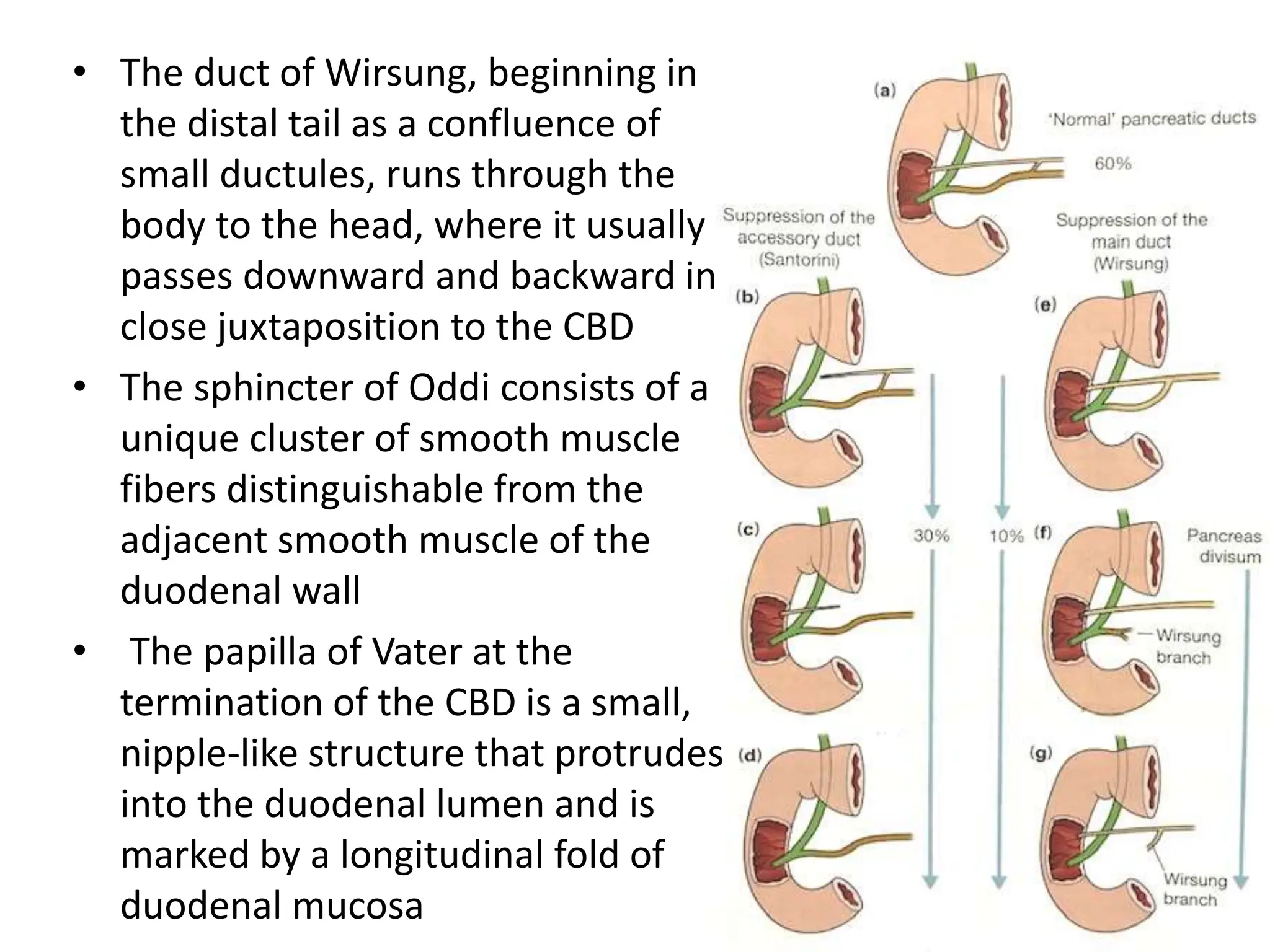
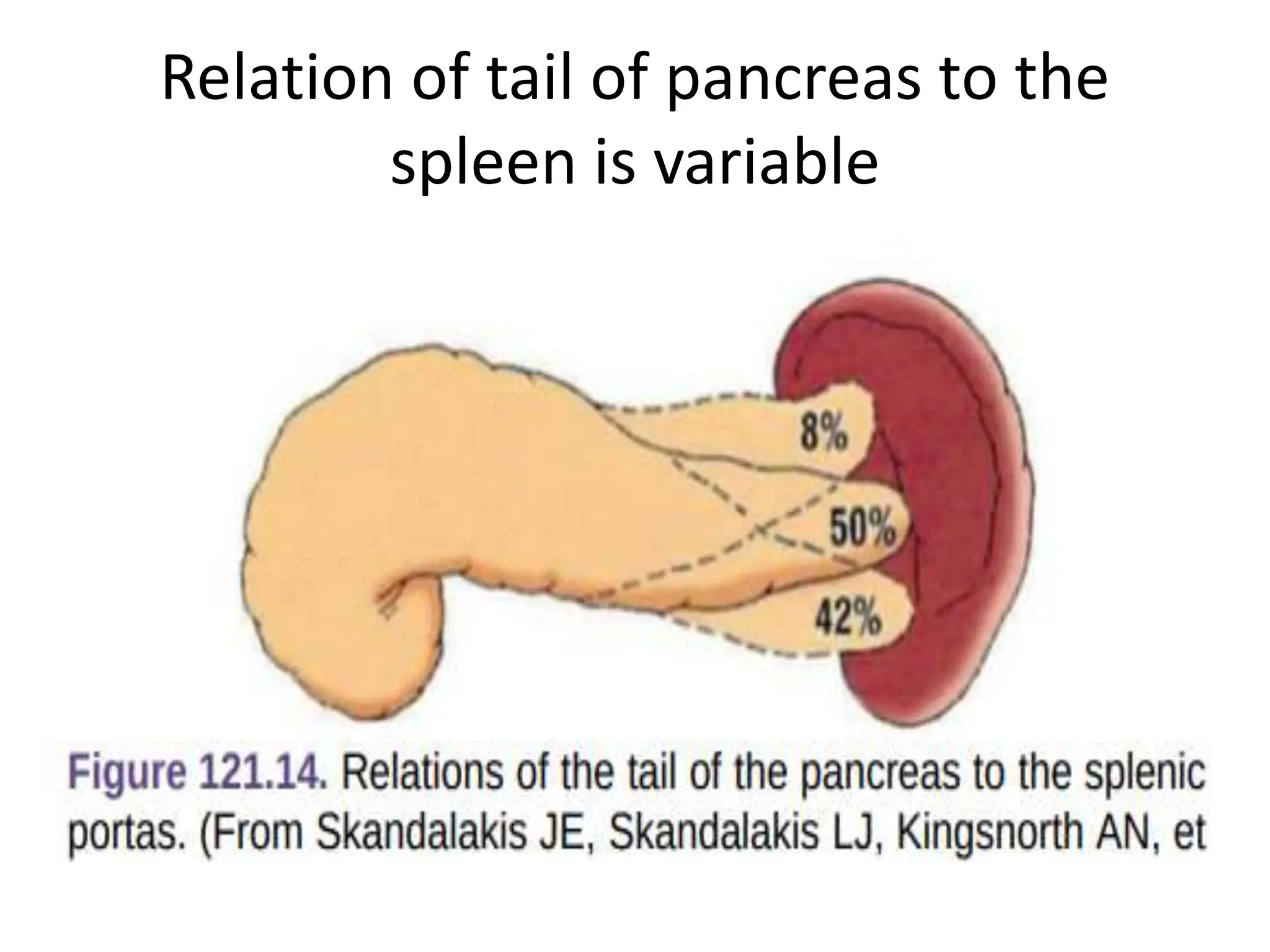
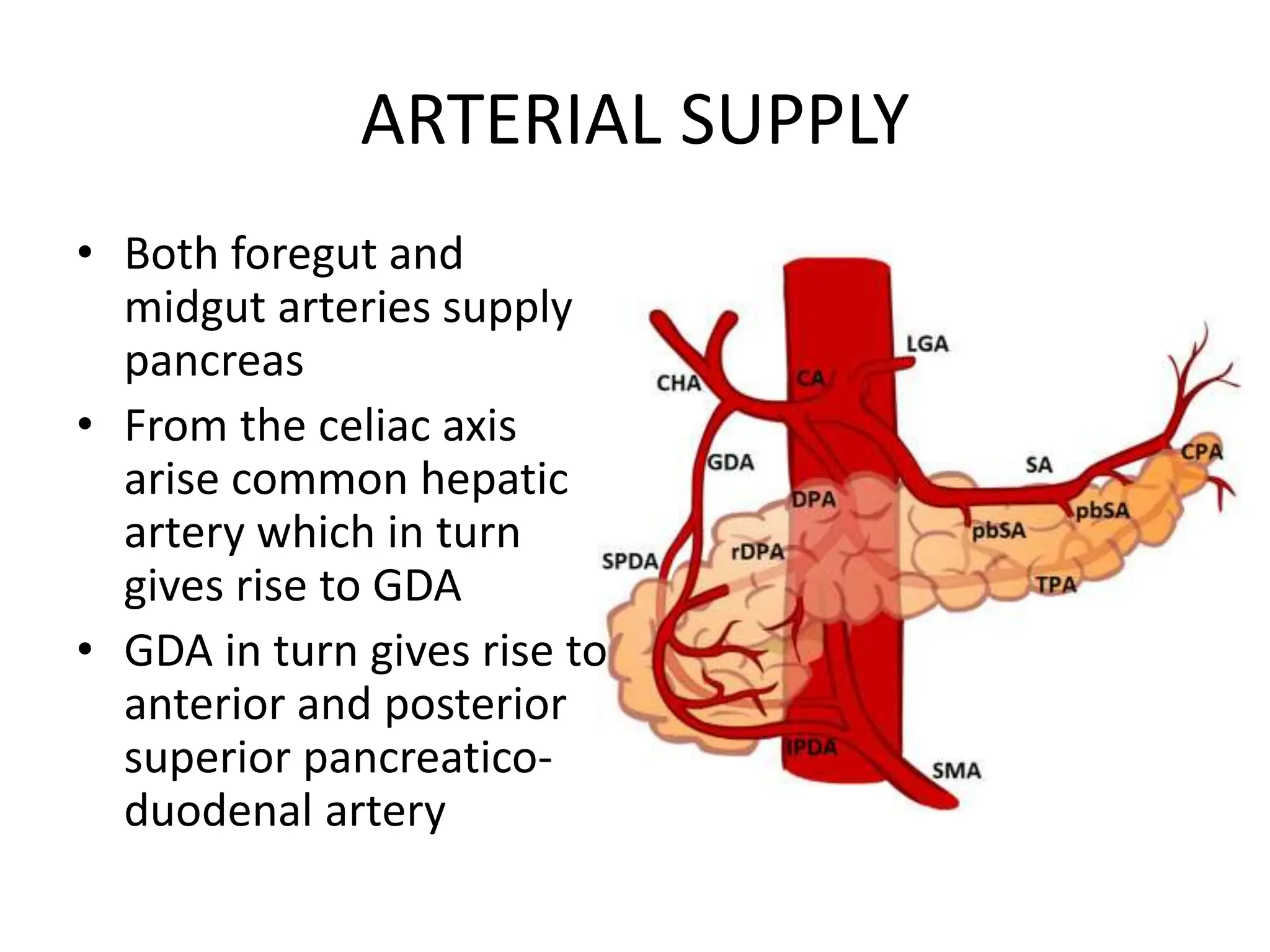
