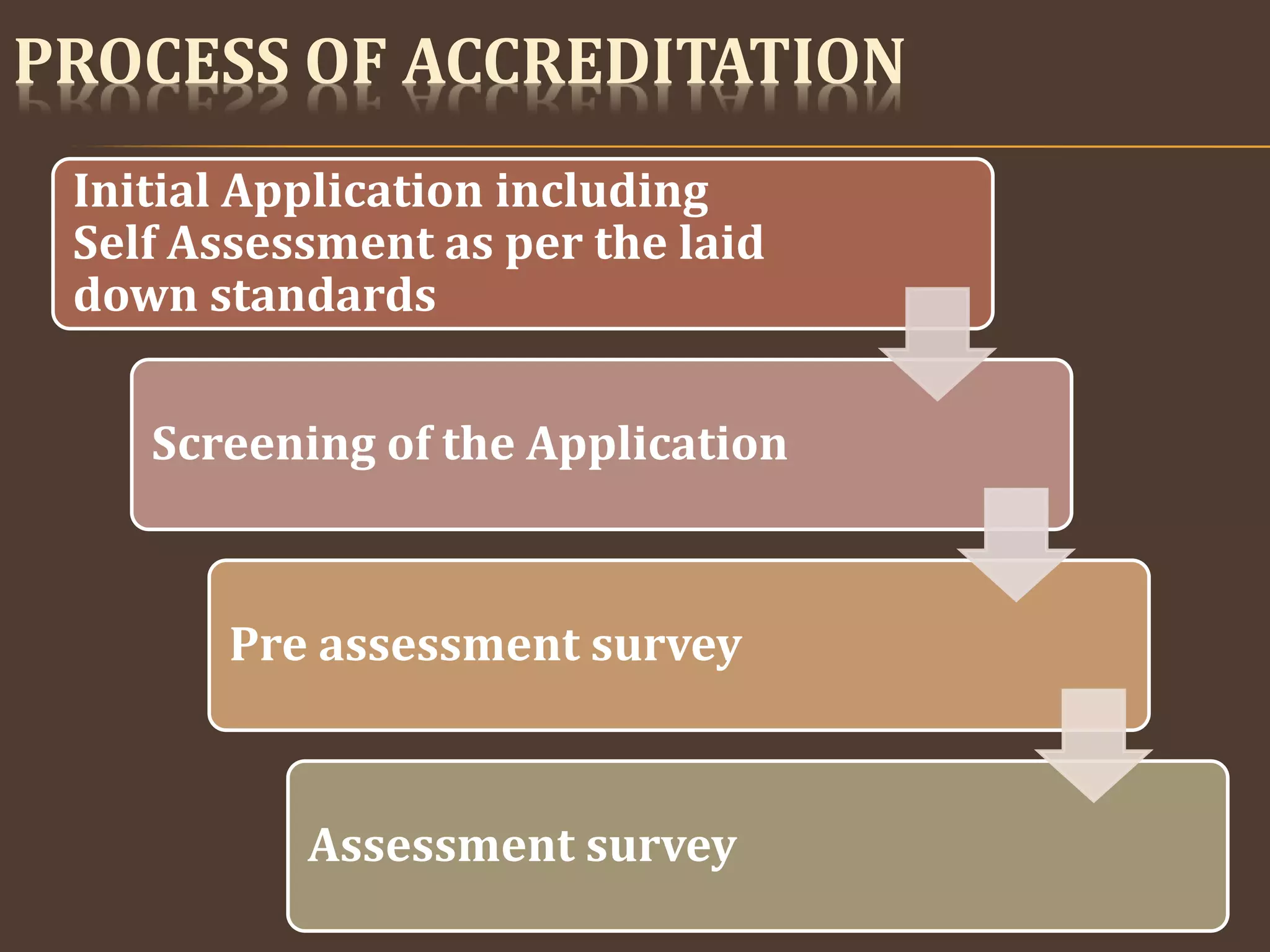
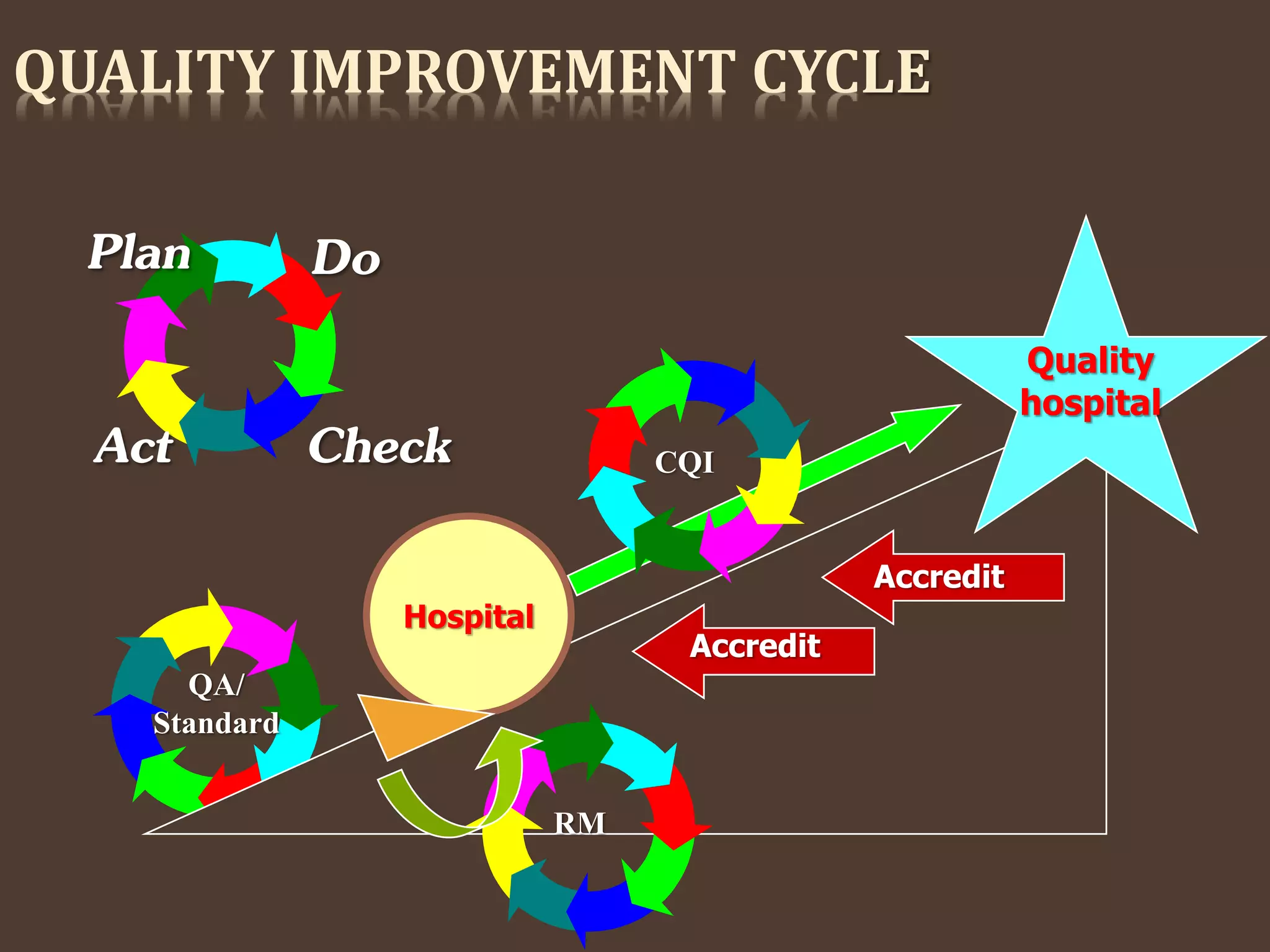
Quality in healthcare refers to adhering to predetermined specifications and standards to meet patient needs. Over time, quality practices evolved from craftsmanship to focusing on processes through thinkers like Shewhart and Deming. Donabedian introduced structure-process-outcome measures for assessing quality. National and international organizations like JCAH, ISO, and NABH were formed to standardize healthcare quality. NABH accreditation involves an application process, onsite assessments, and meeting standards in areas like patient care, management, and information systems to certify high quality care.