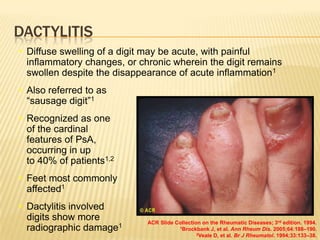
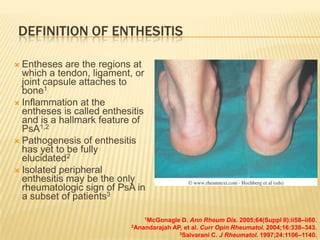
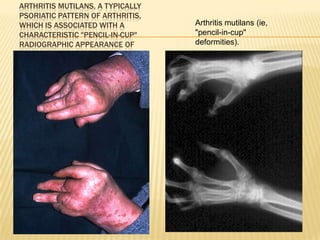
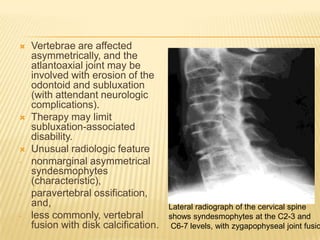
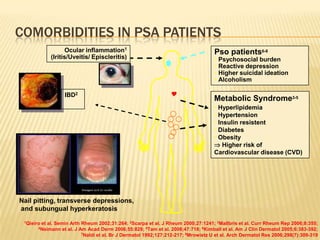
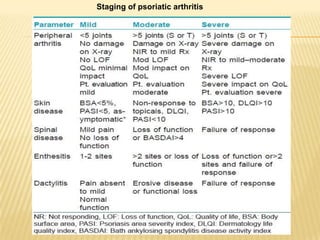
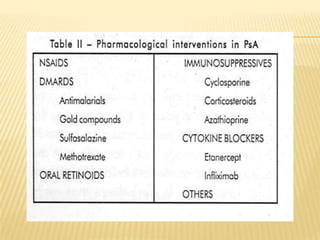
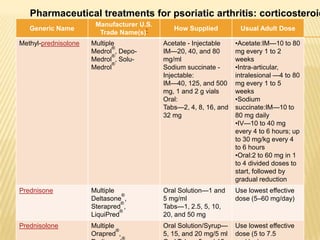
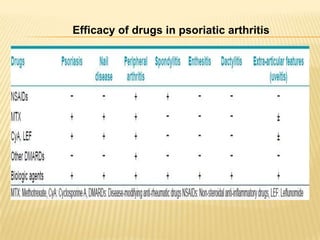
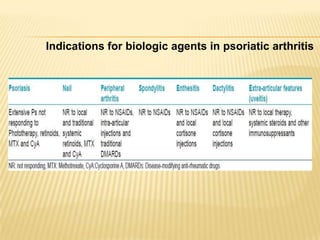
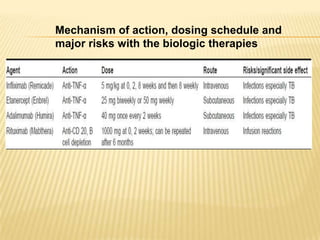
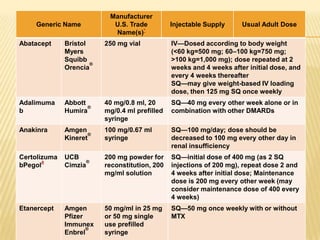
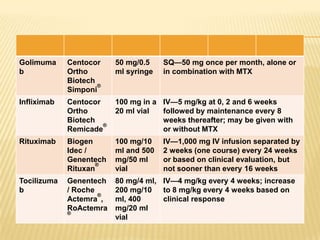
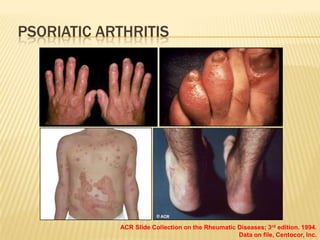
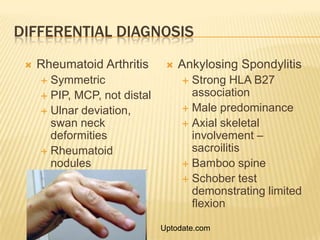
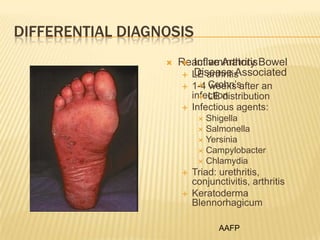
Psoriatic arthritis is a chronic inflammatory disease that affects the joints and skin. It is characterized by osteolysis, bony proliferation, and can cause dactylitis, enthesitis, spondylitis, and various forms of arthritis. While it is classified as a type of spondyloarthritis, it is distinct from rheumatoid arthritis in that it is usually seronegative. The presentation and pattern of joint involvement in psoriatic arthritis can vary between patients and change over time, with the most common forms being asymmetrical oligoarthritis or symmetrical polyarthritis. Diagnosis is based on clinical features and classification criteria such as the CASPAR criteria.










![CLASSICAL DESCRIPTION OF PSA USING THE
DIAGNOSTIC CRITERIA OF MOLL AND WRIGHT
Including 5 clinical patterns:
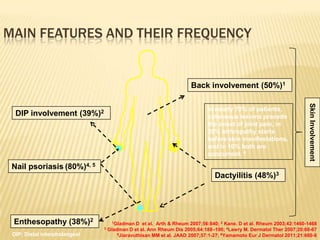
Asymmetric mono-/oligoarthritis (~30% [range 12-70%])1-4
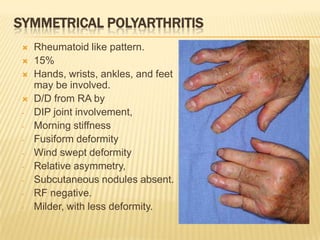
Symmetric polyarthritis (~45% [range 15-65%])1-4
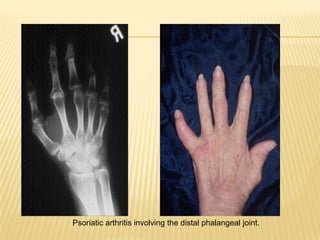
Distal interphalangeal (DIP) joint involvement (~5%)1
Axial (spondylitis and Sacroiliitis) (HLA-B27) (~5%)1,3
Arthritis Mutilans (<5%)1,3
• However patterns may change over time and are therefore not useful for
classification 5
HLA: Human leucocytes antigen
References see notes](https://image.slidesharecdn.com/psoriaticarthropathy-140219140255-phpapp01/85/Psoriatic-arthropathy-14-320.jpg)