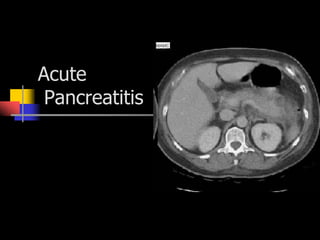
Acute pancreatitis
- 2. Acute Pancreatitis Sudden onset of unrelenting upper abdominal pain resulting from inflammation of the pancreas Patients commonly present to ED due to severe abdominal pain Requires admission to the hospital for medical management, accounting for between 166,000 to 224,000 admissions each year with an estimated annual cost of $3.6 to $6 billion
- 3. Pancreas Complicated exocrine and endocrine gland located in the upper abdominal region Non-capsulated lobular organ about 12 to 20 cm long and lies behind the peritoneum of the posterior abdominal wall Divided into head, body, and tail
- 4. Pancreas Tail Adjacent to hilum of spleen Body Extends horizontally behind stomach Head Nestled in the duodenal sweep Sphincter of Oddi Circular smooth muscle that surrounds both the common bile duct and the main pancreatic duct Ampule of Vater Site where the common bile duct and main pancreatic duct drain into duodenum
- 6. Pancreas The lobes of the pancreas are divided into subunits of acini cells and the Islets of Langerhans Acini cells are involved in the production of 20 different digestive enzymes and include amylase released to digest starch and lipase released to digest fats The most abundant of the enzymes is trypsin, which is released into the duodenum These enzymes are activated by enterokinase, which is produced by the intestinal mucosa
- 7. Pathophysiology Triggering mechanism not exactly understood Pancreatic enzymes that escape into the surrounding tissue due to compromised pancreatic function seem to be the primary cause When the pancreas becomes damaged or the ducts become blocked, the trypsin inhibitor accumulates and activates the pancreatic secretions that escape into the surrounding tissue, resulting in inflammation, thereby causing acute pancreatitis
- 8. Pathophysiology Release of kallikrein and chymotrypsin results in increased capillary membrane permeability, leading to leakage of fluid into the interstitium and development of edema and relative hypovolemia Elastase is the most harmful in terms of direct cell damage, it causes dissolution of the elastic fibers of blood vessels and cuts, leading to hemorrhage Phospholipase A in the presence of bile, destroys phosholipids of cell membranes causing severe pancreatic and adipose tissue necrosis Lipase flows into damaged tissue and is absorbed into systemic circulation, resulting in fat necrosis of the pancreas and surrounding tissues
- 9. Acute Pancreatitis Inflammation of the pancreas that produces exocrine and endocrine dysfunction Results from premature activation of pancreatic exocrine enzymes (trypsin, phospholipase A, and elastase)
- 10. Edematous (Interstitial) Pancreatitis Usually mild Resolves in about 7 days Results in fluid accumulation and swelling
- 11. Severe or Necrotizing Pancreatitis Associated with a high degree of complications and mortality Caused by the release of cytokines and other proinflammatory mediators that produce a hyperinflammatory reaction, resulting in cell death and tissue damage
- 12. Causes of Acute Pancreatitis Ethanol abuse Biliary diseases Gallstones Choledocholithiasis Biliary sludge Microlithiasis Mechanical/structural injury Sphincter of Oddi dysfunction Pancreas divisum Trauma Postendoscopic retrograde cholangiopancreatography Pancreatic malignancy PUD IBD Medications Azathiprine/6-mercaptopurine Dideoxyinosine Pentamidine Sulfonamides Thiazide diuretics ACEI Metabolic Hypertriglyceridemia Hypercalcemia Infectious Viral Bacterial Parasitic Vascular Vasculitis Genetic predisposition idiopathic
- 13. Acute Pancreatitis: Damage and Destruction Inflammation is caused by premature activation of enzymes which leads to tissue damage If pancreatitis damages the islets of Langerhans, diabetes mellitus may result Severe sudden pancreatitis causes massive hemorrhage and total destruction of the pancreas, manifested as diabetic acidosis, shock and coma
- 14. Clinical Presentation Upper abdominal pain rapidly increasing in severity, often within 60 minutes Epigastric pain Right-sided pain Diffuse abdominal pain with radiation to back Pain rarely only in left upper quadrant Restless Prefer to sit and lean N/V Fever Tachycardia
- 15. Abdominal Examination Decreased or absent bowel sounds Abdominal tenderness Guarding Palpable mass in epigastric area Biliary colic Jaundice if there’s obstruction of the bile duct Cullen’s sign Grey Turner’s Sign
- 16. Clinical Manifestations Abdominal distention Abdominal guarding Abdominal tympany Hypoactive bowel sounds Severe disease: peritoneal signs, ascites, jaundice, palpable abdominal mass, Grey Turner’s sign, Cullen’s sign, and signs of hypovolemic shock
