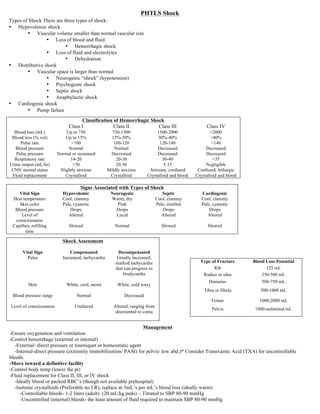
The document provides information on a 2-day PHTLS course, including the course plan, lesson topics, and assessment sequence. It also includes review materials and a pre-test for participants. The goal is to review trauma guidelines and management criteria prior to the course.