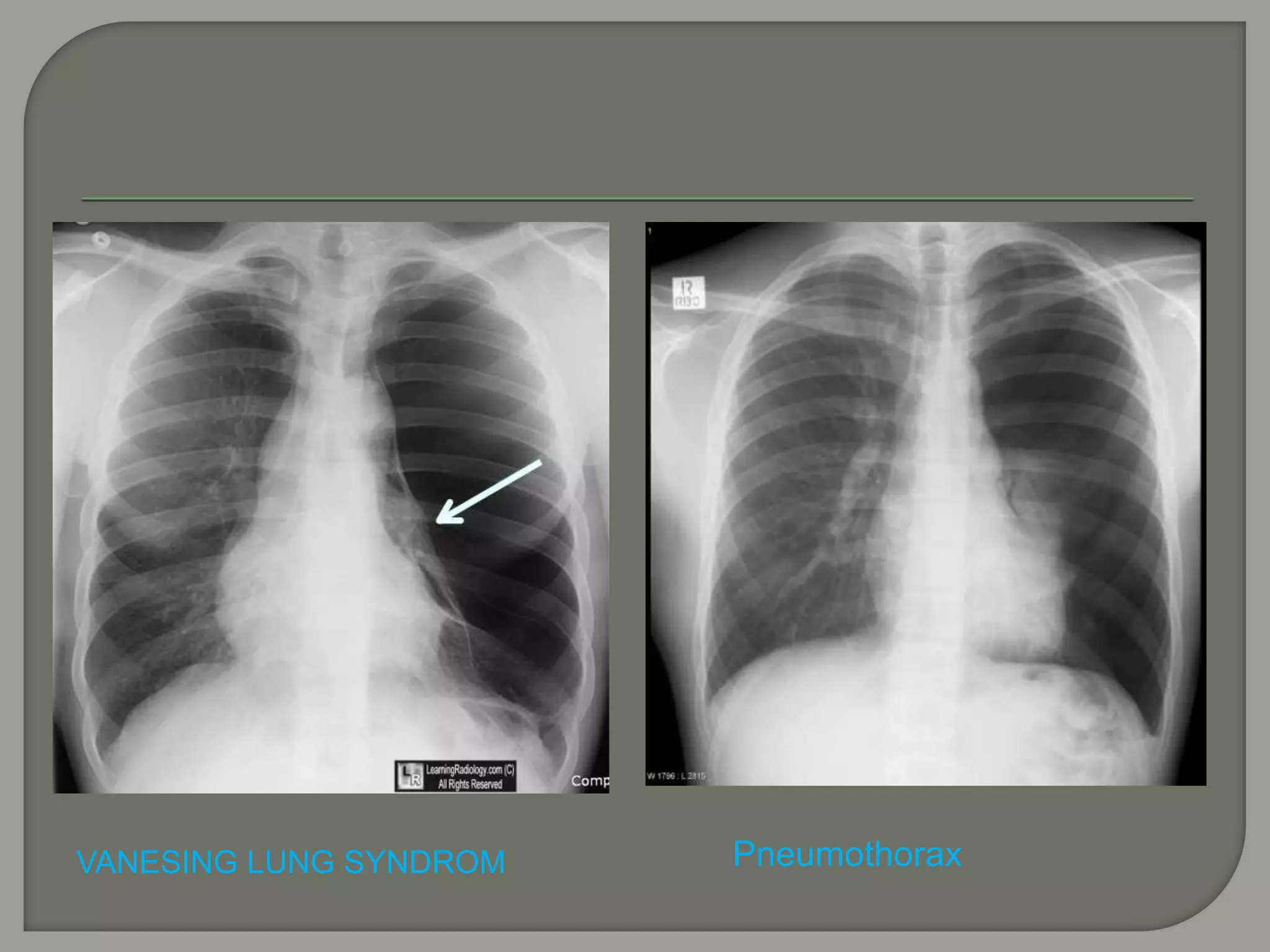
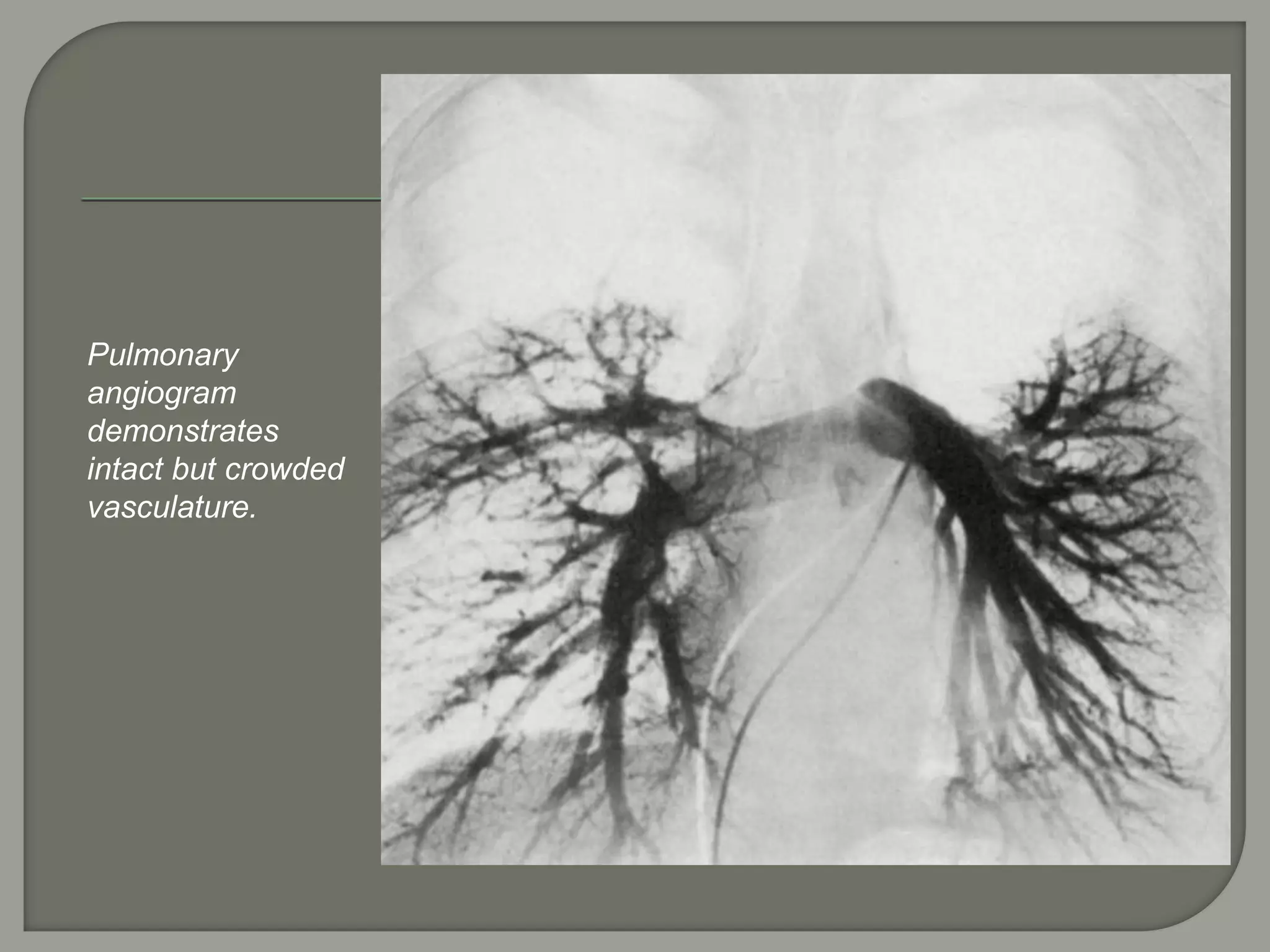
