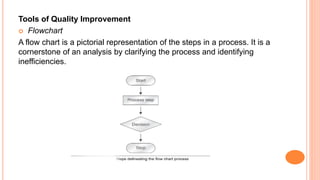
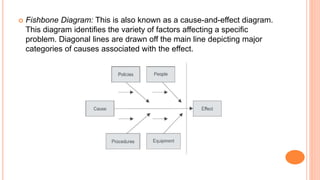
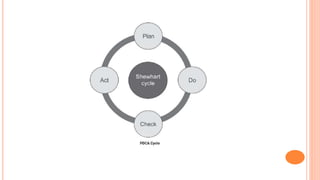
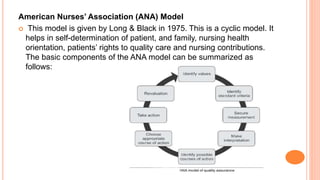
Quality management in healthcare aims to minimize harm and optimize patient outcomes through administration of systems, policies, and processes. It involves continuous improvement efforts to meet expectations of customers (patients and providers), increase effectiveness and efficiency of care, and fulfill ethical obligations. Common models for quality management include the Joint Commission's 10-step process of planning, implementing, evaluating and improving care, and the PDCA (Plan-Do-Check-Act) cycle of establishing objectives, implementing plans, monitoring results, and applying lessons learned.