Here are the three principles of health promotion from the Ottawa Charter:
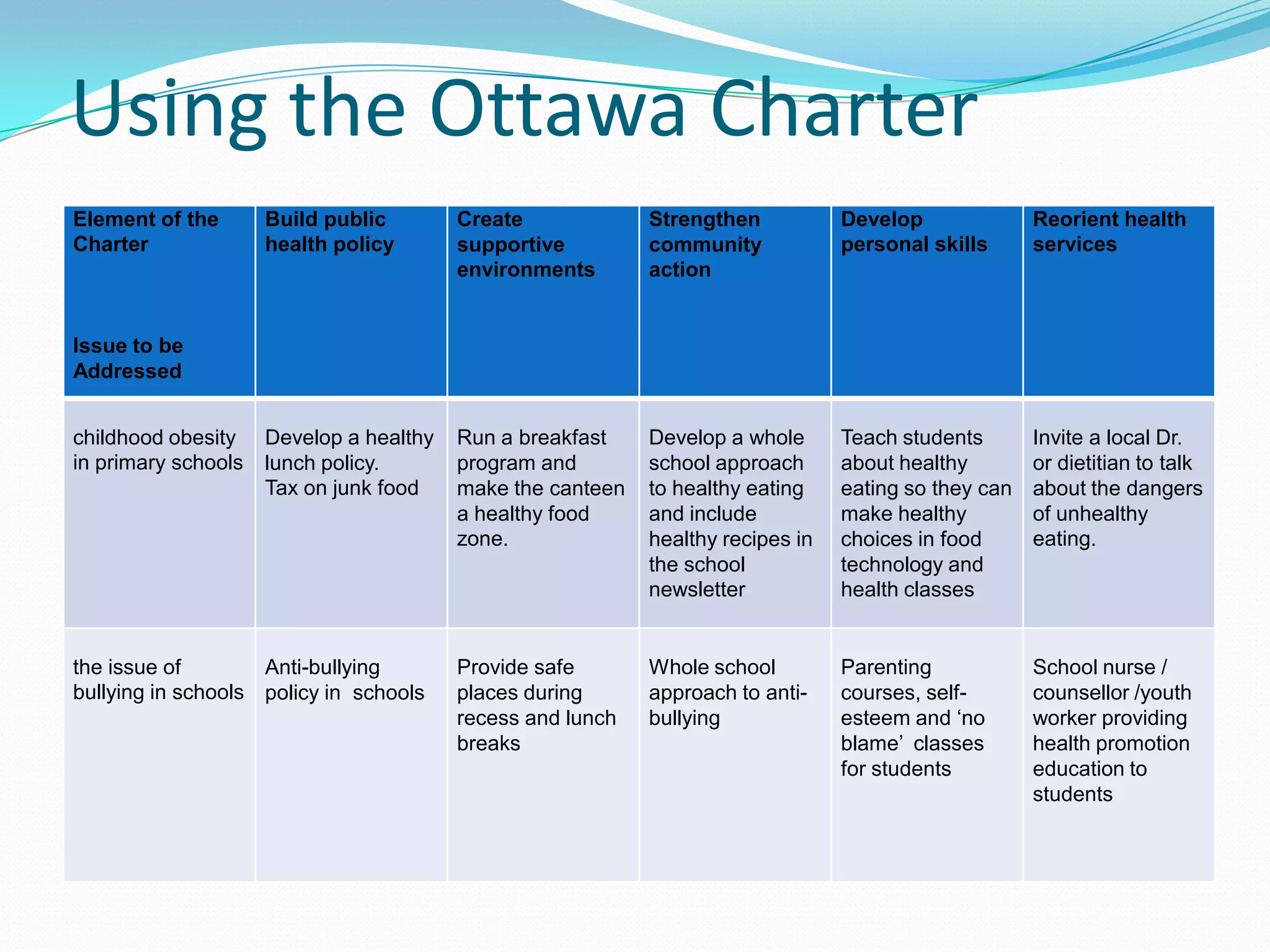
1. Enable - This principle aims to enable people to increase control over their own health and its determinants, and thereby improve health.
2. Mediate - This principle acknowledges that health promotion requires coordinated action by all concerned: by governments, by health and other social and economic sectors, by nongovernmental and voluntary organizations, by local authorities, by industry and by the media.
3. Advocate - This principle aims to advocate for health as a positive concept and fundamental human right. It requires the identification of obstacles to the adoption of healthy public policies in non-health sectors, and ways to remove them.