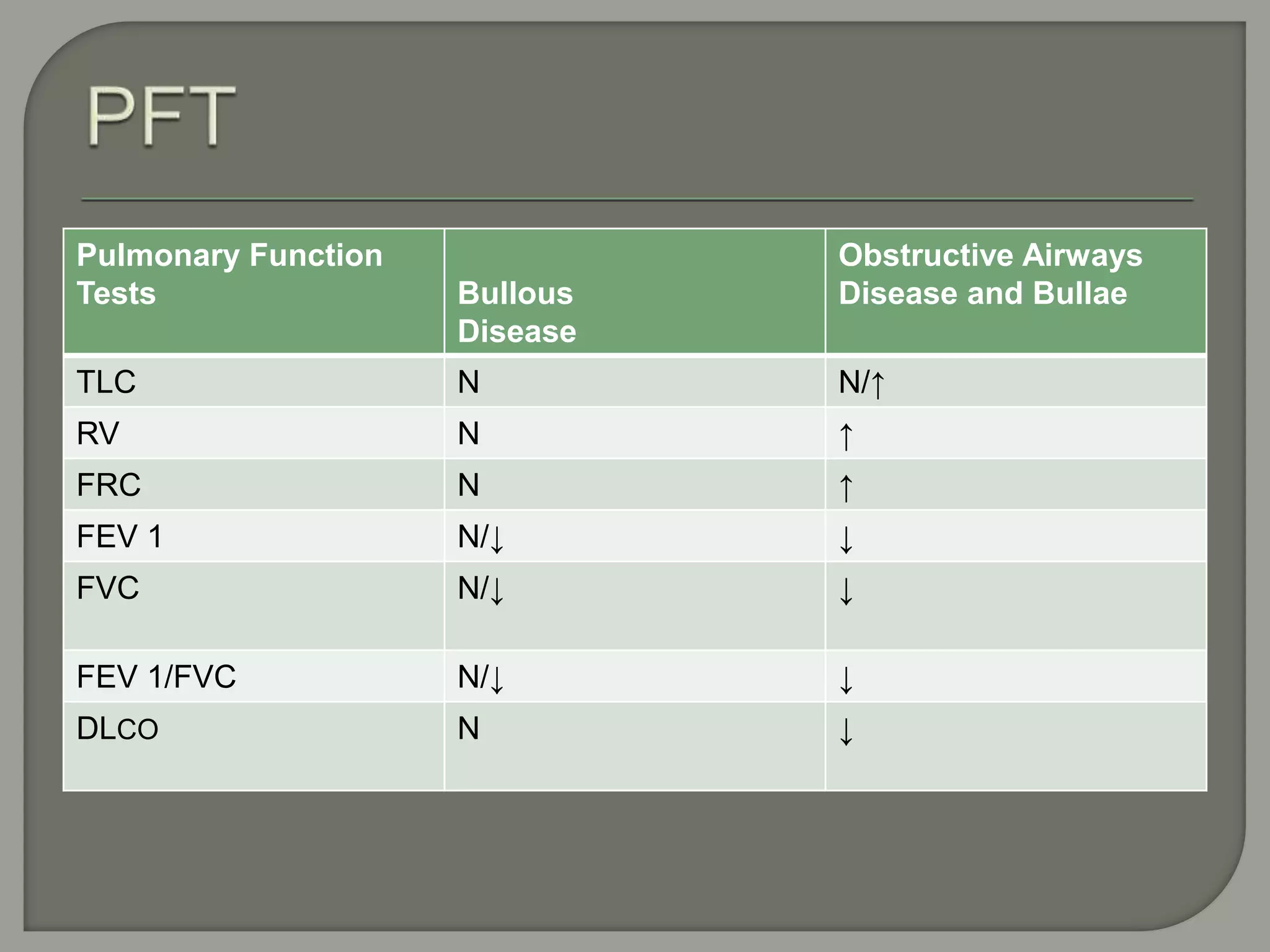
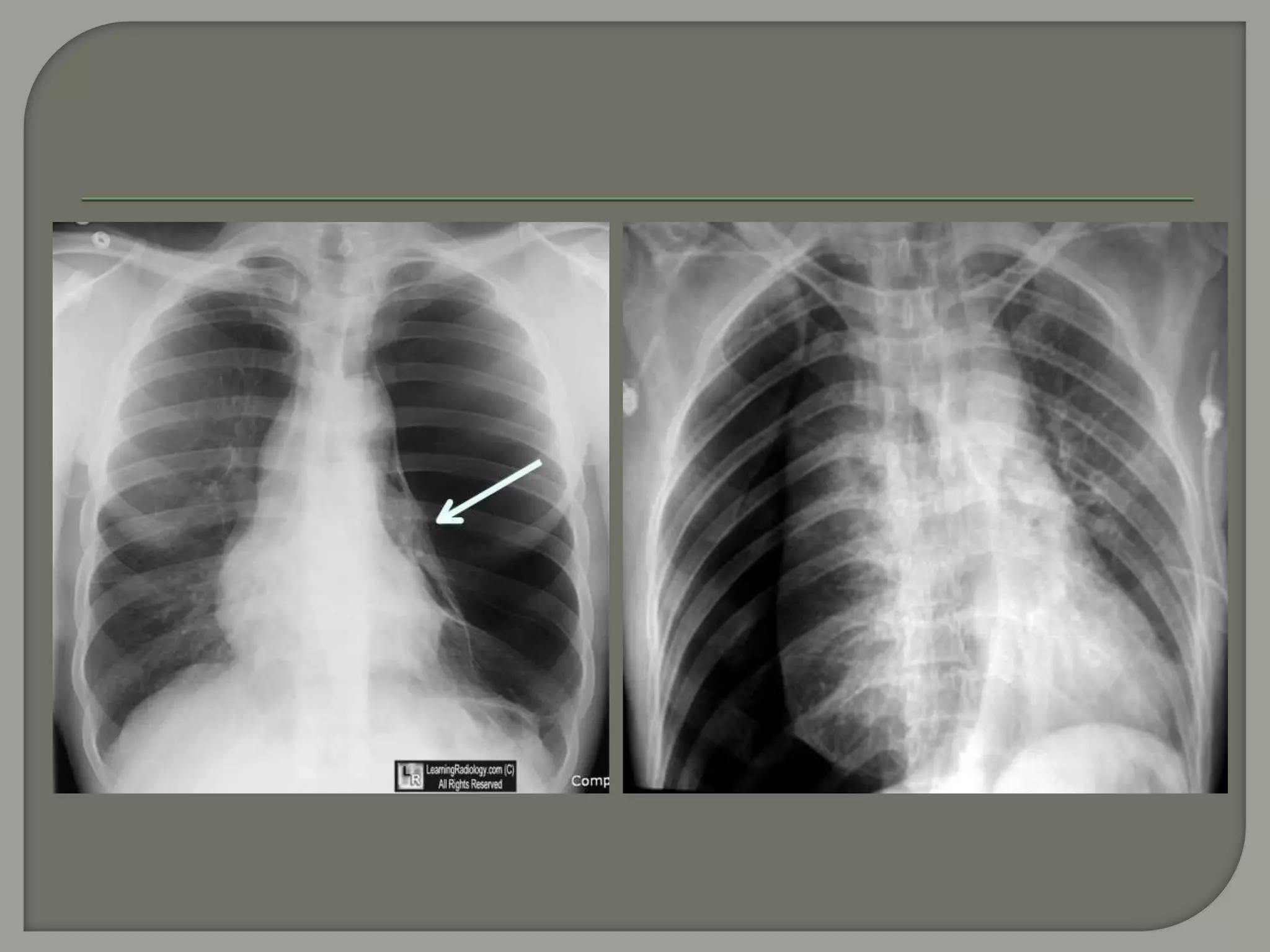
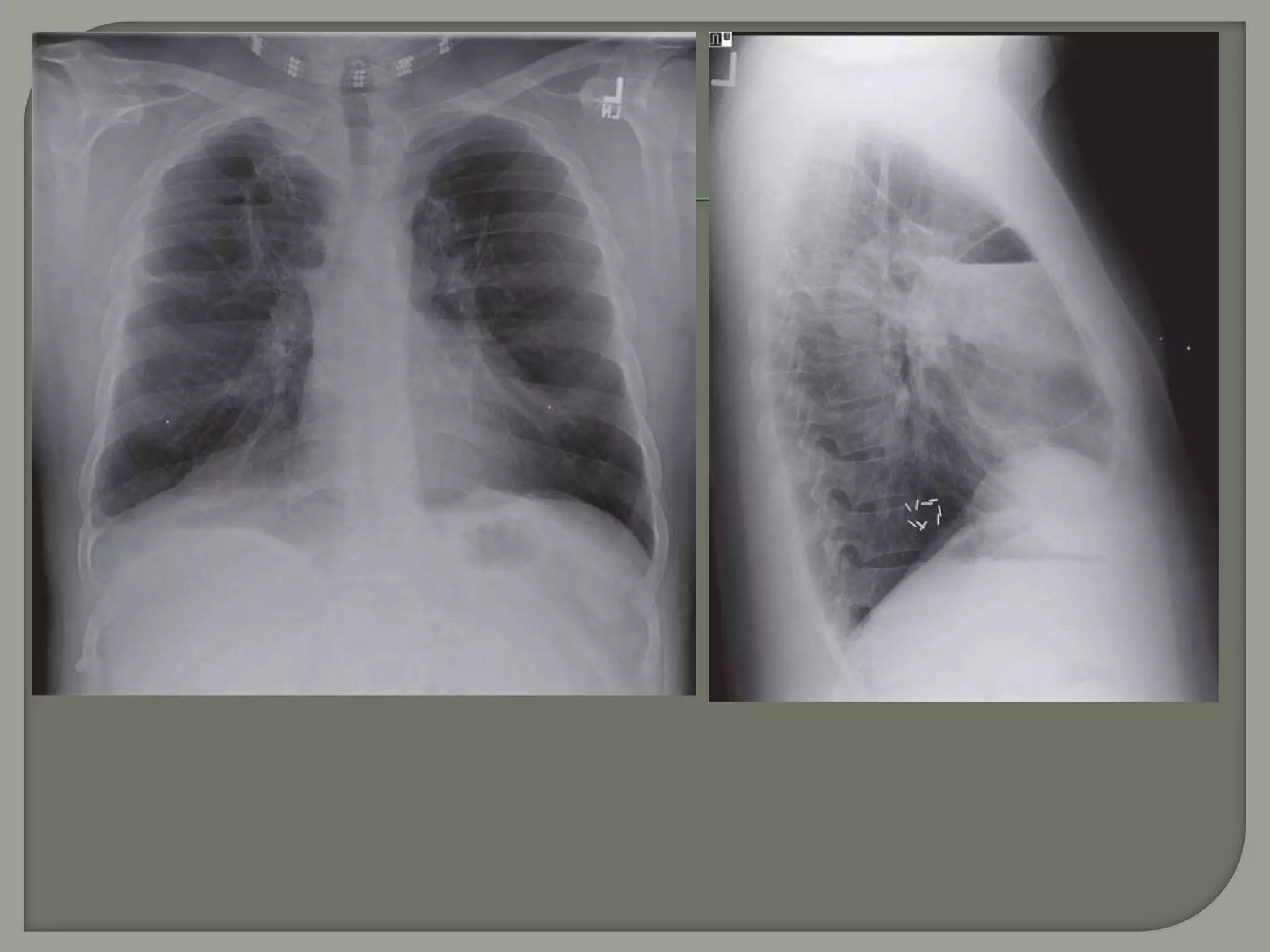