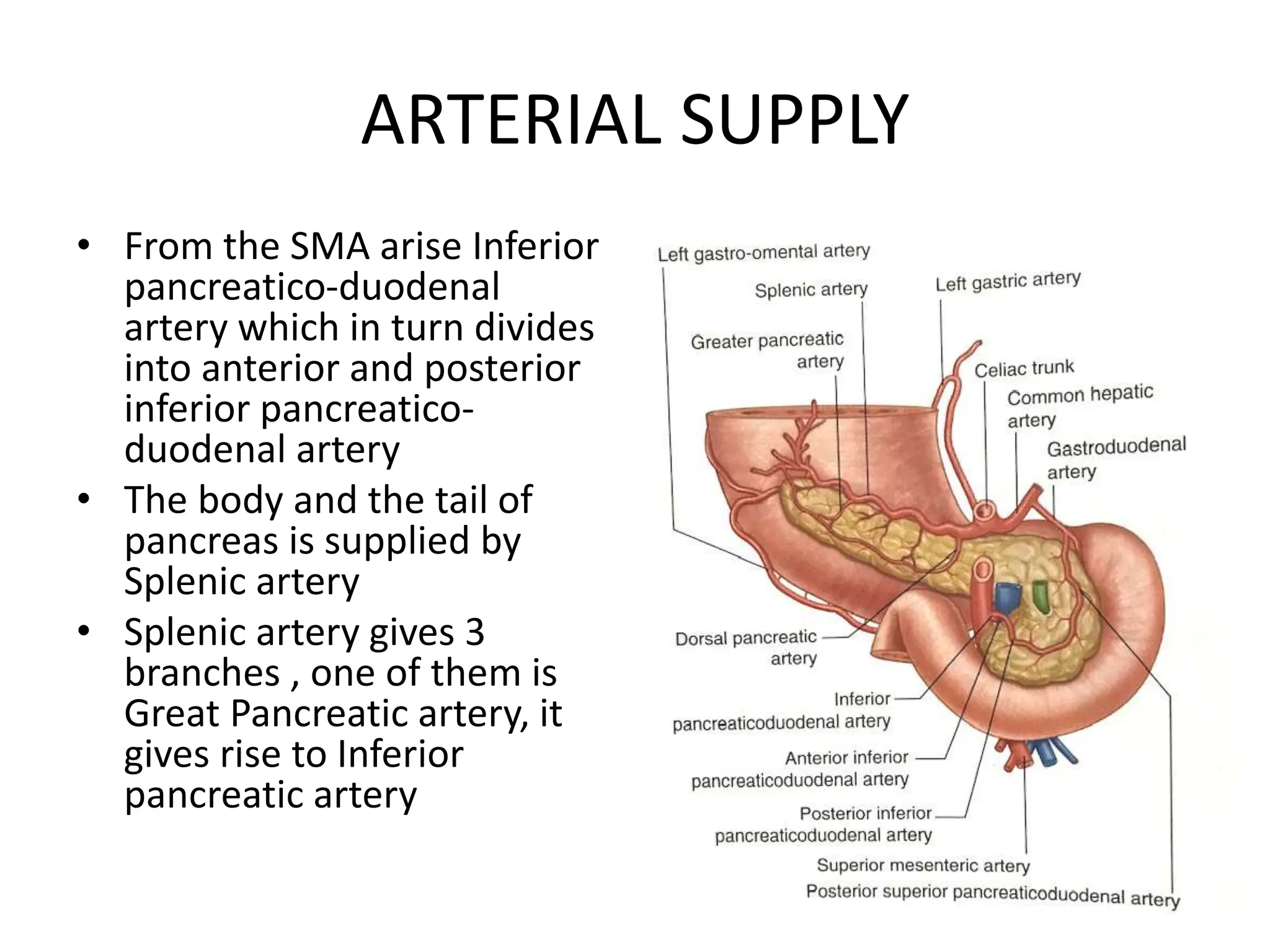
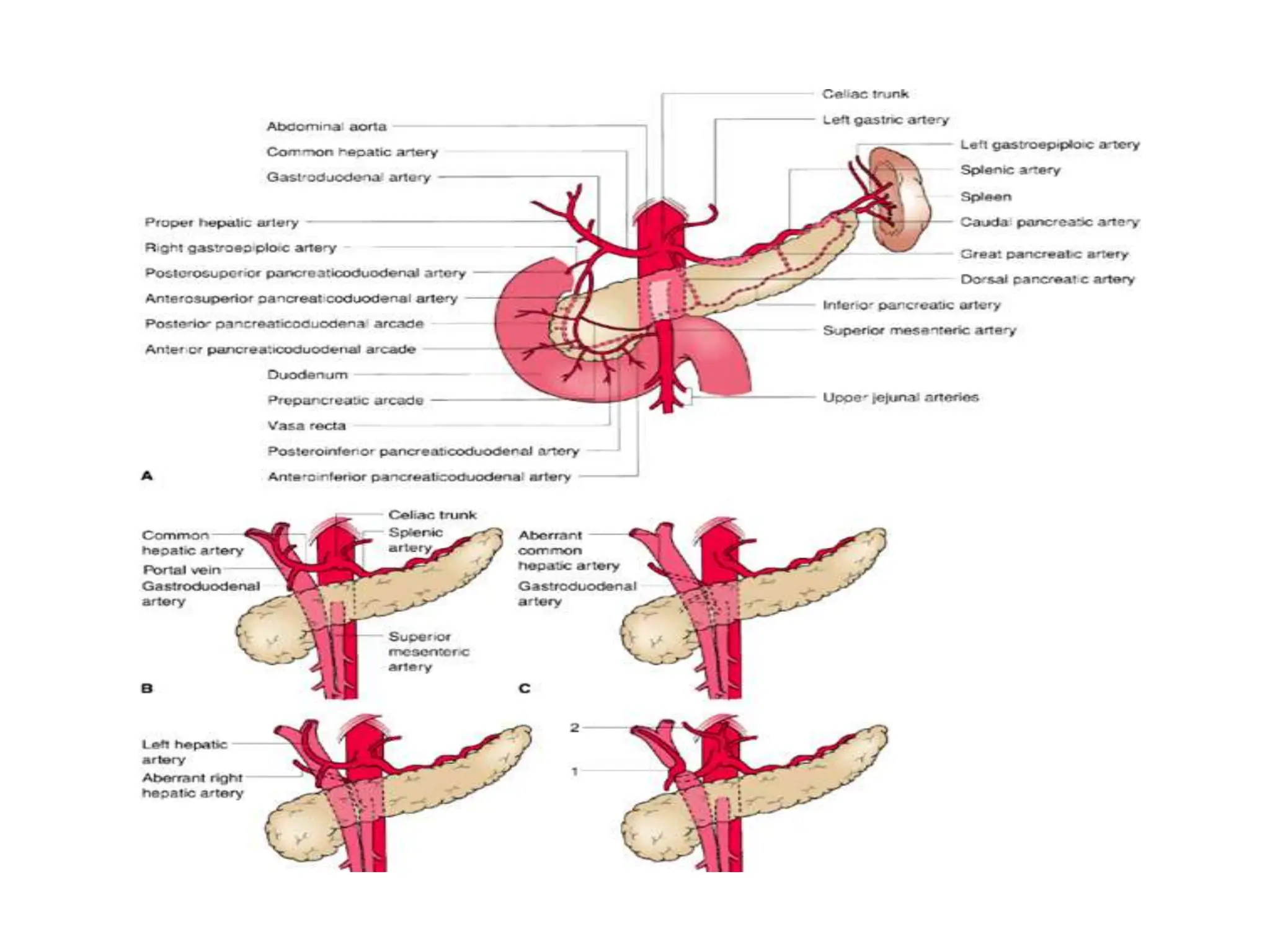
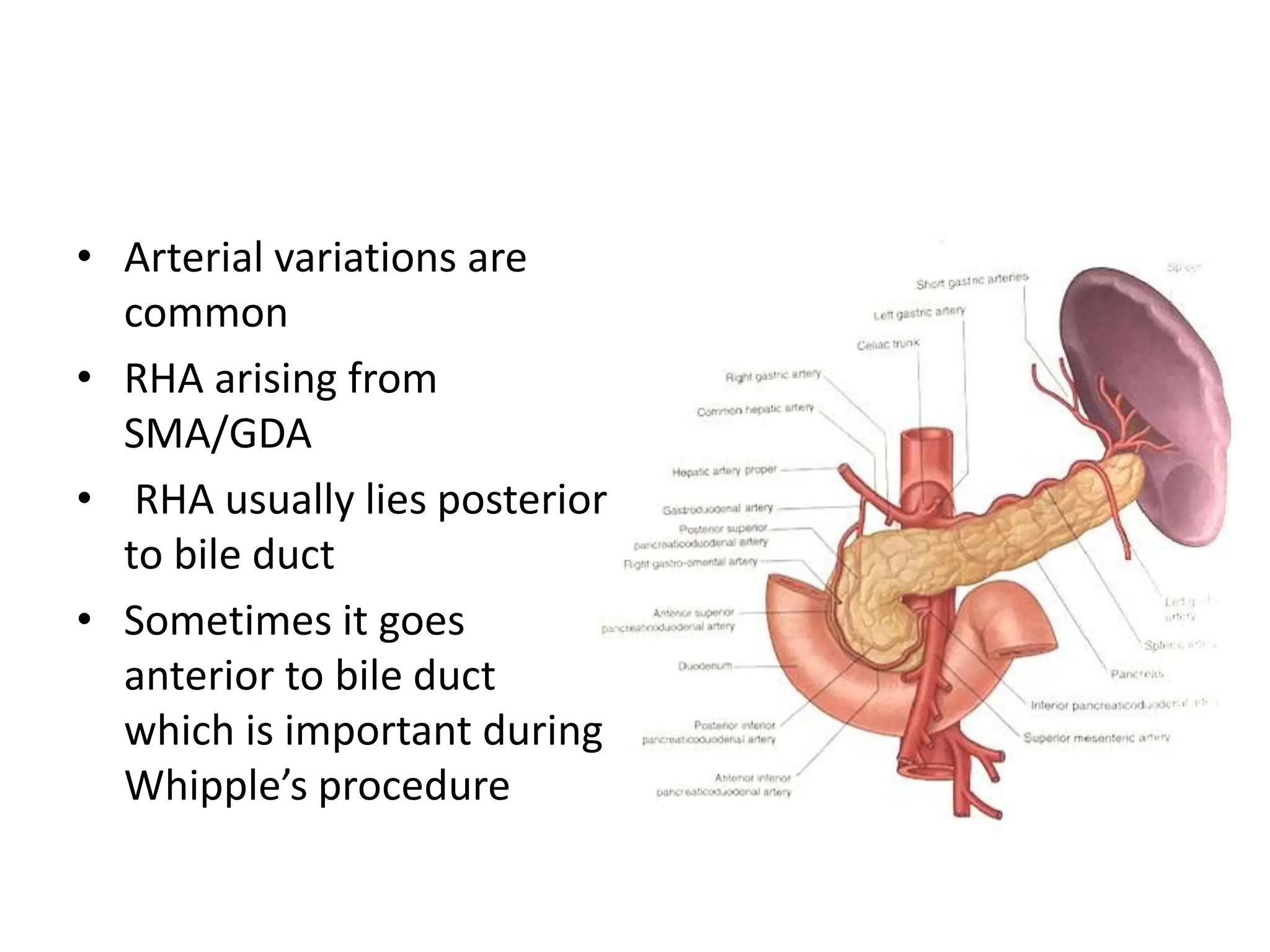
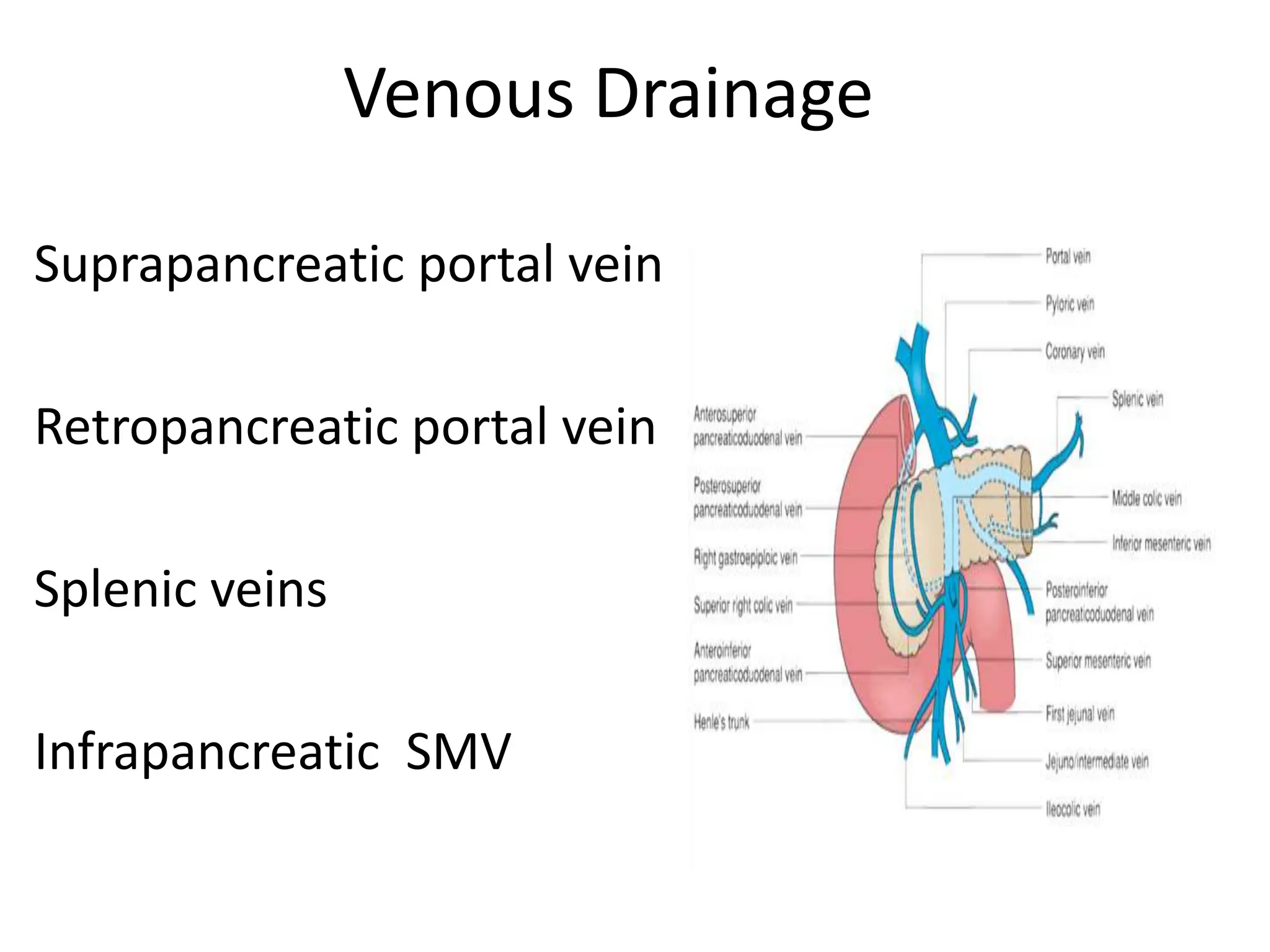
