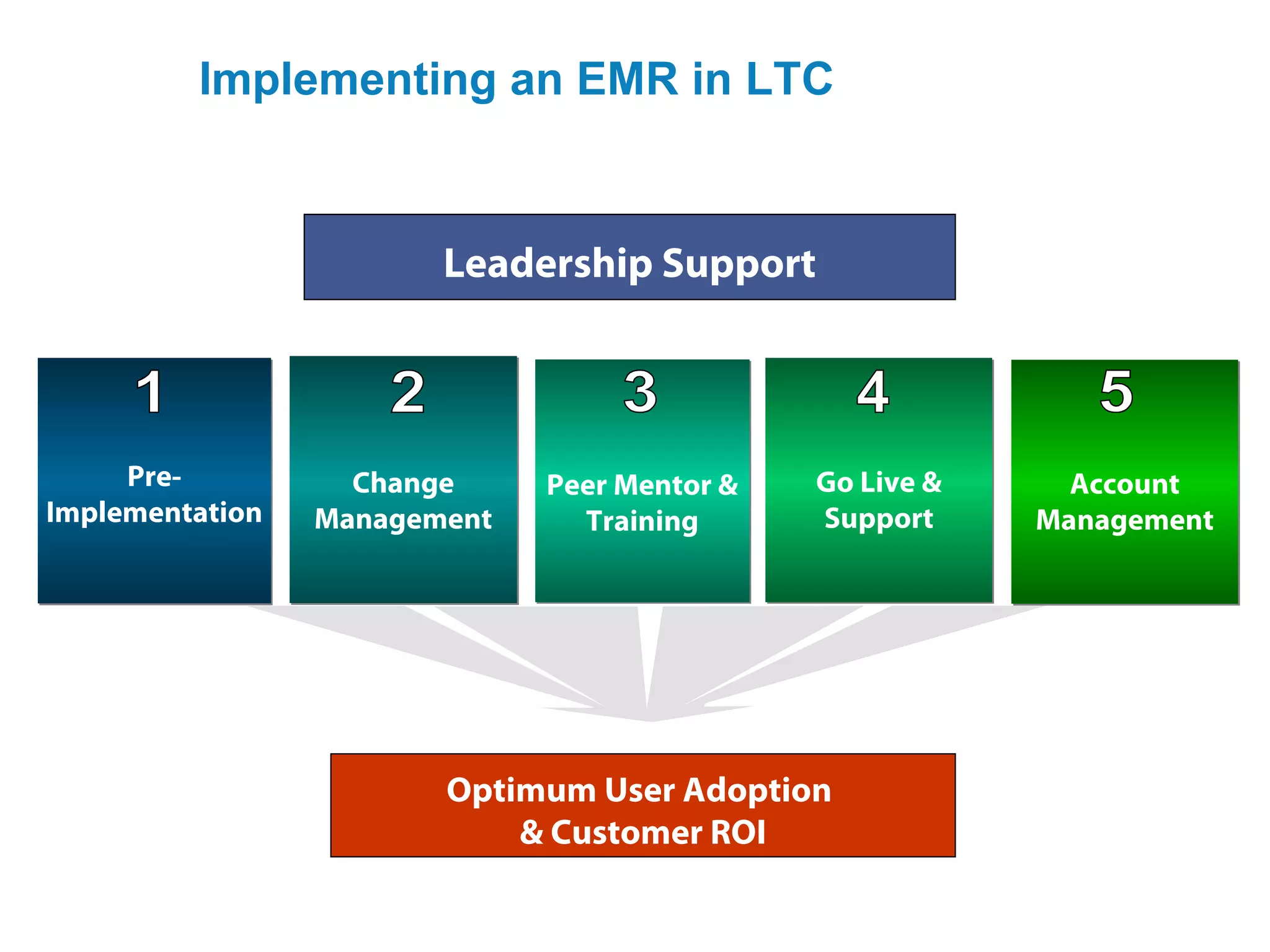
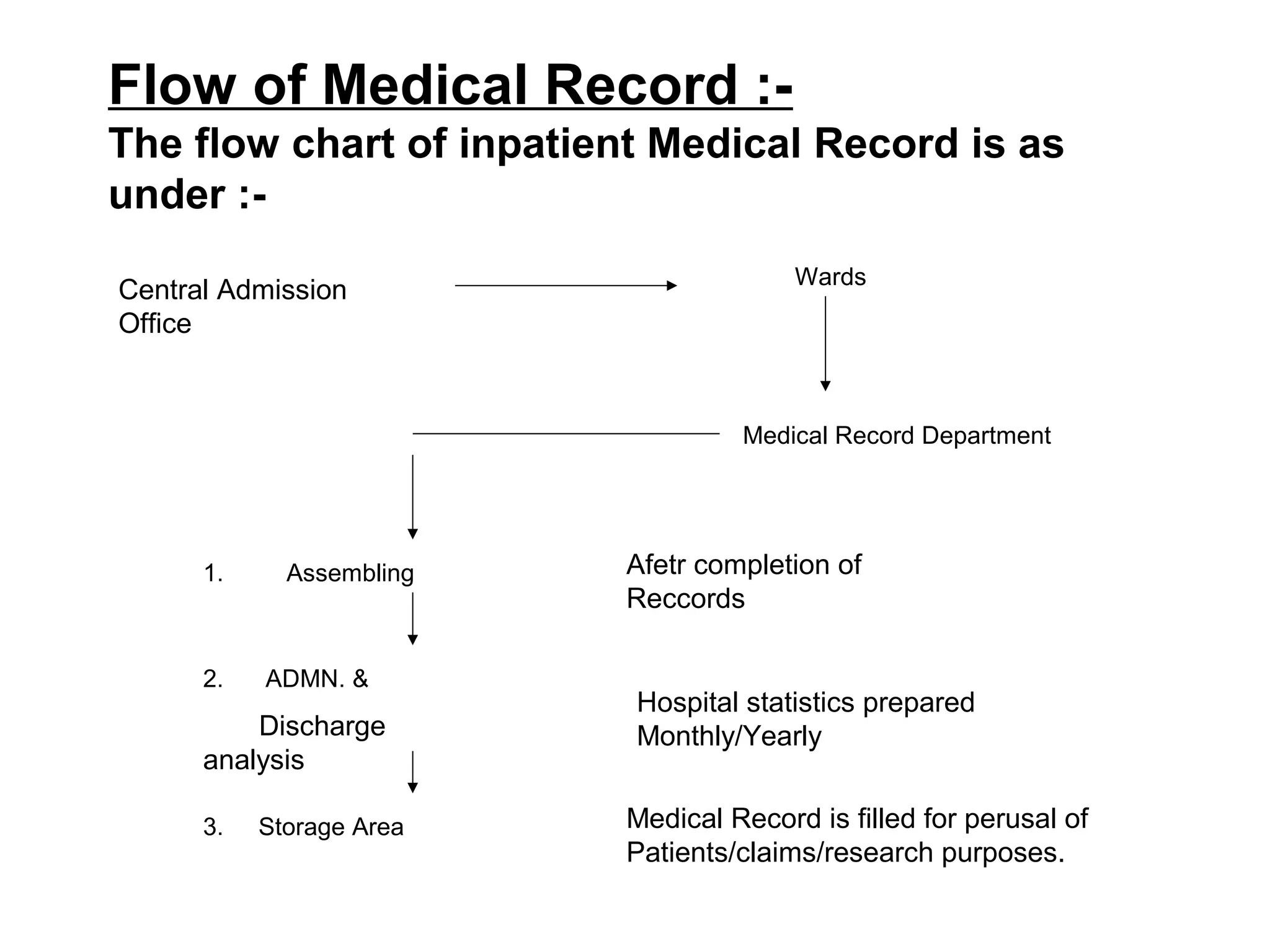
The document discusses guidelines for proper documentation and reporting in healthcare, including maintaining accurate, complete records for communication, education, and legal purposes. It also outlines the different types of reports like change of shift reports, incident reports, and legal reports that are important for monitoring quality of care. Proper documentation in medical records is essential for continuity of care, research, and evaluating health programs.