- 17. What testing will reveal…… Serum amylase and lipase levels elevated 3-5 times normal Urine amylase increased for 1-2 weeks Elevated WBC H/H decreased Decreased serum calcium Elevated serum bilirubin, AST, ALT, LD, and alkaline phosphatase Abdominal XRAYS and CT’s showing pleural effusions and bowel dilation and ileus Serum triglycerides >150mg/dl
- 18. Diagnostic Evaluation Patient’s history Physical examination Diagnostic findings Serum amylase levels greater than three times the upper limit Serum amylase levels may be normal in patients with pancreatitis related to alcohol abuse or hypertriglyceridemia Levels greater than five times the top normal value should be expected in patients with renal failure because amylase is cleared by the kidneys
- 19. Diagnostic Evaluation Serum lipase is more sensitive and specific to the pancreas An elevation of greater than three times the top normal value usually confirms acute pancreatitis A lipase-to-amylase ratio of greater than 2 is usually evident with pancreatitis related to alcohol abuse A rise in urine amylase and lipase can be expected and are indicative of pancreatic damage Leukocytosis Hemoconcentration due to third space fluid loss Pancreatitis due to gallstones: elevated AST, ALT, and lactate dehydrogenase
- 20. Imaging Modalities Plain abdominal x-rays for visualizing gallstones or a gas-filled transverse colon ending at the area of pancreatic inflammation colon cut-off sign Abdominal ultrasound Cholelithiasis, biliary sludge, bile duct dilation, and pseudocysts CT of abdomen MRCP (magnetic resonance cholangiopancreatography)
- 21. Ranson’s Criteria The severity of acute pancreatitis is determined by the existence of certain criteria, called Ranson’s criteria The more criteria met by the patient, the more severe the episode of pancreatitis 1% mortality: fewer than three 16%: three or four criteria 40% with five or six criteria 100%: seven or eight criteria
- 22. Ranson’s Criteria On admission Patient older than 55 WBC > 16,000 Serum glucose >200 Serum lactate dehydrogenase >350 Aspartate aminotransferase > 250 During initial 48 hours after admission 10% decrease in Hct BUN increase > 5 Serum calcium < 8 Base deficit > 4 PaO2 < 60 Estimated fluid sequestration > 6 liters
- 23. Common Complications of Acute Pancreatitis Pulmonary Atelactasis Pleural effusions ARDS Cardiovascular Cardiogenic shock Neurologic Pancreatic encephalopathy Metabolic Metabolic acidosis Hypocalcemia Altered glucose metabolism Hematologic DIC GI bleeding Renal Prerenal failure
- 24. Management Fluid Management Nutritional support Rest gut TPN Pain management Supporting other organ systems
- 25. Treatment IV replacement of fluids, proteins, and electrolytes Fluid volume replacement and blood transfusions Withholding food and fluids to rest the pancreas NG tube suctioning Drugs Peritoneal lavage Surgical drainage Laparotomy to remove obstruction
- 26. Fluid Resuscitation Patients with acute pancreatitis may have fluid shifts of 4 to 12 L into retroperitoneal space and peritoneal cavity due to inflammation In severe acute pancreatitis, blood vessels in and around the pancreas may also become disrupted, resulting in hemorrhage. Replace fluids with colloids, crystalloids, or blood products Monitor for S/S of hemorrhage
- 27. Rest the Pancreas NPO status Avoiding use of GI tract is recommended until the patient no longer reports abdominal pain and the serum amylase has returned to normal Provide nutrition enterally using a jejunal tube to prevent pancreatic enzyme secretion. If parenteral therapy is used, the solution is usually a mixture of hypertonic glucose and amino acids. The use of lipid emulsion is contraindicated during acute phase because it increases pancreatic exocrine secretion.
- 28. Pharmacologic Agents Somatostatin Used to decrease pancreatic secretion in acute pancreatitis Decreases intestinal motility and reduces endocrine/exocrine pancreatic secretion Anticholinergic agents Glucagon Cimetidine calcitonin
- 29. Pharmaceutical Treatment Demerol for pain Morphine causes spasm of Sphincter of Oddi However, use of demerol leads to metabolite accumulation Pneumatic compressions TPN/early enteral feedings
- 30. Goals for Treatment Supportive care Pain control Antiemetics IVF NPO Lessening inflammation and necrosis Endoscopic retrograde cholangiopancretography (ERCP) with stone extraction or stent placement Anticipating and treating complications Preventing recurrence