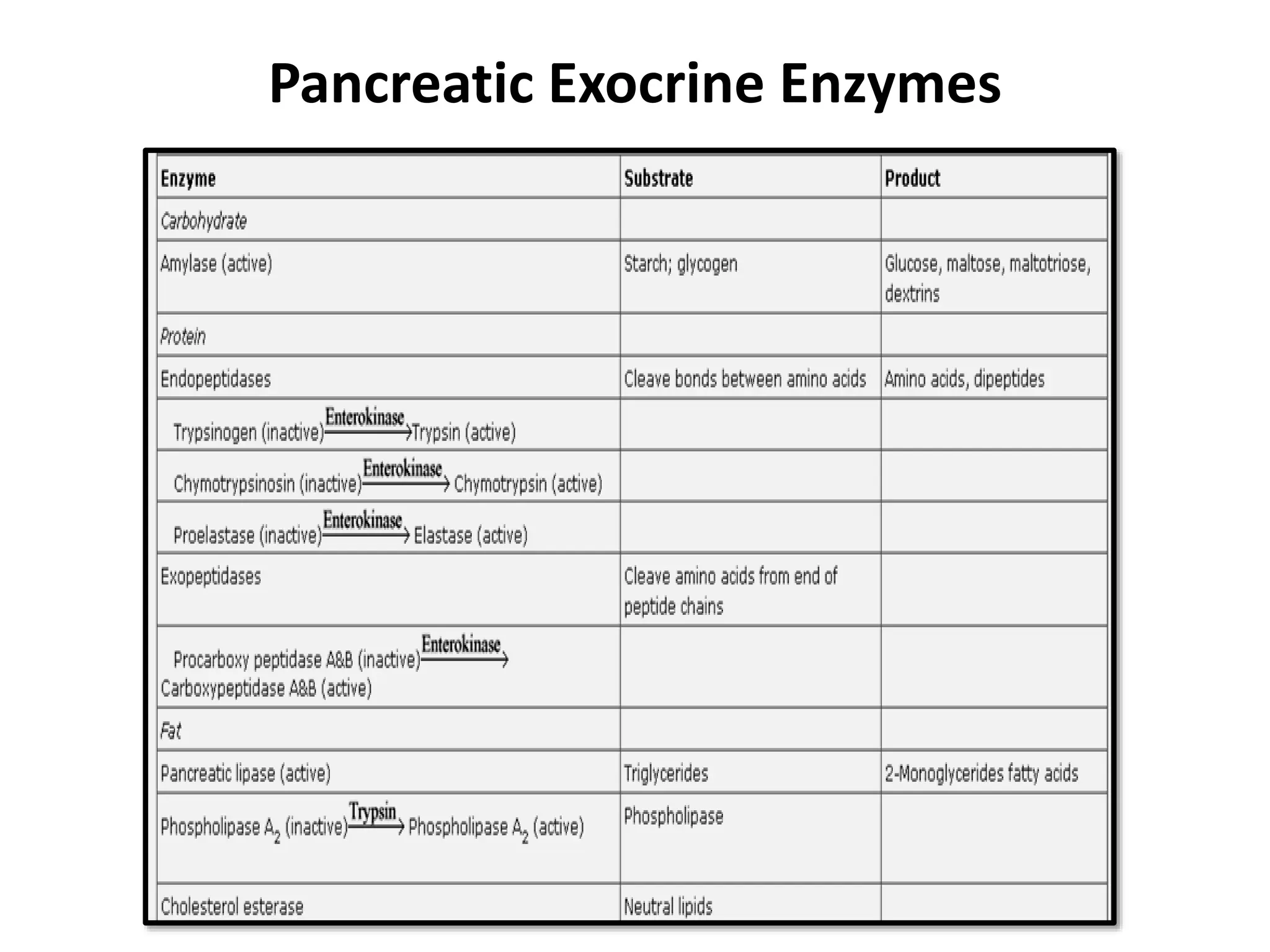
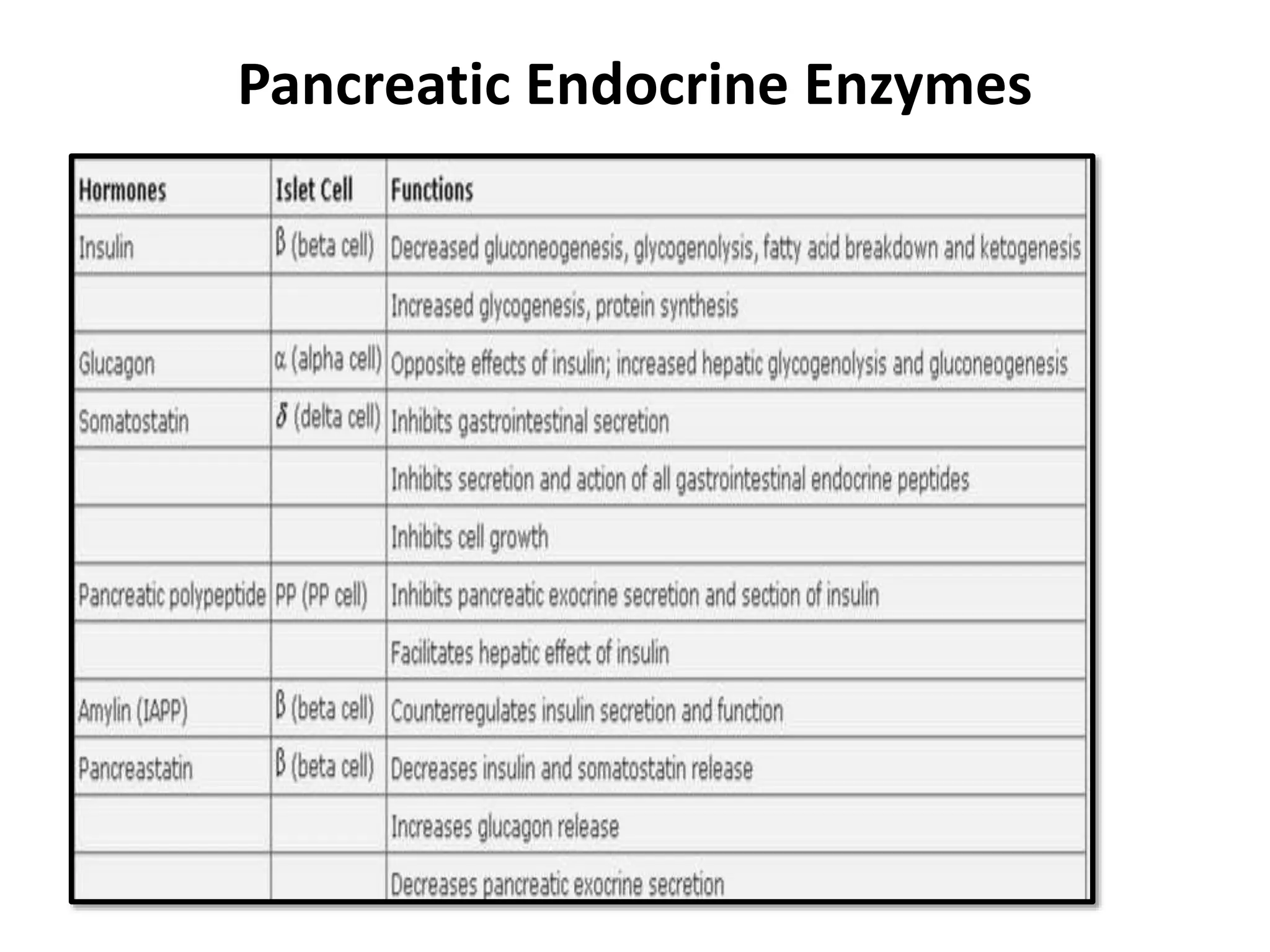
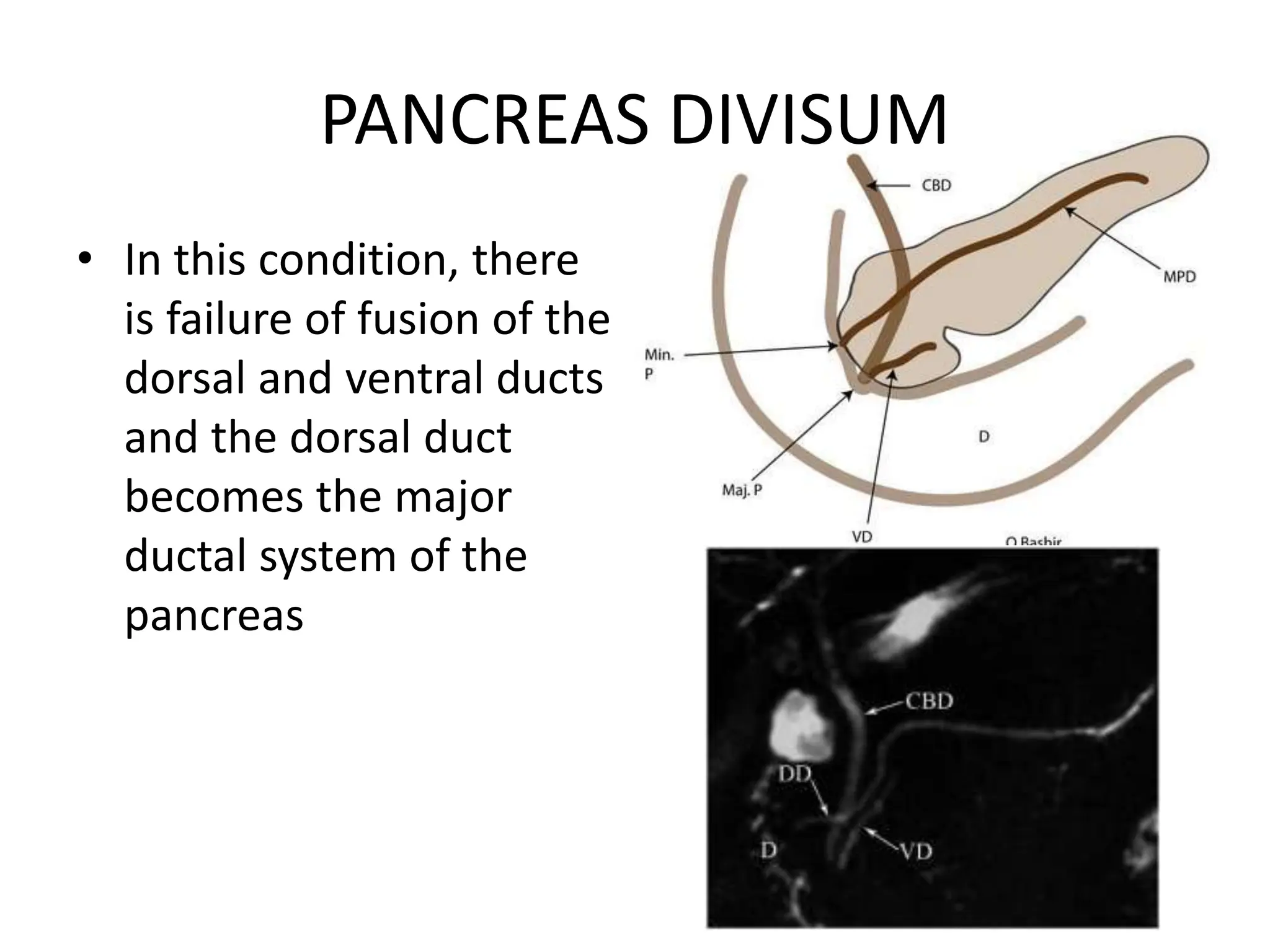
