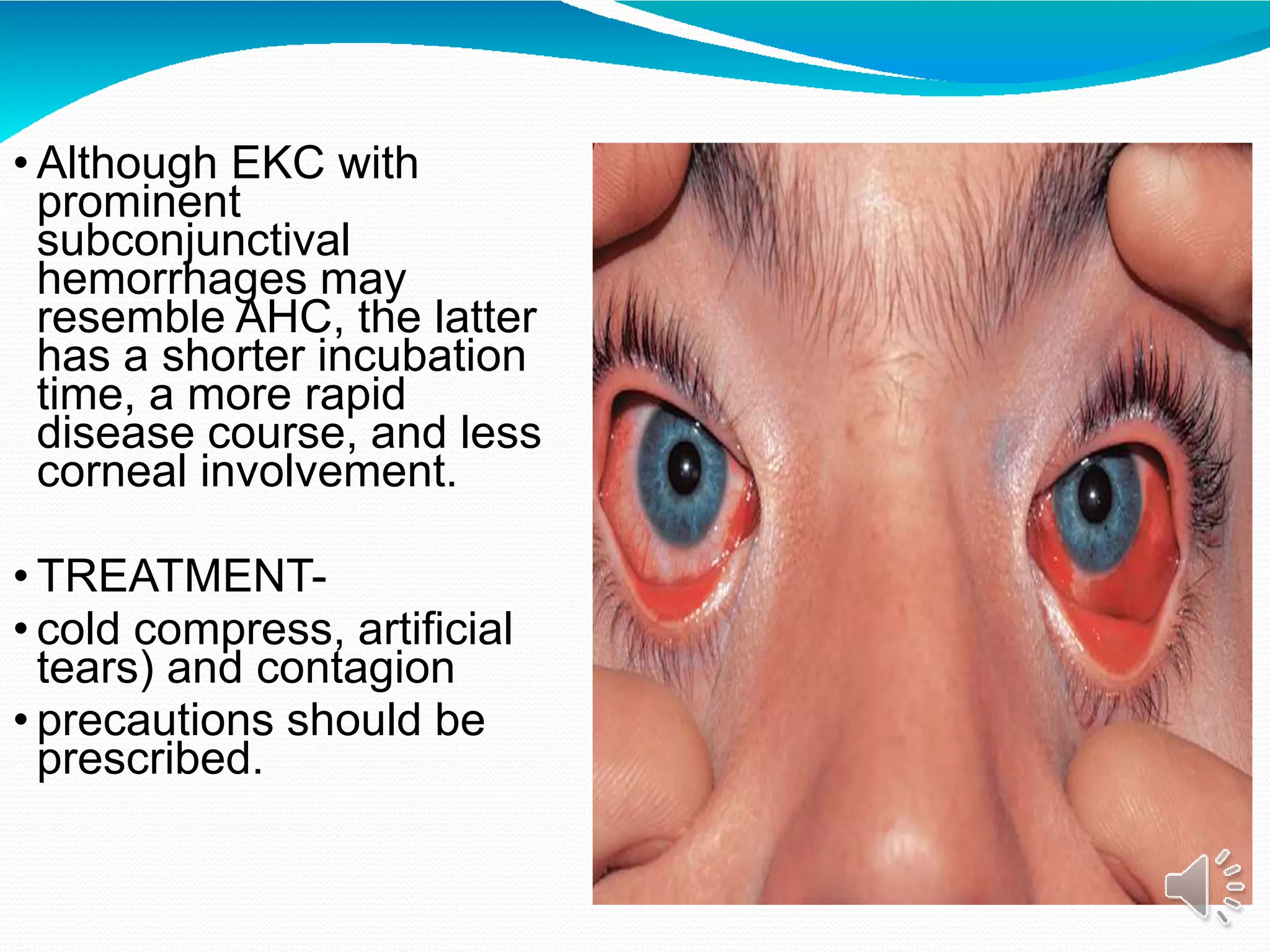
This document summarizes common external ocular infections, with a focus on viral conjunctivitis. It describes the typical causative agents such as adenovirus (in over 90% of cases), herpes simplex virus, and enterovirus. The symptoms of redness, irritation, watering and photophobia are outlined. Signs may include eyelid edema, follicles, papillae, and punctate epithelial keratitis in more severe cases. Treatment focuses on supportive measures like artificial tears and cold compresses.