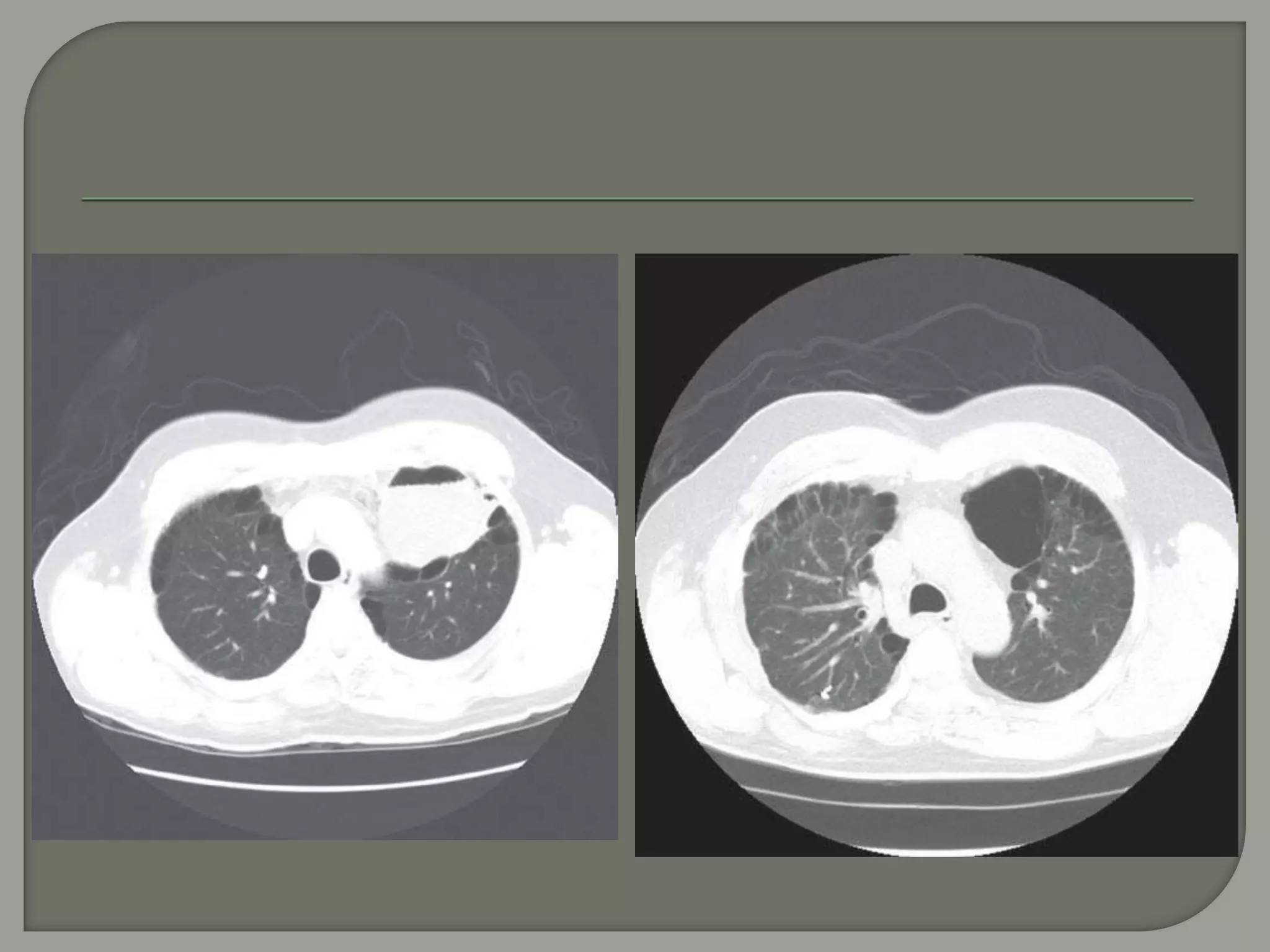
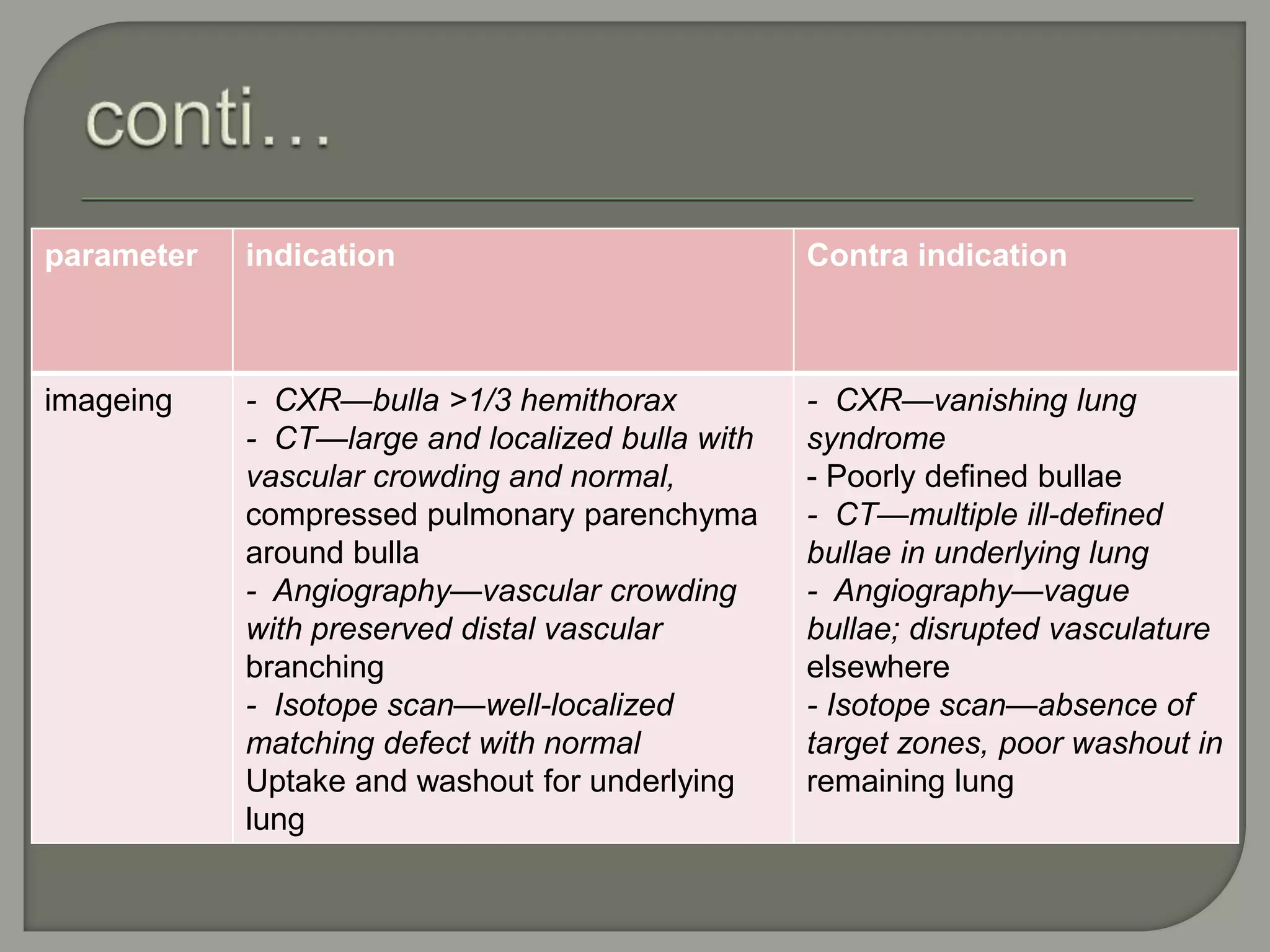
The document discusses the characteristics and clinical contexts of bullae in the lungs, including their formation, types, and associated conditions such as emphysema and pulmonary fibrosis. It outlines diagnostic methods, complications, and treatment options, including bullectomy for severe cases. Management strategies for patients with bullous lung disease, including monitoring and surgical interventions, are also detailed.