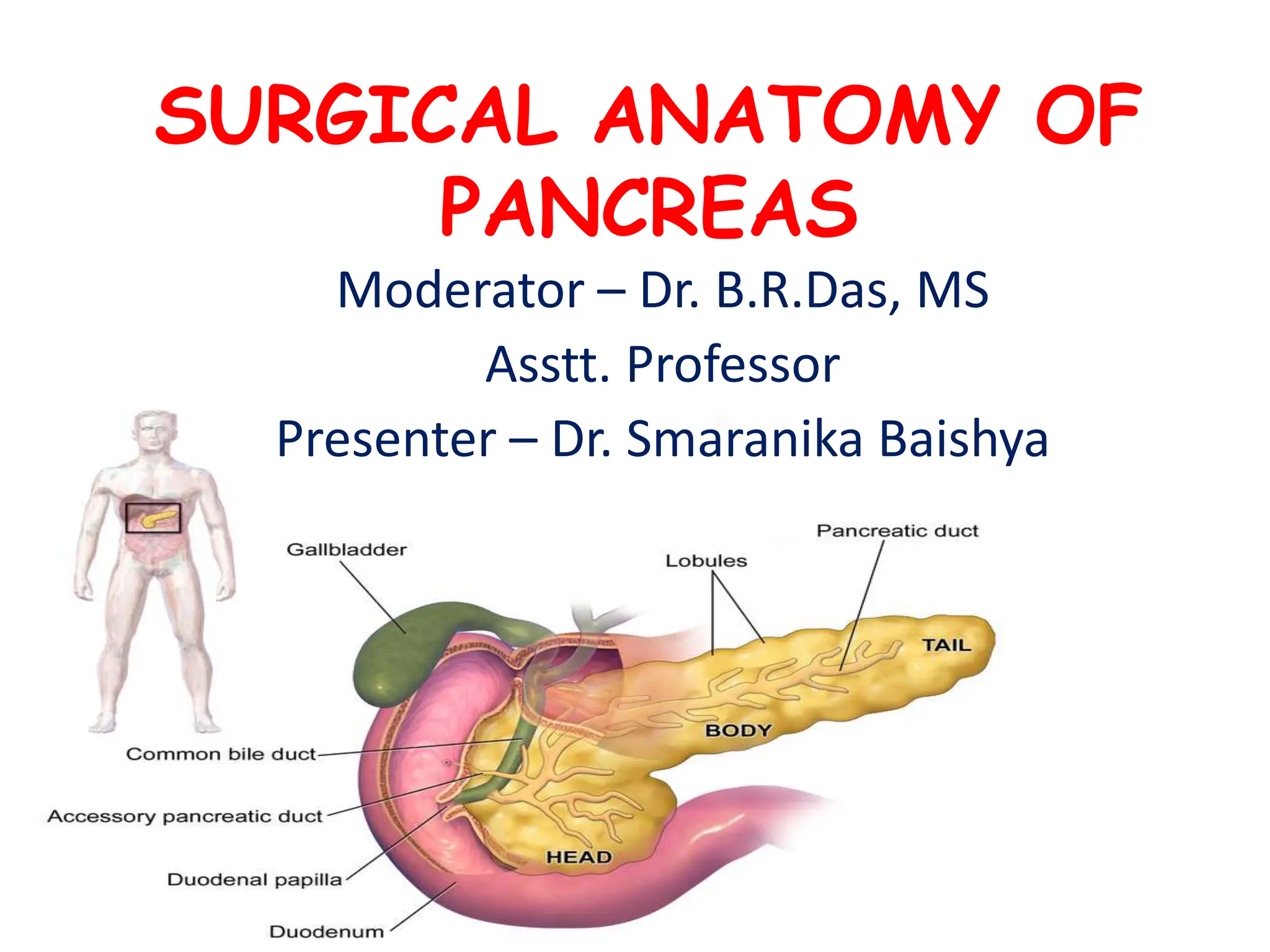
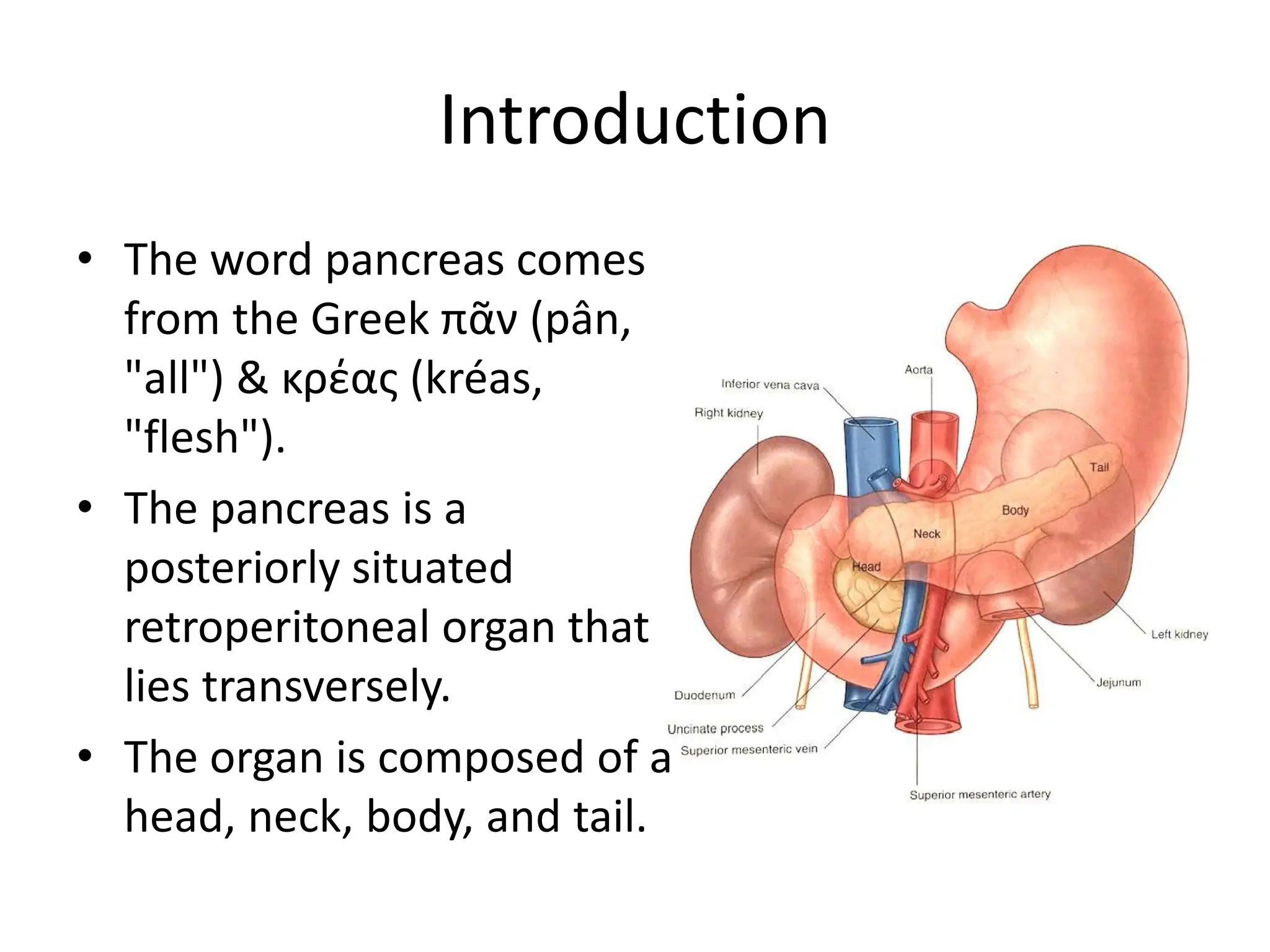
The document outlines the surgical anatomy of the pancreas, detailing its structure, location, embryology, and vascular supply. It discusses the pancreas's relations with surrounding organs and key anatomical features such as the main pancreatic duct and venous drainage. Additionally, it addresses variations, conditions like pancreas divisum and annular pancreas, and the histological structure distinguishing exocrine and endocrine functions.
