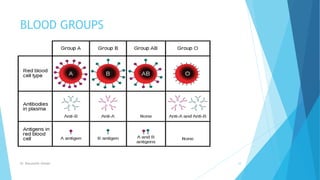
The document offers a comprehensive overview of blood transfusion, including its definition, historical background, blood components, blood group compatibility, donor selection, storage, and potential complications. It outlines the different types of blood transfusions, the importance of compatibility, and various blood products along with their uses. Additionally, it discusses the management of immediate and delayed reactions associated with blood transfusions, emphasizing the need for careful donor selection and handling.