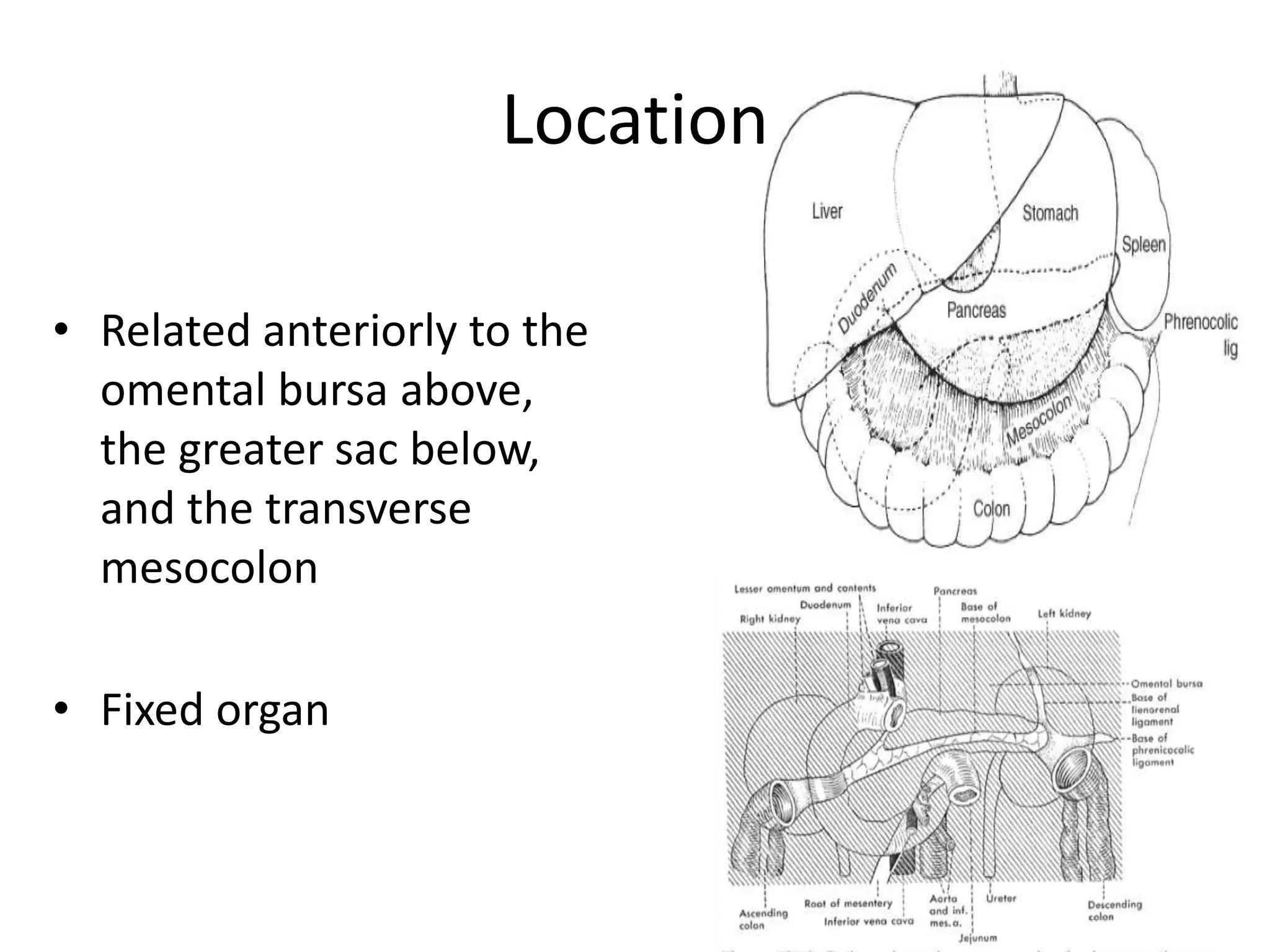



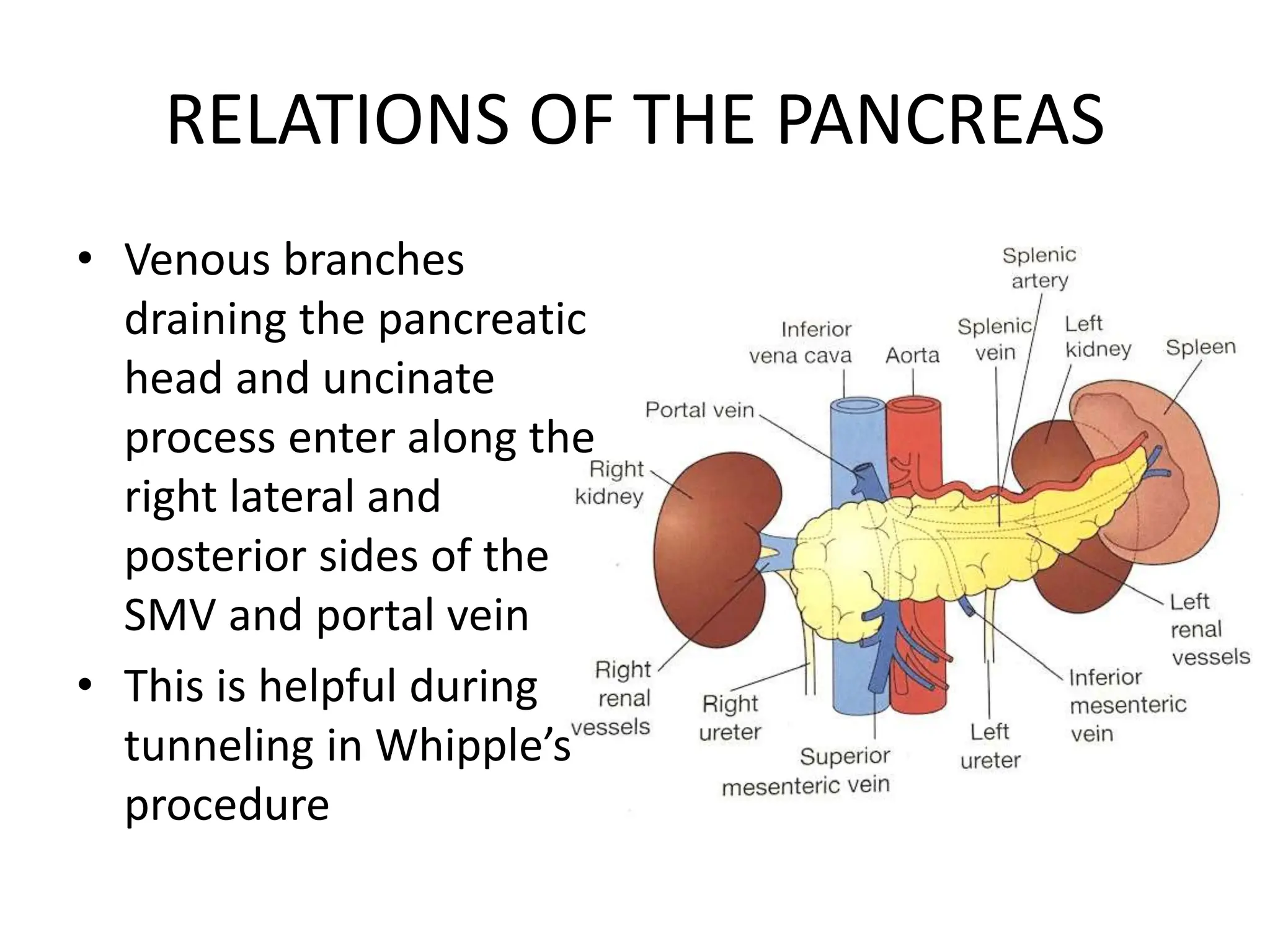

![Embryology
• Carnegie stages are a standardized system of 23 stages
used to provide a unified developmental chronology .
• The pancreas is induced within the endoderm at
Carnegie Stage (CS) 12.
• The pancreatic precursors arise within three locations:
1. the ventral endodermal domain,
2. the VMEL[ventral midline of endoderm lip] (both the
ventral endodermal domain and the VMEL are
common progenitors with the liver), and
3. a dorsal domain to give rise to the dorsal and ventral
pancreatic buds.](https://image.slidesharecdn.com/surgicalanatomyofpancreas-240508171445-7502733c/75/SURGICAL-ANATOMY-OF-PANCREAS-INTRO-pptx-9-2048.jpg)